## Persistent Weakness in Organophosphate Poisoning: Timing and Pralidoxime Efficacy ### Clinical Context The patient has: - **Resolved muscarinic signs:** normal HR, BP, pupils dilated and reactive → atropine worked - **Persistent nicotinic weakness:** no spontaneous respiration, absent train-of-four response - **Timeline:** 6 hours post-ingestion, antidotes given in ED This dissociation between muscarinic recovery and nicotinic persistence is the hallmark of **pralidoxime failure due to delayed administration**. ### Pralidoxime: Mechanism and Time Window **Key Point:** Pralidoxime reactivates acetylcholinesterase by nucleophilic attack on the phosphorylated enzyme. However, this reactivation is **time-dependent** and becomes progressively less effective as the organophosphate-enzyme complex "ages." ```mermaid flowchart TD A[Organophosphate + Acetylcholinesterase]:::outcome --> B{Time Since Exposure?}:::decision B -->|0-2 hours| C[Pralidoxime highly effective]:::action B -->|2-24 hours| D[Pralidoxime moderately effective]:::action B -->|>24 hours| E[Pralidoxime often ineffective]:::urgent C --> F[Enzyme reactivated, weakness resolves]:::outcome D --> G[Partial reactivation, variable recovery]:::outcome E --> H[Irreversible enzyme inhibition<br/>Prolonged mechanical ventilation needed]:::urgent ``` ### Why Pralidoxime Failed in This Case 1. **6-hour delay:** The patient ingested organophosphate and received pralidoxime 6 hours later. While still within the theoretical window, the enzyme complex has partially undergone **"aging"** — the phosphorus-enzyme bond becomes increasingly resistant to nucleophilic attack. 2. **Nicotinic effects persist:** Acetylcholine accumulation at the neuromuscular junction causes: - Initial depolarization block (fasciculations) - Prolonged depolarization → desensitization of nicotinic receptors - Functional neuromuscular blockade (cannot generate action potentials) 3. **Atropine does NOT reverse nicotinic effects:** Atropine only blocks muscarinic receptors (salivation, bronchospasm, bradycardia). It has NO effect on nicotinic blockade at the neuromuscular junction. **High-Yield:** The **muscarinic-nicotinic dissociation** (normal vitals + severe weakness) indicates pralidoxime failure, not inadequate dosing. ### Intermediate Syndrome **Clinical Pearl:** Intermediate syndrome (IMS) is a distinct entity that occurs 24–96 hours post-exposure in ~50% of organophosphate poisonings: - Develops AFTER initial recovery from acute cholinergic crisis - Characterized by proximal muscle weakness, respiratory failure, cranial nerve palsies - Mechanism: unclear (possibly acetylcholine receptor desensitization, not enzyme reactivation failure) - This patient is only 6 hours post-exposure, so IMS has not yet developed ### Management of Persistent Nicotinic Weakness 1. **Continue mechanical ventilation** until neuromuscular function recovers (may take days to weeks) 2. **Repeat pralidoxime** doses (500 mg IV every 4–6 hours) for up to 24–48 hours, though efficacy is limited 3. **Avoid depolarizing agents** (succinylcholine) — risk of hyperkalemia and prolonged paralysis 4. **Monitor train-of-four** to assess neuromuscular recovery 5. **Supportive care:** nutrition, DVT prophylaxis, ICU care **Warning:** Do NOT assume the weakness is from sedation alone — organophosphate-induced neuromuscular blockade is real and requires time to resolve. [cite:Harrison 21e Ch 473; Poisoning & Drug Overdose (Olson) Ch 12] 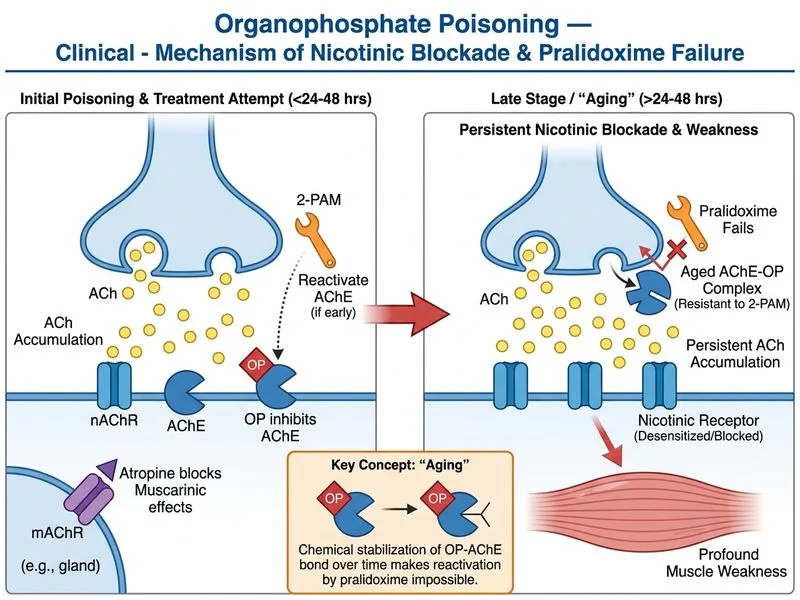
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.