## Diagnosis: Osteoarthritis ### Clinical Features Supporting OA **Key Point:** Osteoarthritis is a degenerative joint disease characterized by progressive cartilage loss, osteophyte formation, and subchondral bone changes. ### Diagnostic Criteria Met | Feature | Finding | Significance | |---------|---------|---------------| | **Age & onset** | 62 years, 3-year progressive course | OA typically affects older adults; gradual onset | | **Morning stiffness** | 15–20 minutes | Brief stiffness typical of OA (RA: >1 hour) | | **Joint involvement** | Bilateral knees (weight-bearing) | OA favours weight-bearing joints | | **Crepitus** | Present on passive motion | Cartilage irregularity and osteophytes | | **Inflammatory markers** | ESR 12, CRP 2 (normal) | OA is non-inflammatory; RA would show elevation | | **X-ray findings** | Joint space narrowing, osteophytes, sclerosis | Pathognomonic for OA | ### Pathophysiology 1. **Cartilage degradation** → loss of articular surface 2. **Osteophyte formation** → bone remodelling at joint margins 3. **Subchondral sclerosis** → bone thickening beneath cartilage 4. **Synovial inflammation** (mild) → crepitus and effusion **High-Yield:** The combination of **normal inflammatory markers + radiographic osteophytes + weight-bearing joint involvement + brief morning stiffness** is diagnostic of primary OA. **Clinical Pearl:** Bilateral knee OA in a 62-year-old woman is extremely common; it is the leading cause of disability in older adults in India. ### Why OA, Not Other Diagnoses? - **RA:** Would show prolonged morning stiffness (>1 hour), elevated ESR/CRP, symmetrical small joint involvement (hands), and rheumatoid factor positivity. - **SLE:** Would present with systemic features (rash, photosensitivity, renal involvement), positive ANA, and low complement levels. - **AS:** Would show axial spine involvement, HLA-B27 positivity, and inflammatory markers elevation. 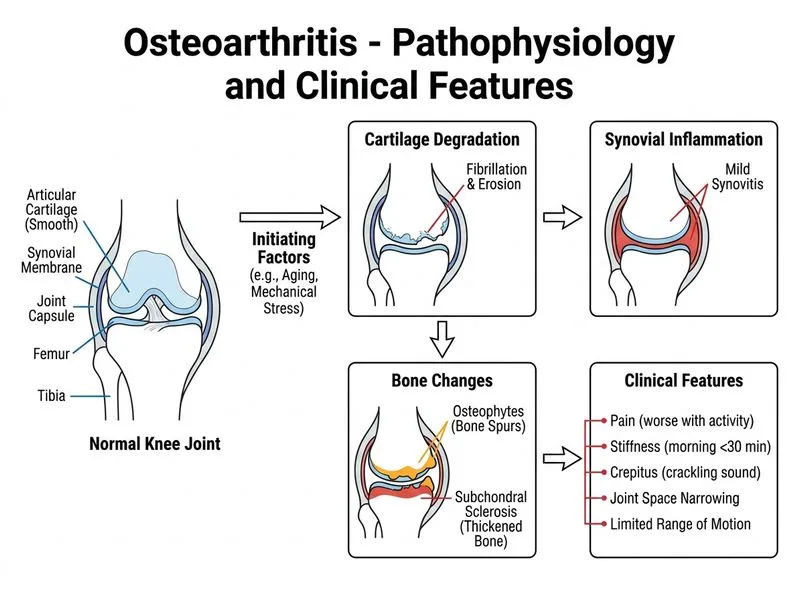
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.