## Clinical Diagnosis: Osteomalacia ### Key Clinical Features **Key Point:** Osteomalacia is defective mineralization of the organic bone matrix in adults, presenting with bone pain, muscle weakness, and pathological fractures. This patient presents with the classic triad of osteomalacia: 1. **Bone pain and tenderness** (diffuse, worse with weight-bearing) 2. **Proximal muscle weakness** (due to hypocalcemia and vitamin D deficiency effects on muscle) 3. **Pathological fractures** (recurrent, with minimal trauma) ### Laboratory Findings | Parameter | This Patient | Normal | Interpretation | |-----------|--------------|--------|----------------| | Serum calcium | 7.8 mg/dL | 8.5–10.5 | ↓ Hypocalcemia | | Serum phosphate | 2.1 mg/dL | 2.5–4.5 | ↓ Hypophosphatemia | | Alkaline phosphatase | 156 U/L | 30–120 | ↑ Elevated (bone turnover) | | 25-OH vitamin D | 12 ng/mL | >30 | ↓ Severe deficiency | | PTH | Expected ↑ | — | Secondary hyperparathyroidism | **High-Yield:** The **25-hydroxyvitamin D level of 12 ng/mL** is diagnostic. Osteomalacia is defined as 25-OH vitamin D <20 ng/mL (or <50 nmol/L). ### Radiological Findings **Key Point:** **Looser's zones** (pseudofractures or Looser's lines) are pathognomonic for osteomalacia. These are: - Transverse radiolucent bands perpendicular to the long axis of bone - Represent areas of incomplete mineralization - Most commonly seen in pelvis, femur, tibia, and ribs - Disappear with vitamin D treatment ### Pathophysiology ```mermaid flowchart TD A[Vitamin D deficiency<br/>Low sun exposure + poor diet]:::action --> B[↓ 1,25-dihydroxyvitamin D]:::outcome B --> C[↓ Intestinal Ca²⁺ absorption]:::outcome C --> D[Hypocalcemia]:::urgent D --> E[↑ PTH secretion]:::outcome E --> F[↑ Bone resorption + ↑ Alkaline phosphatase]:::outcome F --> G[Defective mineralization<br/>Osteomalacia]:::outcome G --> H[Bone pain, muscle weakness,<br/>pathological fractures]:::urgent ``` ### Risk Factors in This Patient - **Minimal sun exposure** (cultural practices → reduced cutaneous vitamin D synthesis) - **Low dietary calcium and vitamin D** (cereal-based diet, minimal dairy) - **Female gender** (higher prevalence of osteomalacia in women) - **Geographic location** (rural Maharashtra, limited sunlight access) **Clinical Pearl:** Osteomalacia is endemic in parts of India, particularly in women with restricted outdoor exposure and low dietary vitamin D intake. ### Differential Exclusion **Why not osteoporosis?** Osteoporosis presents with normal or elevated calcium and phosphate; it does NOT cause hypocalcemia, hypophosphatemia, or elevated alkaline phosphatase. Looser's zones are absent. **Why not hypophosphatemic rickets?** This is an inherited disorder (X-linked hypophosphatemia) presenting in childhood with growth retardation and dental abnormalities. It does NOT present acutely in a 38-year-old adult with environmental risk factors. **Why not Paget's disease?** Paget's presents with localized bone deformity, elevated alkaline phosphatase, and normal calcium/phosphate. It does NOT cause diffuse hypocalcemia or Looser's zones. 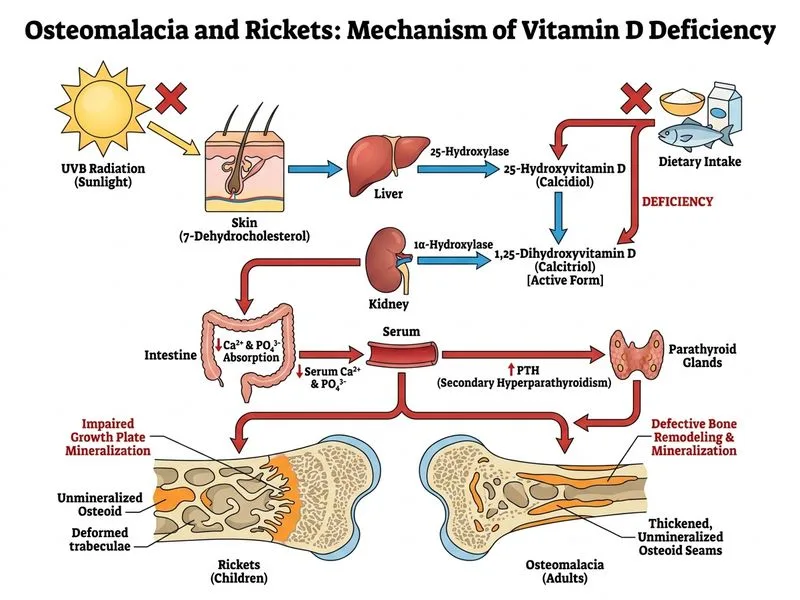
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.