## Diagnosis: Tuberculous Osteomyelitis ### Clinical and Microbiological Reasoning **Key Point:** The isolation of *Mycobacterium tuberculosis* from pus culture of a draining sinus tract arising from a lytic bone lesion in the distal femur is diagnostic of **tuberculous osteomyelitis**. The lesion is primarily in the bone (medial femoral condyle/distal femur metaphysis), not in the joint synovium, making this osteomyelitis — not arthritis with secondary osteomyelitis. ### Important Nomenclature Clarification **Poncet's disease** (reactive tuberculous polyarthritis) is a sterile, reactive arthritis occurring in the setting of active TB elsewhere in the body — *M. tuberculosis* is NOT isolated from the joint. This is distinct from tuberculous osteomyelitis, where the organism is directly cultured from the bone/sinus. Option B in this question incorrectly labels TB osteomyelitis as "Poncet's disease," but the underlying diagnosis of tuberculous osteomyelitis is correct. ### Distinguishing Tuberculous Skeletal Disease | Feature | Tuberculous Osteomyelitis | Tuberculous Arthritis with Secondary Osteomyelitis | Pyogenic Osteomyelitis | |---------|--------------------------|-----------------------------------------------------|----------------------| | **Primary site** | Bone metaphysis | Joint (synovium); spreads to bone | Bone metaphysis | | **Onset** | Insidious (weeks–months) | Insidious; joint swelling prominent | Acute (days); fever, toxemia | | **Fever/Systemic signs** | Absent or low-grade | Absent or low-grade | High fever, toxemia | | **Blood culture** | Negative | Negative | Often positive | | **Pus culture organism** | *M. tuberculosis* | *M. tuberculosis* | *S. aureus*, *S. pyogenes* | | **Radiological pattern** | Lytic, 'moth-eaten' or 'caries sicca' | Joint space narrowing + adjacent bone lysis | Periosteal reaction, sequestrum, involucrum | | **Sinus tract** | May occur (chronic) | May occur (chronic) | Common (acute suppurative) | ### Why This Case Is Tuberculous Osteomyelitis 1. **Positive pus culture for *M. tuberculosis*:** Gold standard for diagnosis. The organism was cultured from the sinus tract draining the bone lesion, confirming direct mycobacterial infection of bone. 2. **Primary bone lesion:** The lytic 'moth-eaten' lesion is in the distal femur (medial femoral condyle), with bone marrow edema on MRI — the primary pathology is in the bone, not the joint synovium. 3. **Afebrile, insidious 4-month course:** Skeletal TB is characteristically indolent, without high fever or systemic toxemia — contrasting with acute pyogenic osteomyelitis. 4. **Negative blood culture:** *M. tuberculosis* is not isolated from blood in skeletal TB; this rules out acute pyogenic osteomyelitis where bacteremia is common. 5. **Draining sinus tract:** A hallmark of chronic osteomyelitis, including tuberculous osteomyelitis, where cold abscess formation and sinus tract development are classic. 6. **Elevated but not dramatically raised ESR/CRP:** Consistent with chronic granulomatous infection rather than acute pyogenic sepsis. **Why NOT Tuberculous Arthritis with Secondary Osteomyelitis (Option C):** In tuberculous arthritis, the primary site is the synovium, with joint space narrowing and periarticular osteopenia as early radiological features. Secondary bone involvement occurs later. In this case, the primary lesion is in the bone (distal femur), with no mention of joint space narrowing or synovial involvement — making primary tuberculous osteomyelitis the correct diagnosis. **Why NOT Brucellosis (Option A):** Brucellosis can cause chronic osteomyelitis but is associated with animal exposure (livestock), positive Brucella serology/culture, and is far less common in urban India. The pus culture here grew *M. tuberculosis*, not *Brucella* spp. **Why NOT Pyogenic Osteomyelitis (Option D):** Pyogenic osteomyelitis presents acutely with high fever, toxemia, and often positive blood culture. The 4-month indolent course, afebrile status, and *M. tuberculosis* on culture exclude this diagnosis. **Clinical Pearl:** In India (endemic TB region), any chronic osteomyelitis with a draining sinus, afebrile status, and negative routine cultures must be investigated for *M. tuberculosis*. Pus from sinuses should always be sent for AFB smear, culture, and PCR. (Reference: Maheshwari's Orthopedics; Harrison's Principles of Internal Medicine, 21st ed., Chapter on Skeletal Tuberculosis) **High-Yield:** The combination of positive *M. tuberculosis* culture + lytic 'moth-eaten' bone lesion + draining sinus + afebrile indolent course = **Tuberculous Osteomyelitis**. Do not confuse with Poncet's disease (reactive, sterile arthritis in TB) or tuberculous arthritis (primary synovial disease). **Mnemonic: CRAB** — Chronic, afebrile, Resistant to antibiotics, Blood culture negative = Think TB osteomyelitis. 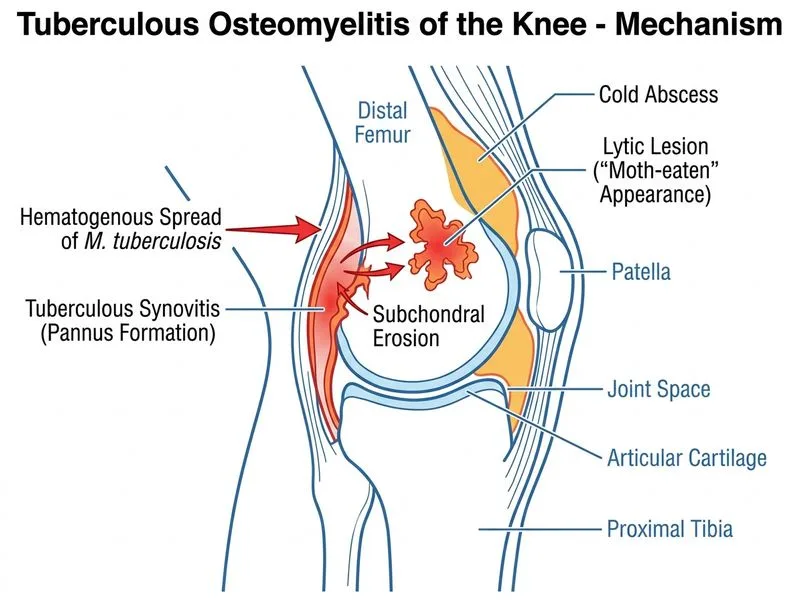
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.