## Pathophysiology of Bone Loss in This Patient This patient has **multifactorial osteoporosis** with two major contributors: chronic glucocorticoid therapy and active rheumatoid arthritis. The dominant mechanism is increased bone resorption, not impaired mineralization. ## Mechanisms of Glucocorticoid-Induced Osteoporosis (GIO) ```mermaid flowchart TD A[Chronic glucocorticoid use]:::outcome A --> B[Direct effects on bone cells]:::action A --> C[Indirect systemic effects]:::action B --> B1[↓ Osteoblast differentiation & function]:::action B --> B2[↑ Osteoblast apoptosis]:::action B --> B3[↑ Osteoclast lifespan]:::action C --> C1[↓ Intestinal calcium absorption]:::action C --> C2[↑ Renal calcium wasting]:::action C --> C3[Secondary hyperparathyroidism]:::action B1 --> D[Net result: ↑ Bone resorption]:::urgent B2 --> D B3 --> D C1 --> D C2 --> D C3 --> D D --> E[Accelerated bone loss & fracture risk]:::urgent ``` **High-Yield:** Glucocorticoid-induced osteoporosis (GIO) causes rapid bone loss, particularly in the first 3–6 months of therapy. Loss of 5–10% of bone mass per year is common with doses ≥7.5 mg prednisolone daily [cite:Harrison 21e Ch 425]. ## Dual Contribution: Glucocorticoids + RA | Factor | Mechanism | Impact | |--------|-----------|--------| | **Prednisolone 7.5 mg daily** | Suppresses osteoblast function; increases osteoclast lifespan; reduces intestinal Ca²⁺ absorption; increases renal Ca²⁺ wasting | Rapid bone loss, especially in first 6 months | | **Active RA (TNF-α, IL-6)** | Inflammatory cytokines directly stimulate osteoclastogenesis via RANKL pathway; promote osteoblast apoptosis | Systemic bone loss + local periarticular erosions | | **Combined effect** | Synergistic increase in bone resorption | T-score −3.2 at lumbar spine (severe osteoporosis) | **Key Point:** While estrogen deficiency (menopause) is the most common cause of postmenopausal osteoporosis, in this patient the dominant mechanism is glucocorticoid-induced and RA-mediated bone resorption, not estrogen deficiency alone. ## Why Vitamin D Deficiency (Option 3) Is NOT the Primary Mechanism **Warning:** Vitamin D insufficiency (22 ng/mL) is **present but secondary**. It contributes to secondary hyperparathyroidism and worsens bone loss, but it does NOT explain the severe osteoporosis (T-score −3.2) in the presence of normal calcium and phosphate. Vitamin D deficiency causes **impaired mineralization** (osteomalacia), not the rapid resorptive bone loss seen here. ## Clinical Pearl **Mnemonic: GLUCOCORTICOID BONE LOSS** — **G**lucose metabolism altered, **L**ow osteoblast function, **U**ncoupling of remodeling, **C**alcium malabsorption, **O**steoclast activation, **C**ytokine effects (in RA), **O**steoblast apoptosis, **R**enal wasting, **T**herapy duration critical, **I**nflammatory disease (RA), **C**ombined with RA cytokines, **O**steoporosis rapid onset, **I**ntestinal absorption ↓, **D**irect bone cell effects. **Key Point:** GIO is characterized by **high bone turnover** (increased resorption >> increased formation), not low turnover. This is why antiresorptive agents (bisphosphonates) are effective. 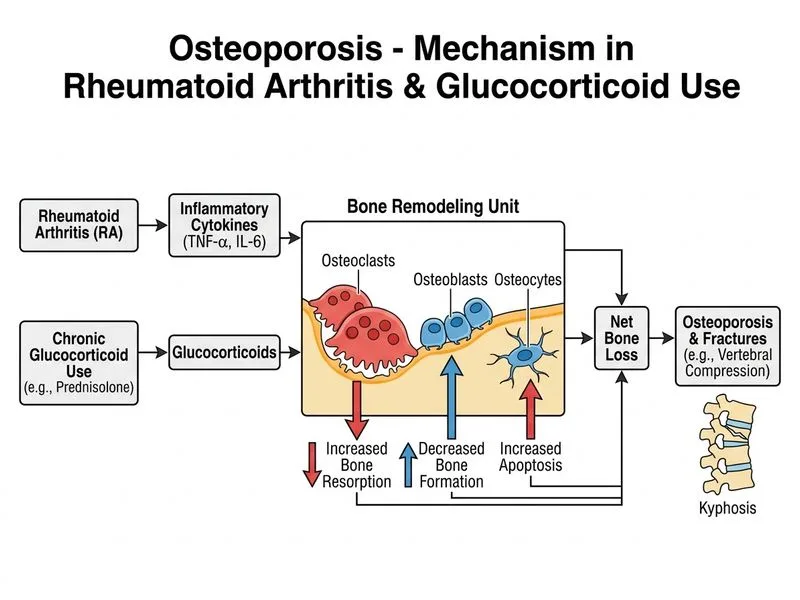
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.