## Clinical Context: CKD and Bone Disease **Key Point:** Chronic kidney disease stage 3b is associated with mineral and bone disorder (MBD). The combination of hypocalcemia, hyperphosphatemia, reduced vitamin D, and a fragility fracture in the setting of CKD points to renal osteodystrophy rather than simple osteoporosis. ## Differential Diagnosis of CKD-MBD ```mermaid flowchart TD A[CKD Stage 3b]:::outcome --> B[Phosphate retention]:::outcome B --> C[Secondary hyperparathyroidism]:::outcome C --> D{Bone turnover?}:::decision D -->|High| E[High-turnover bone disease]:::action D -->|Low| F[Adynamic bone disease]:::action D -->|Mixed| G[Mixed uremic bone disease]:::action A --> H[Vitamin D deficiency]:::outcome H --> I[↓ Calcium absorption]:::outcome I --> C ``` ## Why This Is Renal Osteodystrophy, Not Simple Osteoporosis | Feature | This Patient | Simple Osteoporosis | Renal Osteodystrophy | |---------|--------------|--------------------|-----------------------| | **eGFR** | 35 (CKD 3b) | Normal (>60) | <60 (CKD 3–5) | | **Phosphate** | 4.8 (HIGH) | Normal (2.5–4.5) | Elevated (↑ retention) | | **Calcium** | 8.2 (LOW) | Normal or low-normal | Low (↓ activation of vitamin D) | | **Vitamin D** | 18 (DEFICIENT) | May be low | Often deficient | | **PTH** | Expected ↑↑ | Normal or low | Markedly elevated | | **Pathology** | Loss of bone mass | Loss of bone mass | Altered bone turnover + mass loss | **High-Yield:** Renal osteodystrophy encompasses a spectrum of bone abnormalities in CKD, including: - **High-turnover disease** (secondary hyperparathyroidism with increased bone remodeling) - **Low-turnover disease** (adynamic bone disease, osteomalacia) - **Mixed uremic bone disease** (combination of high-turnover and low-turnover features) This patient has evidence of secondary hyperparathyroidism (hypocalcemia, hyperphosphatemia, vitamin D deficiency) with mixed features — hence "mixed uremic bone disease." ## Clinical Pearl **Warning:** Do NOT diagnose simple osteoporosis in a patient with CKD without first evaluating mineral metabolism. The T-score alone is misleading in CKD; bone quality and turnover are abnormal even if bone density appears only mildly reduced. Treating CKD-MBD requires phosphate binders, vitamin D analogues, and PTH suppression — not just calcium and bisphosphonates. ## Why Each Distractor Is Wrong | Option | Reason | |--------|--------| | **Osteoporosis with secondary hyperparathyroidism** | While secondary hyperparathyroidism is present, the underlying pathology is not simple osteoporosis. Renal osteodystrophy is the correct term for bone disease in CKD; it encompasses altered turnover, mineralization defects, and abnormal remodeling — not just mass loss. | | **Osteomalacia due to vitamin D deficiency** | Although vitamin D deficiency is present (25-OH-D = 18 ng/mL), osteomalacia alone does not explain the hyperphosphatemia and hypocalcemia in the context of CKD 3b. Osteomalacia is a mineralization defect; renal osteodystrophy is the broader diagnosis that includes vitamin D deficiency as one component. | | **Adynamic bone disease** | Adynamic bone disease is a low-turnover variant of renal osteodystrophy, characterized by suppressed PTH and reduced bone remodeling. This patient has evidence of secondary hyperparathyroidism (hypocalcemia, hyperphosphatemia), indicating high-turnover disease or mixed disease, not purely adynamic bone disease. | ## Management Implications **Mnemonic: PHOS-CAL-VIT** — **P**hosphate binders (calcium acetate, sevelamer), **H**yperparathyroidism management (vitamin D analogues, calcimimetics), **O**ptimize **S**erum calcium, **C**ontrol **A**lkaline phosphatase, **L**imit **V**itamin D supplementation (risk of hypercalcemia), **I**ncrease **T**arget PTH (8–72 pg/mL in CKD 3b). **Clinical Pearl:** Bisphosphonates are generally avoided in CKD 3b–4 due to risk of adynamic bone disease and impaired renal clearance. First-line therapy is phosphate restriction, phosphate binders, vitamin D analogues (calcitriol, paricalcitol), and calcimimetics (cinacalcet) if PTH is markedly elevated. 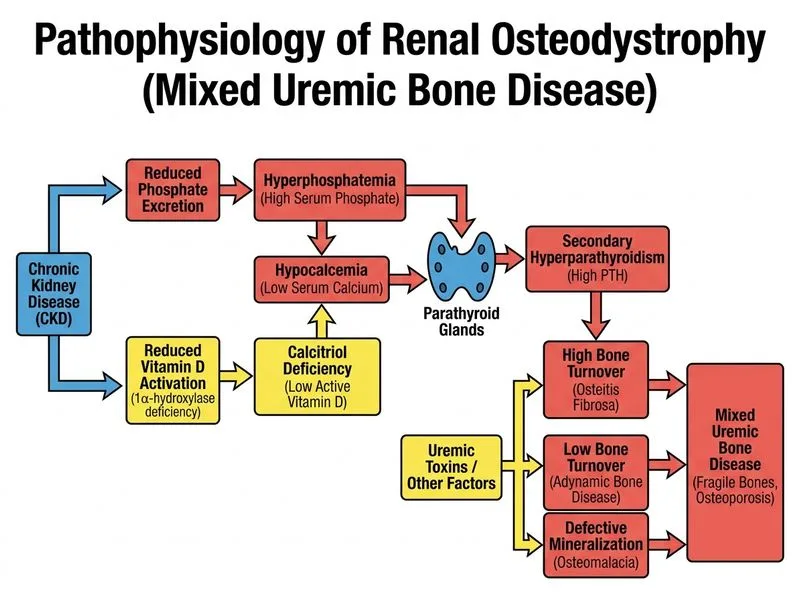
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.