## Clinical Context: Renal Osteodystrophy This patient has **chronic kidney disease–mineral bone disorder (CKD-MBD)**, a complex syndrome encompassing secondary hyperparathyroidism, abnormal mineral metabolism, and bone disease. ### Diagnostic Clues **Key Point:** The 'rugger jersey spine' (alternating bands of sclerosis and lucency on X-ray) is pathognomonic for secondary hyperparathyroidism in CKD, NOT primary osteoporosis. **High-Yield:** The constellation of: - CKD stage 3b (eGFR 32) - **Elevated PTH** (185 pg/mL, >2.8× upper normal) - **Hypocalcemia** (7.8 mg/dL, <8.5) - **Hyperphosphatemia** (4.8 mg/dL, >3.5) - **Vitamin D insufficiency** (22 ng/mL) - **Rugger jersey spine** ...all point to **secondary hyperparathyroidism**, NOT primary osteoporosis or osteomalacia alone. ## Pathophysiology: The Cascade ```mermaid flowchart TD A[CKD stage 3b: eGFR 32]:::outcome A --> B[Reduced nephron mass]:::outcome B --> C[↓ Phosphate excretion]:::outcome C --> D[Hyperphosphatemia]:::outcome D --> E[↓ 1,25-dihydroxyvitamin D production]:::outcome E --> F[Hypocalcemia]:::outcome F --> G[Parathyroid gland stimulation]:::action G --> H[↑ PTH secretion]:::action H --> I[Secondary hyperparathyroidism]:::outcome I --> J[Increased bone turnover]:::action J --> K[Osteitis fibrosa cystica + rugger jersey spine]:::outcome E --> L[Concurrent osteomalacia]:::outcome L --> K ``` ### Mechanism in Detail | Step | Mechanism | Lab Finding | |------|-----------|-------------| | 1. Phosphate retention | ↓ GFR → ↓ renal phosphate excretion | PO₄ 4.8 (↑) | | 2. FGF23 surge | Phosphate-sensing → ↑ FGF23 (suppresses 1α-hydroxylase) | PTH 185 (↑) | | 3. Calcitriol deficiency | ↓ 1α-hydroxylase activity → ↓ 1,25(OH)₂D₃ | Ca 7.8 (↓) | | 4. Hypocalcemia | ↓ Intestinal calcium absorption | PTH ↑ further | | 5. PTH resistance | Uremic toxins + hyperphosphatemia impair PTH signaling | Parathyroid hyperplasia | | 6. Bone disease | ↑ Osteoblast & osteoclast activity; fibrosis | Rugger jersey | **Clinical Pearl:** In CKD, bone disease is **mixed**: secondary hyperparathyroidism (high-turnover) + osteomalacia (low 1,25(OH)₂D₃) + adynamic bone disease (if PTH is suppressed too aggressively). This patient has predominantly high-turnover disease (elevated PTH, elevated ALP, rugger jersey). **Mnemonic — CKD-MBD triad:** **PHO** = **P**hosphate retention, **H**yperparathyroidism, **O**steodystrophy [cite:Harrison 21e Ch 279]. ## Why NOT the Other Options? ### Option 1: Primary Hyperparathyroidism **Distinguishing features:** - Primary: PTH ↑ with **hypercalcemia** (usually >10.5 mg/dL) - Secondary (this patient): PTH ↑ with **hypocalcemia** (7.8 mg/dL) - Primary: Normal/low phosphate; Secondary: **Hyperphosphatemia** (4.8 mg/dL) - Primary: No rugger jersey spine; Secondary: **Rugger jersey is hallmark** **Warning:** Do NOT confuse secondary hyperparathyroidism with primary hyperparathyroidism — the calcium direction is opposite. ### Option 3: Osteomalacia from Vitamin D Deficiency Alone - Vitamin D insufficiency (22 ng/mL) is *present* but is a **cofactor**, not the primary driver - Pure osteomalacia shows **normal or low PTH**, not elevated PTH - This patient's elevated PTH and rugger jersey indicate **secondary hyperparathyroidism superimposed on osteomalacia** - Treating vitamin D alone without addressing phosphate retention and PTH will not resolve the bone disease ### Option 4: Estrogen Deficiency - This is a **72-year-old man** — estrogen deficiency is not relevant - Even in women, estrogen deficiency causes postmenopausal osteoporosis, NOT secondary hyperparathyroidism or rugger jersey spine - CKD-MBD is mineral-driven, not sex-hormone-driven ## Management Implications **Key Point:** Treatment must address the entire cascade: 1. **Phosphate binders** (calcium carbonate, sevelamer, lanthanum) → ↓ serum phosphate 2. **Vitamin D analogs** (calcitriol, paricalcitol) → ↑ serum calcium, suppress PTH 3. **Calcimimetics** (cinacalcet) → ↓ PTH if resistant to above 4. **Dietary phosphate restriction** → reduce dietary load 5. **Monitor PTH target** (CKD stage 3: PTH 35–70 pg/mL per KDIGO) **Clinical Pearl:** Simply giving calcium and vitamin D supplements without phosphate binders will worsen hyperphosphatemia and perpetuate secondary hyperparathyroidism. 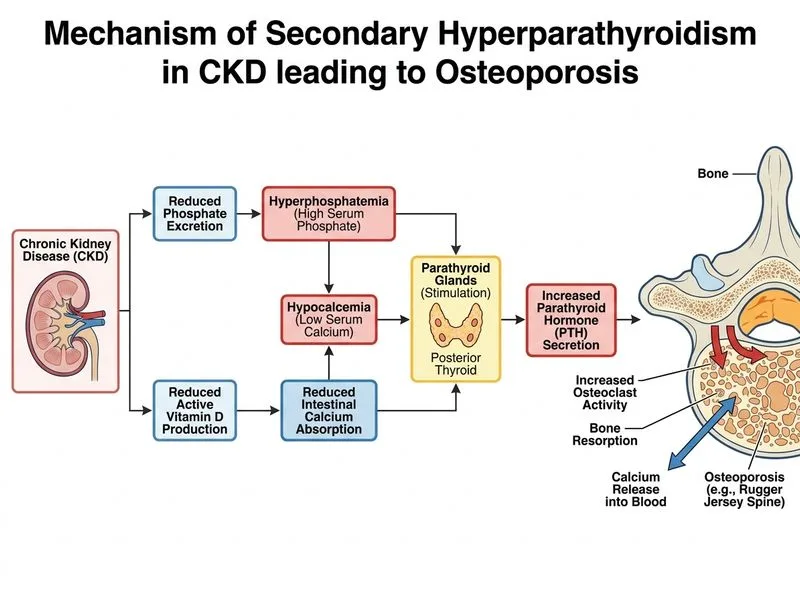
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.