## Management of Osteosarcoma: Neoadjuvant Chemotherapy First ### Current Standard of Care **Key Point:** The modern management paradigm for osteosarcoma is **biopsy confirmation followed by neoadjuvant chemotherapy and then wide surgical resection**. In clinical practice, biopsy is performed as part of the staging workup, and once histological diagnosis is confirmed, neoadjuvant chemotherapy is initiated promptly. This multimodal approach has improved 5-year survival from ~20% (surgery alone) to ~70%. ### Why Neoadjuvant Chemotherapy? | Rationale | Benefit | |-----------|----------| | **Systemic disease control** | Targets micrometastases (present in ~80% at diagnosis) | | **Tumor downsizing** | Reduces soft tissue extension; aids surgical planning | | **Chemosensitivity assessment** | Guides adjuvant therapy; good responders have better prognosis | | **Limb salvage facilitation** | Allows wider margins without amputation | | **Proven survival benefit** | Level 1 evidence from multiple RCTs | ### Treatment Algorithm The standard sequence in localized osteosarcoma: 1. **Staging workup** — MRI of primary, CT chest, bone scan 2. **Biopsy** — core needle or open biopsy for histological confirmation (performed at the treating center to avoid tract contamination) 3. **Neoadjuvant chemotherapy** — 8–12 weeks (MAP protocol) 4. **Wide surgical resection** — limb-salvage preferred 5. **Adjuvant chemotherapy** — to complete ~6 months total ### Why Option B (Neoadjuvant Chemo → Surgery) Is Correct in This Context This question asks for the **most appropriate next step** in a patient whose clinical and radiological picture is **classic for osteosarcoma** (adolescent, proximal tibial metaphysis, sunburst periosteal reaction, mixed lytic-sclerotic lesion, elevated ALP and LDH, no metastases on CT chest). In the NEET PG / INI-CET framework, the tested standard-of-care answer for localized osteosarcoma is **neoadjuvant chemotherapy followed by wide resection** — reflecting the landmark COSS and INT-0133 trial protocols. Biopsy is understood to be part of the staging workup that precedes chemotherapy initiation, not a separate "next step" that delays treatment. ### Neoadjuvant Chemotherapy Regimen **High-Yield:** The standard regimen is **MAP** (Methotrexate, doxorubicin [Adriamycin], cisplatin): 1. **Cisplatin** 120 mg/m² IV 2. **Doxorubicin** 75 mg/m² IV 3. **High-dose Methotrexate** 12 g/m² IV (with leucovorin rescue) **Duration:** 8–12 weeks (typically 2–3 cycles before surgery) ### Chemosensitivity & Prognosis **Clinical Pearl:** Tumor necrosis >90% after neoadjuvant therapy indicates good chemosensitivity and is the **strongest prognostic factor** for disease-free survival (Huvos grading system). - **Good responders** (>90% necrosis): 5-year DFS ~80–85% - **Poor responders** (<90% necrosis): 5-year DFS ~50–60% ### Surgical Resection **Key Point:** Surgery is performed **after** neoadjuvant chemotherapy (typically 3–4 weeks post-final cycle): - **Wide excision** with 2–3 cm margins - **Limb-salvage surgery** preferred over amputation when feasible - **Reconstruction** with prosthesis, allograft, or autograft - **Intraoperative frozen section** to confirm negative margins ### Why Not the Other Options? **Option A — Palliative radiation therapy:** - Osteosarcoma is relatively radioresistant; radiation is **not** first-line - Palliative intent applies to **unresectable or metastatic disease** — this patient has localized disease with no CT chest metastases, so curative intent is appropriate - Radiation may be used for pain control or in unresectable pelvic/axial tumors **Option C — Surgery alone (wide resection without chemotherapy):** - Historical approach (pre-1970s); now **obsolete** - Leaves micrometastases untreated → high recurrence rate - 5-year survival <20% without chemotherapy (Jaffe et al., 1974) **Option D — Needle biopsy before any treatment:** - Biopsy is indeed essential and is performed as part of the staging workup **before** chemotherapy begins; however, in the context of this question, Option D implies biopsy as the *only* next step, delaying the definitive treatment plan - The question stem already provides a highly characteristic clinical-radiological diagnosis; the tested answer reflects the **overall management strategy** (neoadjuvant chemo → surgery), not a single isolated procedural step - In real practice, biopsy and chemotherapy planning occur in close sequence at the treating center **Mnemonic — NACS:** **N**eoadjuvant chemo → **A**ssess response → **C**ut (surgery) → **S**urveillance. The modern osteosarcoma paradigm: start chemo early, assess response, then resect, then finish chemo. [cite: Robbins & Cotran Pathologic Basis of Disease, 10e, Ch 26; Harrison's Principles of Internal Medicine, 21e; Maheshwari & Mhaskar — Essentials of Orthopedics] 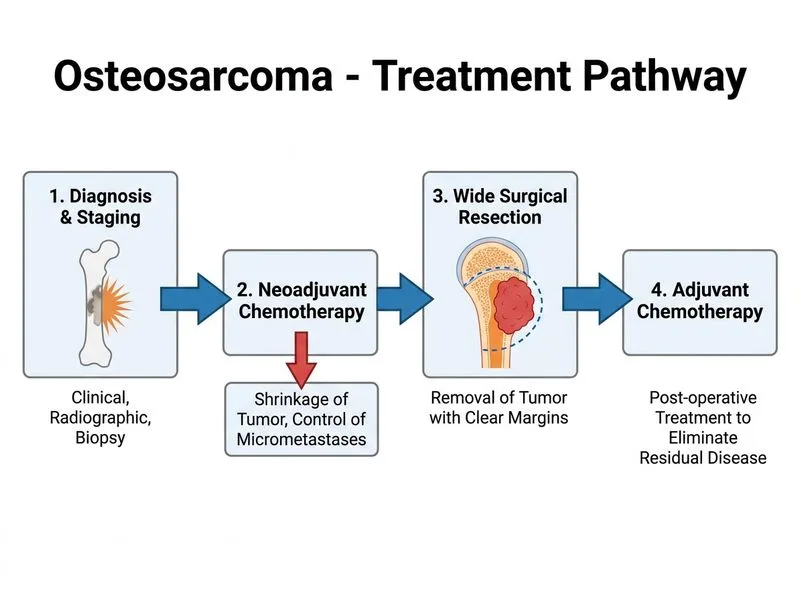
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.