## Prognostic Factors in Advanced Ovarian Cancer **Key Point:** Among all prognostic factors in ovarian cancer, **extent of cytoreduction** (residual tumor burden) is the single most important modifiable factor that directly impacts overall survival, independent of stage or histology. ### Hierarchy of Prognostic Factors | Prognostic Factor | Impact on OS | Modifiable? | |-------------------|--------------|-------------| | **Residual disease burden** | Strongest predictor | **Yes** — surgical skill | | **FIGO stage** | Strong predictor | No — extent at diagnosis | | **Platinum sensitivity** | Strong predictor | No — tumor biology | | **CA-125 nadir** | Moderate predictor | Partially — chemotherapy response | | **Histological grade** | Moderate predictor | No — tumor biology | | **Age** | Weak predictor | No — patient factor | | **Histological subtype** | Weak predictor | No — tumor biology | **High-Yield:** Optimal cytoreduction (residual disease <1 cm) is associated with a **median OS of 40–50 months**, while suboptimal cytoreduction (>1 cm) results in median OS of 20–30 months in Stage III disease. This is the **most modifiable** and **most impactful** prognostic factor. ### Why Cytoreduction Matters 1. **Reduces tumor burden** — fewer cancer cells for chemotherapy to target 2. **Improves chemotherapy penetration** — smaller residual masses have better drug delivery 3. **Removes chemotherapy-resistant foci** — bulky disease harbors resistant clones 4. **Predictive of platinum sensitivity** — patients achieving optimal debulking often have platinum-sensitive tumors **Clinical Pearl:** The **"no residual disease" (R0)** resection is increasingly recognized as the gold standard. Recent data (DESKTOP III, LION trial) show that aggressive cytoreduction to R0 improves recurrence-free survival and overall survival compared to <1 cm residual disease. ### Why Other Options Are Weaker Prognostic Factors **Histological subtype (serous vs. mucinous):** - Serous tumors are more common and have intermediate prognosis - Mucinous tumors are rare and often present at earlier stages - However, **grade** (G1, G2, G3) is more prognostically relevant than subtype - Subtype alone does NOT override the impact of cytoreduction **Age at diagnosis:** - Age is a **weak** prognostic factor - Younger patients (age <50) have slightly better outcomes, but the difference is modest (5–10% in 5-year OS) - Performance status and comorbidities matter more than chronological age - Cytoreduction benefit is independent of age **Number of chemotherapy cycles:** - Standard is 6 cycles of platinum-paclitaxel - Extending beyond 6 cycles does NOT improve OS (ICON3, GOG-114 trials) - The **response to chemotherapy** (CA-125 nadir, imaging response) is more prognostically relevant than cycle count - Completion of 6 cycles is standard; additional cycles add toxicity without benefit ### Treatment Outcome in This Patient - **Optimal cytoreduction achieved** ✓ (best prognostic indicator) - **Complete clinical response** ✓ (good sign) - **Normal CA-125 nadir** ✓ (favorable response) - **Serous histology** (intermediate prognosis, but not the strongest factor) - **Expected 5-year OS:** ~40–50% for Stage IIIC with optimal debulking and platinum sensitivity **Mnemonic:** **CROPS** — Cytoreduction, Response to chemotherapy, Platinum sensitivity, Stage, Grade (in order of prognostic strength for advanced ovarian cancer). 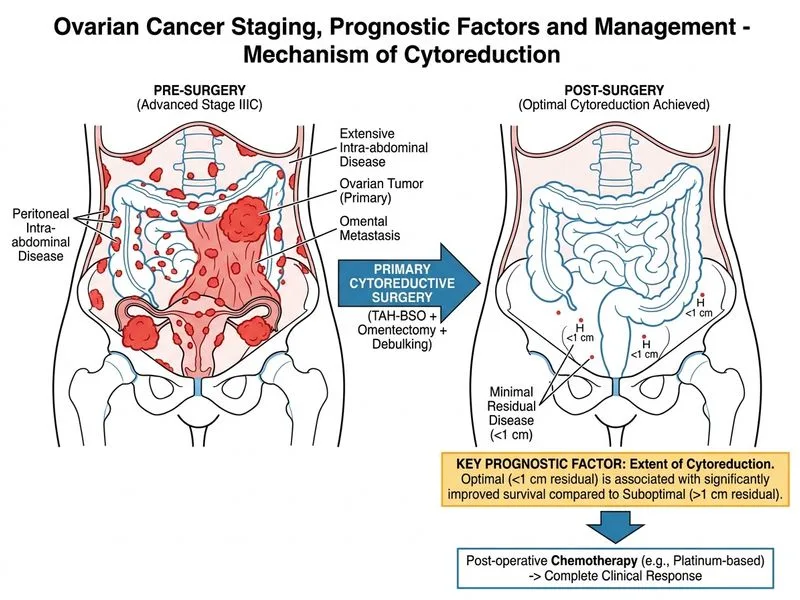
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.