## Clinical Diagnosis: Mucinous Cystadenoma **Key Point:** The defining feature that separates **mucinous cystadenoma** (benign) from **mucinous cystadenocarcinoma** (malignant) is the presence or absence of **true stromal invasion**. Mucin extravasation into the stroma alone — without frank stromal invasion or capsular breach — does NOT constitute malignancy. This case explicitly states **no invasion of the ovarian capsule**, making mucinous cystadenoma the correct diagnosis. ### Diagnostic Criteria: Mucinous Cystadenoma vs. Cystadenocarcinoma | Feature | Mucinous Cystadenoma | Mucinous Cystadenocarcinoma | | --- | --- | --- | | **Stromal invasion** | Absent | Present (frank infiltrative or expansile invasion) | | **Capsule** | Intact | Breached or ruptured | | **Epithelial atypia** | Minimal or absent | Moderate to severe | | **Size** | Often large (10–30 cm) | Often large; size alone ≠ malignancy | | **CA-125** | Normal or mildly elevated | Mildly to moderately elevated | | **Ascites** | Absent | May be present | | **Prognosis** | Excellent (>95% 5-yr survival) | ~50–60% 5-yr survival | **High-Yield (Robbins Pathology):** Mucinous cystadenomas are the **most common benign ovarian epithelial tumors** and can grow to enormous sizes (10–30 cm). They are lined by tall columnar mucinous epithelium resembling endocervical or intestinal epithelium. Mucin extravasation into the stroma can occur as a secondary phenomenon (e.g., cyst rupture) and does **not** by itself indicate malignancy. True carcinoma requires **demonstrable stromal invasion** (irregular glands infiltrating stroma with desmoplastic reaction) or **capsular breach**. ### Pathologic Interpretation of This Case 1. **Tall columnar mucinous epithelium** — hallmark of mucinous differentiation ✓ 2. **Mucin extravasation into stroma** — a secondary finding, NOT equivalent to stromal invasion ✓ 3. **No invasion of the ovarian capsule** — explicitly stated; this rules out carcinoma ✓ 4. **Predominantly cystic, minimal solid component** — favors benign/borderline ✓ 5. **Only mildly elevated CA-125 (45 U/mL)** — consistent with benign mucinous tumor ✓ 6. **No ascites** — further supports benign process ✓ This combination = **Mucinous cystadenoma**, not cystadenocarcinoma. ### Why the Other Options Are Incorrect - **A) Clear cell carcinoma:** Characterized by hobnail cells, clear cytoplasm, and solid/papillary architecture — not mucinous epithelium. - **B) Serous cystadenocarcinoma:** Shows psammoma bodies, papillary architecture, and serous (not mucinous) epithelium; typically associated with markedly elevated CA-125. - **C) Mucinous cystadenocarcinoma:** Requires frank stromal invasion or capsular breach — neither is present in this case. Mucin extravasation alone is insufficient for this diagnosis. **Clinical Pearl:** A **mucinous borderline tumor (atypical proliferative mucinous tumor)** would be considered if there is epithelial stratification and mild atypia without stromal invasion — but the stem describes no atypia and no invasion, making straightforward cystadenoma the best fit. Per Robbins (10th ed.), the diagnosis of carcinoma requires unequivocal stromal invasion. **Mnemonic — Mucinous Cystadenoma:** **No Invasion = No Carcinoma**. Large size + mucinous epithelium + intact capsule + no stromal invasion = Benign cystadenoma. 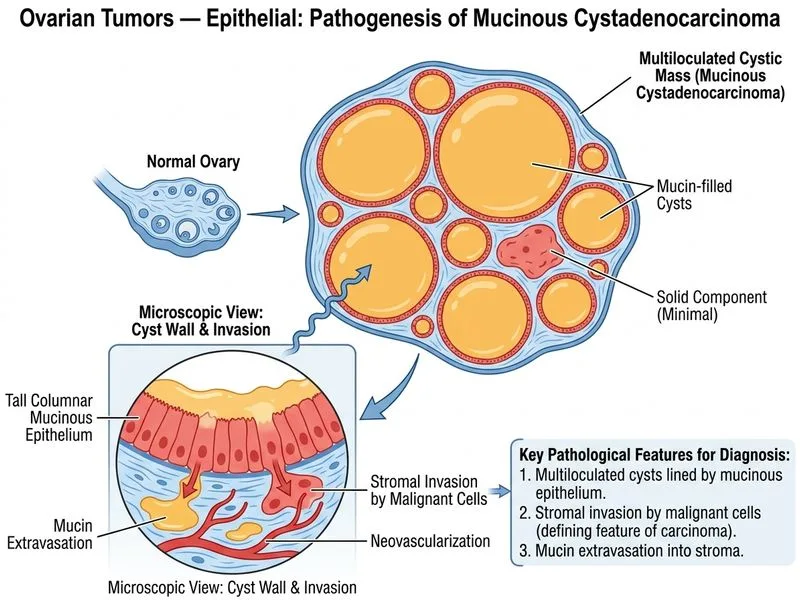
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.