## Clinical Presentation and Diagnosis **Key Point:** Markedly elevated β-hCG (>100,000 mIU/mL) in a young woman with an ovarian mass indicates a trophoblastic component. Mixed germ cell tumours with choriocarcinoma component are more common than pure choriocarcinoma in the ovary. ### Why Mixed Germ Cell Tumour with Choriocarcinoma Component? The clinical and biochemical profile indicates a germ cell tumour with trophoblastic differentiation: 1. **Markedly elevated β-hCG**: 185,000 mIU/mL is characteristic of choriocarcinoma or mixed germ cell tumour with trophoblastic component 2. **Normal AFP**: Rules out yolk sac tumour and mixed tumours with significant yolk sac component 3. **Age and presentation**: Young woman with acute presentation (pain, vaginal bleeding, haemorrhage) 4. **Imaging**: Large mass with internal haemorrhage reflects the aggressive, highly vascular nature of trophoblastic tissue 5. **Pure choriocarcinoma rarity**: Primary pure ovarian choriocarcinoma is extremely rare (<1% of ovarian germ cell tumours); mixed germ cell tumours with choriocarcinoma component are more common **High-Yield:** Mixed germ cell tumours are the **most common malignant ovarian germ cell tumour overall** (accounting for ~40% of malignant germ cell tumours). They may contain yolk sac, choriocarcinoma, dysgerminoma, and teratoma elements. The clinical and biochemical picture is dominated by the most hormonally active component. ### β-hCG-Secreting Germ Cell Tumours: Differential | Tumour Type | β-hCG Level | AFP | Clinical Features | Frequency | |---|---|---|---|---| | Pure choriocarcinoma (ovarian) | Very high (>100,000) | Normal | Rare, acute presentation, haemorrhage | <1% of germ cell tumours | | Mixed germ cell (with choriocarcinoma) | High (often >50,000) | Variable (↑ if yolk sac present) | More common; may have yolk sac component | ~40% of malignant germ cell tumours | | Dysgerminoma with trophoblastic differentiation | Mild to moderate ↑ | Normal | Rare; usually pure dysgerminoma is non-secreting | <5% | | Immature teratoma with trophoblastic element | Mild to moderate ↑ | May be ↑ | Depends on grade and other elements | <10% | **Clinical Pearl:** The combination of **very high β-hCG + normal AFP + young age + acute presentation with haemorrhage** is the hallmark of a choriocarcinoma-containing germ cell tumour. Mixed germ cell tumours are more common than pure choriocarcinoma in the ovary. ### Pathological Basis Mixed germ cell tumours arise from a totipotent germ cell and may differentiate along multiple lineages: - **Yolk sac component** → AFP production - **Trophoblastic component (syncytiotrophoblast)** → β-hCG production - **Dysgerminoma component** → usually non-secreting - **Teratoma component** → variable The **predominant choriocarcinoma component** in this case explains the markedly elevated β-hCG and normal AFP. ### Management and Prognosis - **Surgery**: Unilateral salpingo-oophorectomy (fertility-sparing when possible) - **Chemotherapy**: BEP regimen (bleomycin, etoposide, cisplatin) for advanced or high-risk disease - **Prognostic factors**: β-hCG level, AFP level, stage, and histological composition - **Prognosis**: Good to excellent with modern chemotherapy, even for advanced stages (5-year survival >80% for non-metastatic disease) **Mnemonic:** **MIXED GCT + HIGH β-hCG = CHORIOCARCINOMA COMPONENT** - M: Multiple tissue types - I: Intermediate prognosis (better than pure choriocarcinoma) - X: eXtreme β-hCG elevation - E: Excellent response to BEP - D: Differentiation along trophoblastic lineage [cite:Robbins 10e Ch 22] 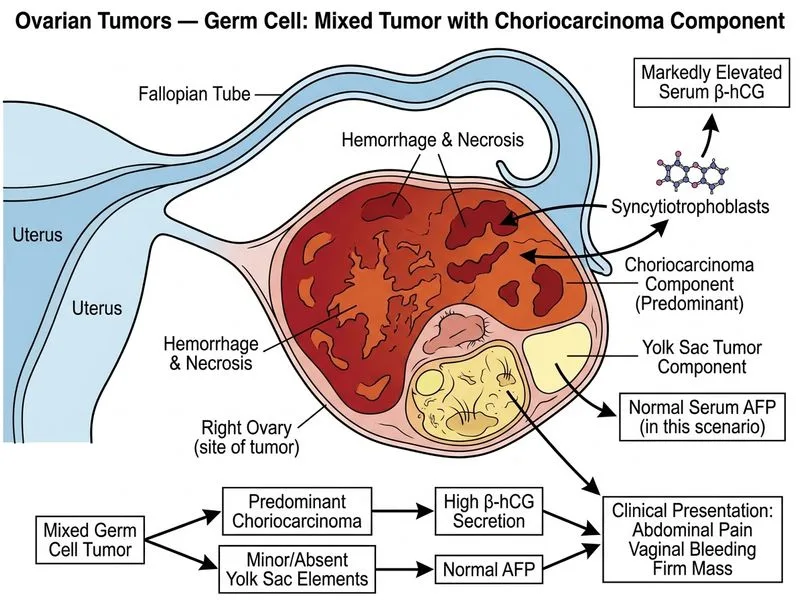
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.