## Distinguishing Mature Cystic Teratoma (MCT) from Dysgerminoma ### Key Histological Difference **Key Point:** The defining feature of mature cystic teratoma (dermoid cyst) is the presence of **somatic differentiation** — organized tissues from all three germ layers (hair follicles, sebaceous glands, bone, cartilage, epithelium). Dysgerminoma, by contrast, is composed entirely of primitive germ cells with no somatic differentiation. ### Comparative Table | Feature | Mature Cystic Teratoma (MCT) | Dysgerminoma | | --- | --- | --- | | **Tissue composition** | Organized somatic tissues (hair, bone, cartilage, epithelium) | Primitive germ cells only | | **Germ layers present** | All three (endo-, meso-, ectoderm) | All three (but undifferentiated) | | **Age of presentation** | Reproductive years (20s–40s) | Adolescents and young women (10s–20s) | | **Malignancy** | Benign (95%); rarely malignant transformation | Malignant | | **Tumor markers** | Usually normal; rarely elevated AFP/hCG | Elevated hCG; normal AFP | | **Appearance** | Cystic with hair, teeth, sebum visible | Solid, tan-white, homogeneous | | **Prognosis** | Excellent (benign course) | Good with chemotherapy (90% 5-yr survival) | ### Clinical Pearl **Clinical Pearl:** Mature cystic teratomas are the most common ovarian germ cell tumor (accounting for ~20% of all ovarian tumors). They are almost always benign and discovered incidentally in reproductive-age women. The presence of **organized, differentiated somatic structures** (especially hair and teeth) is pathognomonic and the single best discriminator from dysgerminoma. ### High-Yield Distinction **High-Yield:** Dysgerminoma = **primitive undifferentiated germ cells** (like seminoma of testis). Mature cystic teratoma = **differentiated somatic tissues** (like dermoid cyst). This is the cardinal distinction. [cite:Robbins 10e Ch 22] 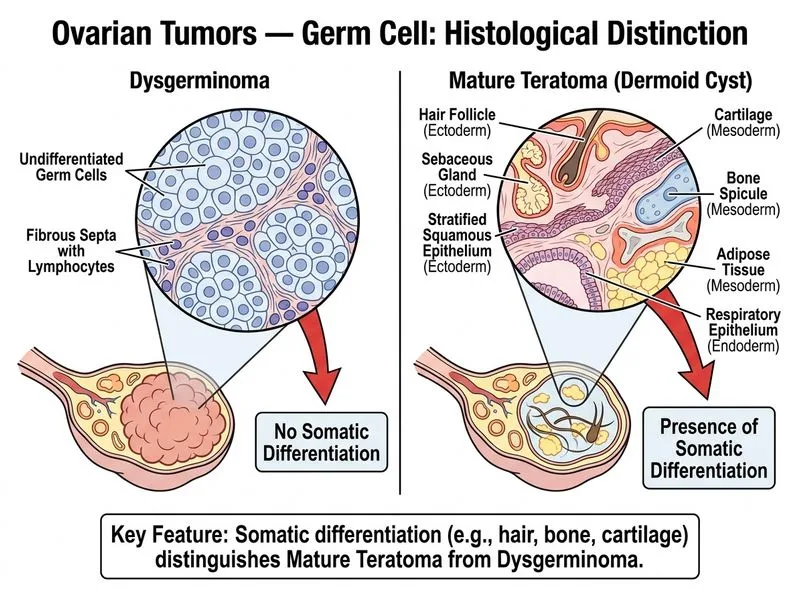
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.