## First-Line Management of Diabetic Peripheral Neuropathic Pain **Key Point:** Both gabapentinoids (gabapentin, pregabalin) AND tricyclic antidepressants (amitriptyline, nortriptyline) are guideline-recommended **first-line** agents for diabetic peripheral neuropathic pain. In this specific clinical context — a patient with **no depression, no anxiety, and no contraindications to either class** — gabapentin is preferred over amitriptyline due to its superior tolerability profile and absence of anticholinergic/cardiac risks. **High-Yield:** For neuropathic pain in diabetes, the evidence-based hierarchy per AAN, EFNS, and NeuPSIG guidelines is: 1. **Gabapentinoids** (gabapentin, pregabalin) — first-line 2. **TCAs** (amitriptyline, nortriptyline) — first-line alternative (especially if concurrent depression/anxiety) 3. **SNRIs** (duloxetine, venlafaxine) — first-line alternative 4. **Opioids** (tramadol, morphine) — reserved for refractory pain after above agents fail **Mnemonic: GAPSO** — **G**abapentin, **A**mitriptyline, **P**regabalin, **S**NRI, **O**pioids (in order of preference for neuropathic pain in most clinical contexts). --- ### Why Gabapentin 300 mg TID Is Correct (Option A) **Mechanism:** Gabapentin binds to the α₂δ subunit of voltage-gated calcium channels in dorsal horn neurons, reducing calcium influx and decreasing release of excitatory neurotransmitters (glutamate, substance P), thereby dampening central sensitization underlying neuropathic pain. **Advantages in This Patient:** - Strong RCT evidence for diabetic peripheral neuropathy (NNT ~4–5) - Renally excreted unchanged; safe with normal eGFR (85 mL/min/1.73 m²) - No hepatic metabolism; minimal drug interactions - No anticholinergic effects, no cardiac conduction risk - Once-daily titration possible; well-tolerated in middle-aged patients - Onset of meaningful analgesia within 1–2 weeks **Dosing:** Start 300 mg once daily or TID, increase by 300 mg every 3–7 days as tolerated; target 1800 mg/day in three divided doses (can go up to 3600 mg/day if needed and tolerated). --- ### Why Amitriptyline Is Also First-Line But Less Preferred Here (Option B) Amitriptyline is a legitimate first-line agent for neuropathic pain (NNT ~3–4) and is **not wrong in general**. However, in this 48-year-old woman **without depression or anxiety**, the TCA's additional pharmacological burden (anticholinergic effects: dry mouth, urinary retention, constipation; orthostatic hypotension; QTc prolongation risk; sedation) makes gabapentin the safer and more appropriate initial choice. TCAs are particularly favored when neuropathic pain co-exists with depression, insomnia, or anxiety — none of which are present here. Per Harrison's Principles of Internal Medicine (21e, Ch. 297), gabapentinoids are preferred when TCAs carry unacceptable risk or when psychiatric comorbidity is absent. **Clinical Pearl:** The distinction between gabapentin and amitriptyline as first-line is **context-dependent**: both are guideline-endorsed, but patient-specific factors (comorbidities, tolerability, age, cardiac history) guide the choice. In exam questions, the absence of depression/anxiety and the presence of a middle-aged patient without cardiac history tips the balance toward gabapentin. --- ### Why Opioids Are Incorrect (Options C & D) **Morphine (Option C):** Strong opioids are **not first-line** for neuropathic pain per WHO, AAN, and NeuPSIG guidelines. They are reserved for refractory cases after gabapentinoids, TCAs, and SNRIs have been optimized. Risks include tolerance, physical dependence, opioid-induced hyperalgesia, and endocrine dysfunction with chronic use. **Tramadol (Option D):** Tramadol has dual action (weak μ-opioid agonism + monoamine reuptake inhibition) and has some evidence in neuropathic pain, but it is classified as a **second- or third-line** agent. It carries opioid-related risks and serotonin syndrome potential. It is not appropriate as initial monotherapy when first-line agents have not been tried. [cite: Harrison 21e Ch. 297; KD Tripathi Essentials of Medical Pharmacology 8e Ch. 32; NeuPSIG Guidelines 2015 (Finnerup et al., Lancet Neurology)] 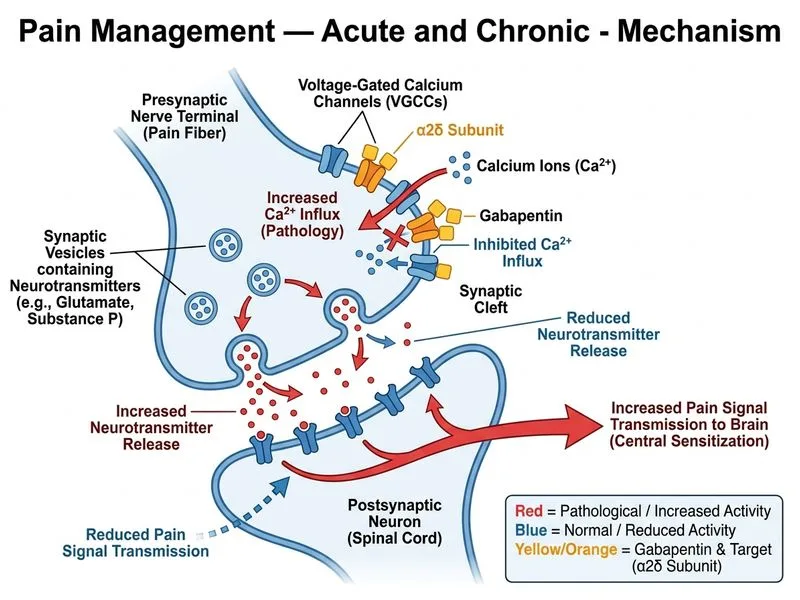
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.