## Neuropathic Pain Management in Diabetic Polyneuropathy **Key Point:** Pregabalin and gabapentin are first-line agents for neuropathic pain, including diabetic peripheral neuropathy (DPN), with strong evidence from randomized controlled trials. ### Mechanism of Action Pregabalin is a gabapentinoid that binds to the α~2~δ subunit of voltage-gated calcium channels, reducing neurotransmitter release and neuropathic pain transmission. ### Evidence Base for DPN - FDA-approved specifically for diabetic peripheral neuropathy - NNT (Number Needed to Treat) ≈ 4–5 for 50% pain reduction - Effective for both positive symptoms (burning, pain) and sleep disturbance - Well-tolerated with predictable pharmacokinetics ### Dosing in DPN | Parameter | Details | | --- | --- | | Starting dose | 75 mg once daily or 50 mg thrice daily | | Target dose | 300 mg/day in divided doses | | Maximum dose | 600 mg/day | | Renal adjustment | Required (CrCl <60 mL/min) | **Clinical Pearl:** Pregabalin also improves sleep quality in neuropathic pain patients, addressing both pain and the patient's sleep disturbance. **High-Yield:** First-line agents for neuropathic pain are gabapentinoids (pregabalin, gabapentin) and SNRIs (duloxetine). NSAIDs and opioids are not first-line for neuropathic pain. ### Why Pregabalin Over Alternatives 1. **Gabapentin** — equally effective but pregabalin has more predictable kinetics 2. **Duloxetine** — also first-line; choice depends on comorbidities (this patient has no contraindications to either) 3. **Tramadol** — second-line; reserved for inadequate response to gabapentinoids 4. **Morphine** — third-line; opioids are not first-line for neuropathic pain due to tolerance and abuse risk 5. **NSAIDs** — ineffective for neuropathic pain; appropriate only for nociceptive pain [cite:Harrison 21e Ch 384] 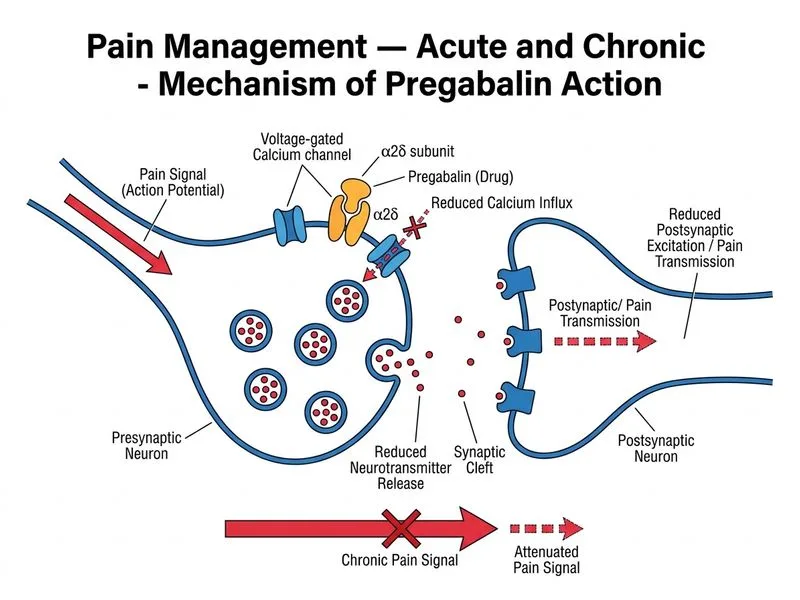
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.