## Clinical Scenario: Inadequately Controlled Cancer Pain This patient has severe pain on a moderate opioid dose (morphine 60 mg/day) with no signs of opioid toxicity (no respiratory depression, confusion, or excessive sedation). The pain is nociceptive (aching, movement-related) from bone and visceral metastases. ## Opioid Titration in Cancer Pain **Key Point:** In cancer pain, opioid doses should be titrated upward until adequate analgesia is achieved or intolerable side effects develop. There is no ceiling dose for opioids in cancer pain management. **High-Yield:** WHO Analgesic Ladder for Cancer Pain: 1. Non-opioid ± adjuvant (mild pain) 2. Weak opioid ± non-opioid ± adjuvant (mild-moderate pain) 3. Strong opioid ± non-opioid ± adjuvant (moderate-severe pain) **Mnemonic: DOSE ESCALATION RULE — "Increase by 25–50% every 48–72 hours if inadequate analgesia and no toxicity" - This patient is at 60 mg/day → escalate to 90 mg/day (50% increase) - Reassess after 48–72 hours - Continue until pain controlled or side effects limit further increase ## Comparison of Opioid Management Strategies | Strategy | Indication | Evidence | Risk | |----------|-----------|----------|------| | **Dose escalation (correct)** | Inadequate analgesia, no toxicity | Standard of care (WHO, ASCO, NCCN) | Rare if titrated carefully | | **Opioid switching** | Intolerable side effects (e.g., nausea, constipation) OR possible tolerance | Equianalgesic conversion needed | Incomplete cross-tolerance; requires careful dosing | | **Adjuvant addition alone** | Neuropathic component OR to reduce opioid requirement | Supportive, not primary for nociceptive pain | Delays adequate analgesia | | **Methadone monotherapy** | Specialized setting (opioid-induced hyperalgesia, renal failure) | Requires expertise; high risk of overdose | Narrow therapeutic window; long half-life | **Clinical Pearl:** "Opioid tolerance" is often misdiagnosed; what appears to be tolerance is usually disease progression (increasing tumor burden, new metastases) or inadequate dosing. True pharmacological tolerance develops slowly over months. ## Pain Management Algorithm for Cancer Pain ```mermaid flowchart TD A["Cancer pain on opioid"]:::outcome --> B{"Pain controlled?"}:::decision B -->|Yes| C["Continue current dose; monitor"]:::action B -->|No| D{"Opioid toxicity present?"}:::decision D -->|Yes| E["Reduce dose or switch opioid"]:::action D -->|No| F["Increase opioid by 25–50%"]:::action F --> G["Reassess in 48–72 hours"]:::action G --> H{"Adequate analgesia?"}:::decision H -->|Yes| I["Establish maintenance dose"]:::action H -->|No| J["Repeat escalation cycle"]:::action E --> K{"Neuropathic component?"}:::decision K -->|Yes| L["Add gabapentinoid or SNRI"]:::action K -->|No| M["Manage side effects"]:::action ``` **Key Point:** Adjuvants (pregabalin, duloxetine, NSAIDs, corticosteroids) are added to optimize analgesia and reduce opioid requirements, but they do NOT replace opioid escalation when pain is inadequately controlled. **Warning:** Opioid switching (option B) is appropriate when side effects limit further escalation (e.g., severe nausea, constipation, sedation), NOT when pain is simply inadequate. This patient has no documented toxicity, so dose escalation is the first step. 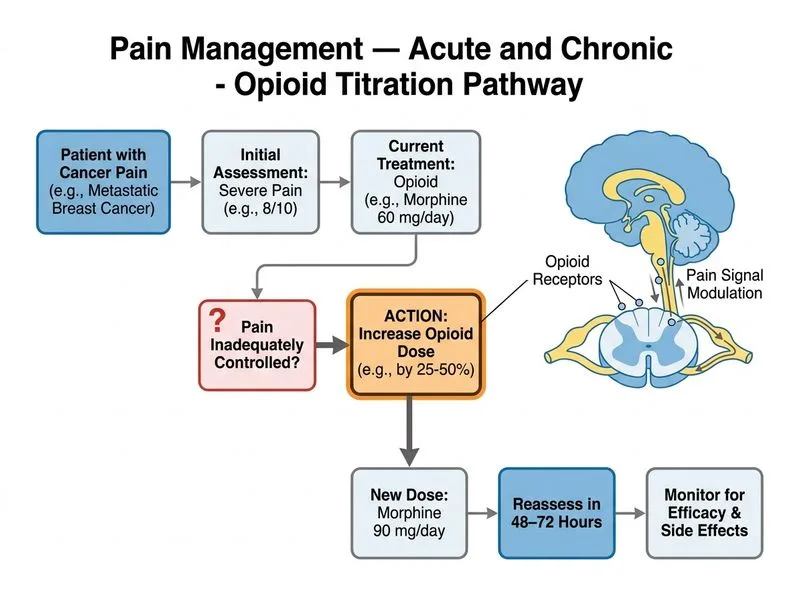
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.