## Clinical Scenario: Cancer Pain with Celiac Plexus Involvement **Key Point:** This patient has opioid-refractory visceral cancer pain due to celiac plexus infiltration. Celiac plexus neurolysis is the gold-standard interventional approach for rapid, durable pain relief in this setting. ### Celiac Plexus Neurolysis: Indications and Efficacy **High-Yield:** Celiac plexus neurolysis is indicated for: - Visceral upper abdominal pain from pancreatic, gastric, or hepatic malignancy - Pain refractory to optimized systemic opioid therapy - Patients with adequate performance status for a minimally invasive procedure ### Technique Comparison | Approach | Route | Advantage | Disadvantage | |---|---|---|---| | **EUS-guided neurolysis** | Endoscopic ultrasound | Direct visualization, high accuracy, rapid onset (24–48 hrs), low morbidity | Requires endoscopy expertise; not universally available | | **CT-guided percutaneous** | Percutaneous needle | Widely available, real-time imaging | Slightly higher morbidity; delayed onset (3–7 days) | | **Fluoroscopy-guided** | Retrocrural approach | Traditional, reproducible | Operator-dependent; higher risk of vascular injury | **Clinical Pearl:** EUS-guided celiac plexus neurolysis achieves pain relief in 80–90% of patients with pancreatic cancer pain, with onset within 24–48 hours. Duration of benefit is typically 4–12 weeks, after which repeat procedures can be performed if needed. ### Mechanism of Pain Relief Celiac plexus neurolysis involves injection of alcohol (95–100%) or phenol into or around the celiac plexus, causing chemical destruction of visceral afferent fibers. This interrupts pain transmission from upper abdominal viscera without affecting somatic sensation or motor function. **Mnemonic: VISCERAL pain pathway** — Visceral afferents → Splanchnic nerves → Celiac plexus → Dorsal root ganglia → Spinal cord. Neurolysis blocks this at the plexus level. ### Why Systemic Escalation Alone Is Inadequate This patient is already on a high-dose opioid (120 mg morphine daily). Further escalation risks: - Dose-limiting side effects (sedation, constipation, respiratory depression) - Incomplete analgesia for visceral pain (opioid-refractory component) - Prolonged symptom burden while titrating Interventional neurolysis provides rapid, targeted relief without additional systemic drug burden. **Warning:** Celiac plexus neurolysis carries small risks of temporary diarrhea (due to loss of sympathetic tone), orthostatic hypotension, and rare vascular injury. However, these are outweighed by the benefit in end-stage cancer pain. 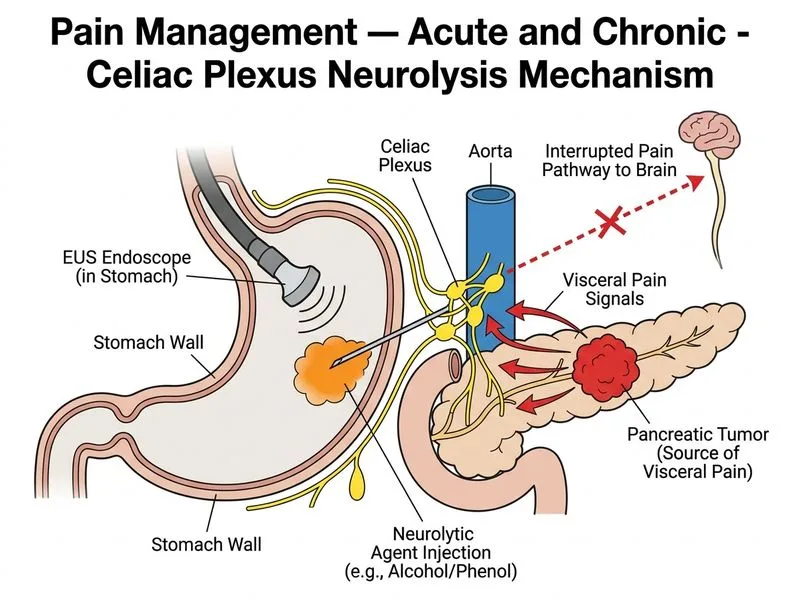
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.