## Neurolytic Superior Hypogastric Plexus Block — Contraindications **Key Point:** Neurolytic blocks use chemical agents (phenol, alcohol) that diffuse through tissue and carry risk of neurotoxicity, vascular injury, and organ damage. Coagulopathy is a **relative contraindication** that significantly increases bleeding and hematoma risk. ### Why Coagulopathy/Liver Disease is Most Important: - **Mechanism:** Neurolytic procedures involve needle placement near major vessels (aorta, iliac vessels) and the superior hypogastric plexus. - **Risk:** In a coagulopathic patient, even minor vascular puncture can lead to retroperitoneal hemorrhage, which is difficult to control and may be fatal. - **Liver disease** → impaired synthesis of clotting factors (II, V, VII, IX, X) and thrombocytopenia → increased bleeding tendency. - **Clinical consequence:** Uncontrolled retroperitoneal bleed in a cachetic, malnourished patient with already compromised organ function carries high mortality. ### Why This Patient's Liver Disease is Particularly Relevant: - Chronic pancreatitis often leads to **secondary biliary cirrhosis** and portal hypertension. - Deranged LFTs indicate synthetic dysfunction (not just cholestasis). - **INR elevation** (if present) is a direct contraindication to neurolytic blocks. **High-Yield:** Before any neurolytic block, always check **PT/INR, aPTT, platelet count**. If INR >1.5 or platelets <50,000, consider alternative analgesia (intrathecal opioids, epidural infusions, or systemic analgesics with hepatic dose adjustment). ### Why Other Options Are NOT the Primary Contraindication: - **Failed celiac plexus block:** Not a contraindication; it indicates need for alternative approach (e.g., superior hypogastric block is actually a valid next step). - **Cachexia/malnutrition:** A risk factor for poor wound healing and infection, but not a direct contraindication to the block itself. - **Age and gender:** Not contraindications; neurolytic blocks are performed across all ages if other criteria are met. 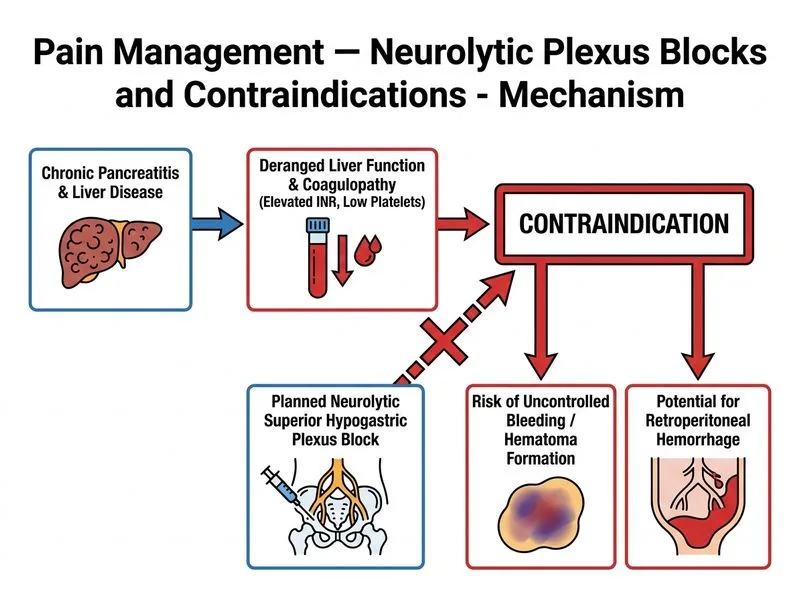
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.