## Clinical Diagnosis: Optic Neuritis (Papillitis) ### Key Distinguishing Features **Key Point:** Optic neuritis presents with **acute vision loss, pain on eye movement, and disc hyperaemia in a young patient with demyelinating disease**. The clinical presentation strongly suggests **papillitis** (anterior optic neuritis): | Feature | Papillitis (Optic Neuritis) | Papilloedema | AION | |---------|---------------------------|-------------|------| | **Vision loss** | Acute, marked (6/36–6/60) | Gradual or none initially | Acute, altitudinal | | **Pain** | Yes, pain on eye movement | No pain | No pain | | **Disc appearance** | Hyperaemic, blurred margins | Blurred margins, elevated | Pale, sectoral | | **Exudates** | Often present around disc | Peripapillary | Rare | | **Pupil** | Relative afferent pupillary defect (RAPD) | Normal | May have RAPD | | **IOP** | Normal | Normal or elevated | Normal | | **Association** | MS, demyelinating disease | Intracranial hypertension | Age >50, vascular risk | ### Clinical Reasoning 1. **Age and demographics:** 28-year-old woman with known MS — optic neuritis is the presenting feature in ~20% of MS patients and occurs in ~50% over the disease course. 2. **Pain on eye movement:** Pathognomonic for inflammation of the optic nerve sheath; absent in papilloedema. 3. **Acute vision loss:** Typical of demyelinating optic neuritis; papilloedema causes gradual visual blurring. 4. **Disc hyperaemia:** Indicates inflammation of the nerve head; papilloedema shows elevation without hyperaemia initially. 5. **Normal IOP:** Rules out glaucoma. **High-Yield:** Optic neuritis is the **most common cause of optic nerve inflammation in young adults** and is strongly associated with MS, particularly in women aged 20–40 years. **Clinical Pearl:** The presence of **pain on eye movement** is the single most useful clinical sign to differentiate optic neuritis from papilloedema. This pain results from inflammation of the dura surrounding the optic nerve. ### Pathophysiology Optic neuritis is a demyelinating inflammation of the optic nerve, often the first manifestation of multiple sclerosis. The inflammatory process affects the myelin sheath, leading to: - Conduction block and vision loss - Optic nerve swelling (if anterior — papillitis) - Relative afferent pupillary defect (RAPD) ### Management Implications - **MRI brain and orbits:** To assess for demyelinating lesions and confirm MS diagnosis. - **High-dose IV methylprednisolone:** 1 g daily for 3–5 days, followed by oral taper (accelerates visual recovery). - **Neuroimaging:** To rule out structural lesions and assess MS burden. [cite:Harrison 21e Ch 378] 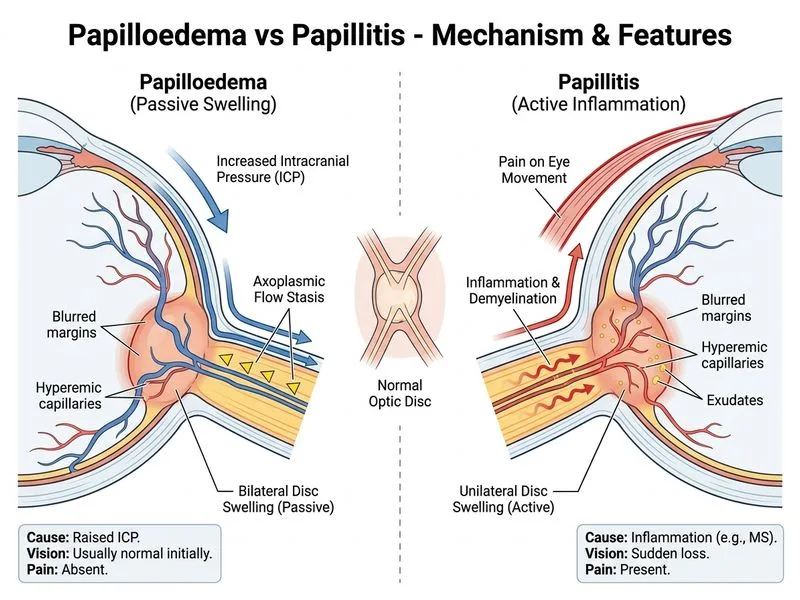
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.