## Clinical Diagnosis: Papilloedema from Raised Intracranial Pressure ### Key Distinguishing Features **Key Point:** Papilloedema is a sign of raised intracranial pressure (ICP), characterised by **bilateral disc swelling, obscured vessels, absent spontaneous venous pulsations, and preserved vision initially**. ### Pathophysiology of Papilloedema 1. Space-occupying lesion (posterior fossa mass) → obstruction of CSF flow 2. Elevated ICP → impaired axoplasmic flow in optic nerve 3. Accumulation of axoplasmic debris → disc swelling 4. **Bilateral involvement** (both optic nerves affected equally) 5. Progressive if untreated → optic atrophy and vision loss ### Comparison: Papilloedema vs Papillitis | Feature | Papilloedema | Papillitis (Optic Neuritis) | |---------|--------------|-----------------------------| | **Onset** | Gradual (days to weeks) | Acute (hours to 24 hrs) | | **Laterality** | **Bilateral** | **Unilateral** | | **Vision loss** | Late/absent initially | Early, marked | | **Pain** | Absent | Present (pain on eye movement) | | **RAPD** | Absent | Present (unilateral) | | **Disc swelling** | Hyperaemia, blurred margins, obscured vessels | Hyperaemia, blurred margins, flame haemorrhages | | **Spontaneous venous pulsations** | Absent | Present | | **Associated symptoms** | Headache, nausea, transient visual obscurations | Demyelinating disease history | | **Aetiology** | Raised ICP (mass, hydrocephalus, pseudotumour) | Demyelination (MS, NMO) | **High-Yield:** The **absence of pain on eye movement** and **bilateral disc swelling** in a patient with imaging evidence of a mass and raised ICP strongly favour papilloedema over optic neuritis. ### Clinical Features of Papilloedema (Frisén Scale) **Mnemonic: SWOLLEN DISC = Swelling (bilateral), Wiped-out margins, Obscured vessels, Layered appearance, Loss of spontaneous pulsations, Enlarged blind spot, Disc hyperaemia, Indistinct nasal border** 1. **Early papilloedema:** Blurring of nasal disc margin, obscuration of vessels at disc edge 2. **Established papilloedema:** Complete obscuration of disc margins, elevation of disc (0.5–2 diopters), hyperaemia 3. **Chronic papilloedema:** Gliosis, optociliary shunt vessels, hard exudates (macular star), peripapillary haemorrhages 4. **Atrophic papilloedema:** Optic atrophy with persistent disc elevation ("waxy pallor") **Clinical Pearl:** Absence of spontaneous venous pulsations is a sensitive sign of raised ICP but not specific (absent in 20% of normal individuals). Obliteration of spontaneous pulsations (previously present) is more specific. ### Why This Patient Has Papilloedema, Not Papillitis - **Bilateral disc swelling** rules out papillitis (unilateral) - **No pain on eye movement** excludes optic neuritis - **Preserved visual acuity (6/6)** is typical of early papilloedema; papillitis causes acute severe loss - **No RAPD** indicates bilateral, symmetric involvement (papilloedema); RAPD is pathognomonic for unilateral optic nerve disease - **Imaging evidence of mass with raised ICP** is the direct cause of papilloedema - **Gradual onset** (6 weeks) fits papilloedema; papillitis is acute ### Management Implications ```mermaid flowchart TD A[Papilloedema confirmed]:::outcome --> B[Treat underlying cause]:::action B --> C{Space-occupying lesion?}:::decision C -->|Yes| D[Neurosurgical intervention]:::action C -->|No| E[Medical management]:::action E --> F[Acetazolamide, fluid restriction]:::action D --> G[Monitor disc appearance & VF]:::action G --> H{Vision threatened?}:::decision H -->|Yes| I[Urgent intervention]:::urgent H -->|No| J[Follow-up imaging & ophthalmology]:::action ``` [cite:Harrison 21e Ch 379; Kline & Bajandas Neuro-Ophthalmology] 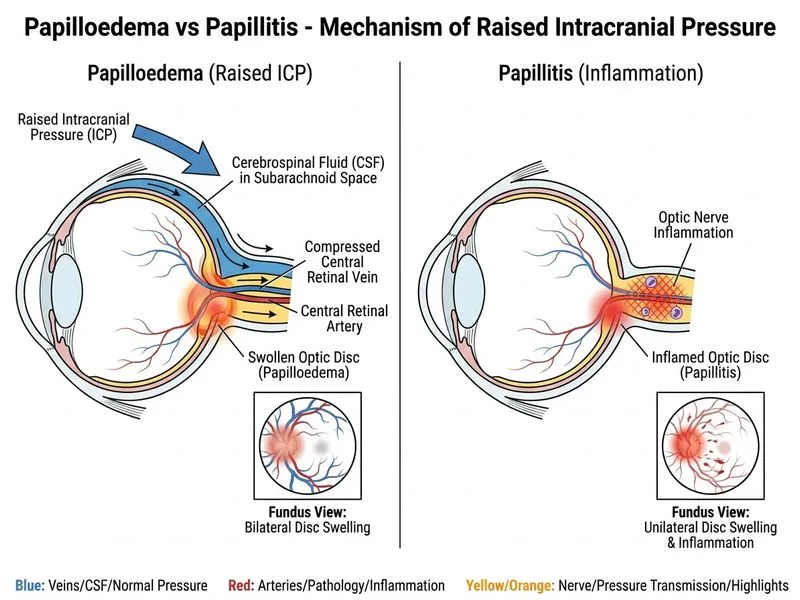
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.