## Clinical Diagnosis: Papilloedema from Raised Intracranial Pressure ### Key Clinical Features **Key Point:** Papilloedema is bilateral optic disc swelling caused by raised intracranial pressure (ICP). It is painless and vision is preserved until late stages. ### Clinical Presentation Analysis This patient exhibits the classic presentation of papilloedema: 1. **Insidious onset** (3 weeks of progressive symptoms) 2. **Bilateral optic disc swelling** with blurred margins 3. **Systemic signs of raised ICP:** headache, nausea, hypertension (160/100) 4. **Preserved visual acuity** (6/6 bilaterally) — vision loss is a **late feature** 5. **No pain on eye movement** — distinguishes from optic neuritis 6. **Normal pupils** — no RAPD 7. **Paton's lines** (retinal folds) — pathognomonic for papilloedema ### Papilloedema vs Papillitis (Optic Neuritis): Differential | Feature | Papilloedema | Papillitis (Optic Neuritis) | |---------|--------------|---------------------------| | **Onset** | Insidious (days to weeks) | Acute (hours to days) | | **Bilaterality** | Bilateral (usually) | Unilateral | | **Vision loss** | Late finding; early vision preserved | Early and marked | | **Pain on eye movement** | Absent | Present | | **RAPD** | Absent (or bilateral if severe) | Present (unilateral) | | **Systemic signs** | Headache, nausea, vomiting, hypertension | Neurological signs (MS, infection) | | **Disc appearance** | Hyperaemia, venous engorgement, Paton's lines, cotton-wool spots | Hyperaemia, blurred margins, less venous engorgement | | **Aetiology** | Raised ICP (tumour, hydrocephalus, pseudotumor cerebri, hypertensive emergency) | Demyelination, infection, inflammation | **High-Yield:** **Paton's lines** (retinal folds radiating from the optic disc) are virtually pathognomonic for papilloedema and distinguish it from other causes of disc swelling. ### Mechanism of Papilloedema ```mermaid flowchart TD A[Raised Intracranial Pressure]:::urgent --> B[Impaired axoplasmic flow in optic nerve] B --> C[Accumulation of axonal material at disc] C --> D[Optic disc swelling - Papilloedema] D --> E[Venous engorgement] D --> F[Retinal folds - Paton's lines] D --> G[Cotton-wool spots, flame haemorrhages] E --> H[Late: Vision loss] F --> H ``` ### Stages of Papilloedema **Mnemonic: CHOKED DISC** - **C**ircumferential blurring of disc margins - **H**yperemia of the disc - **O**bliteration of physiological cup - **K**ey feature: venous engorgement - **E**levation of disc margins - **D**ilatation of blind spot - **I**ntact vision (early) - **S**welling extends beyond disc - **C**otton-wool spots and haemorrhages **Clinical Pearl:** Early papilloedema is characterized by **preserved vision**. Once vision loss occurs, chronic papilloedema with optic atrophy has likely developed — this is a medical emergency requiring urgent ICP management. ### Why Bilateral Optic Neuritis Is Ruled Out - Bilateral optic neuritis is **rare** (optic neuritis is typically unilateral) - **Pain on eye movement is absent** in this patient - No RAPD (optic neuritis causes RAPD) - **Insidious 3-week onset** is inconsistent with the acute presentation of optic neuritis - Demyelinating disease (MS) would not explain the hypertension and systemic signs of raised ICP [cite:Harrison 21e Ch 428; Neuro-Ophthalmology] 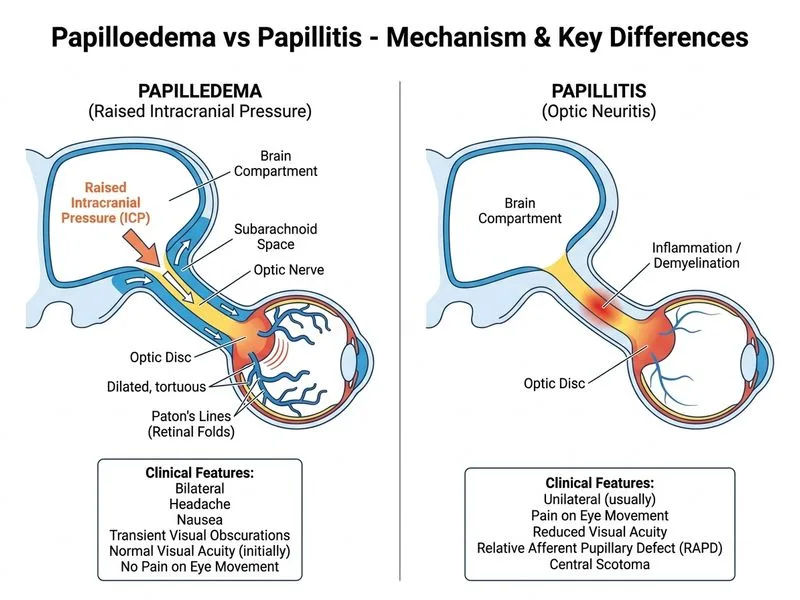
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.