## Clinical Diagnosis: Papilloedema from Raised Intracranial Pressure ### Key Distinguishing Features **Key Point:** Papilloedema is the optic disc swelling caused by raised intracranial pressure. It is bilateral, painless, and associated with progressive headache, nausea, and vomiting. ### Differential Diagnosis: Papilloedema vs Papillitis | Feature | Papilloedema | Papillitis (Optic Neuritis) | |---------|--------------|-----------------------------| | **Etiology** | Raised intracranial pressure | Demyelinating inflammation of optic nerve | | **Onset** | Insidious, progressive (weeks to months) | Acute (hours to days) | | **Bilaterality** | Bilateral (always) | Unilateral (typically) | | **Pain** | Absent or mild headache (from ICP) | Acute eye pain, worse with movement | | **Vision loss** | Late finding; preserved until advanced | Early; central scotoma | | **Visual field defect** | Peripheral constriction, arcuate defects | Central scotoma | | **Disc appearance** | Blurred margins, hyperaemia, exudates, hemorrhages, cotton-wool spots | Hyperaemia, swelling, less hemorrhage | | **Pupil** | Normal (no RAPD) | RAPD present | | **Systemic signs** | Headache, nausea, vomiting, papilloedema headache | Eye pain, neurological signs of MS | | **Imaging** | Mass, edema, hydrocephalus, hemorrhage | Optic nerve hyperintensity; brain lesions suggest MS | **High-Yield:** The combination of **bilateral disc swelling + painless + normal vision + headache/nausea/vomiting + imaging evidence of raised ICP = papilloedema**. ### Why This Is Papilloedema 1. **Bilateral optic disc swelling** — papilloedema is always bilateral; optic neuritis is unilateral. 2. **Painless** — no pain on eye movement; papillitis is painful. 3. **Preserved visual acuity (6/6)** — papilloedema preserves vision until late stages; papillitis causes early vision loss. 4. **Normal visual fields** — papilloedema may show peripheral constriction, but early papilloedema can have normal fields; papillitis causes central scotoma. 5. **Progressive headache, nausea, vomiting** — classic signs of raised ICP. 6. **MRI shows posterior fossa mass with hydrocephalus** — obstructive hydrocephalus is a direct cause of raised ICP and papilloedema. ### Stages of Papilloedema (Frisén Scale) **Mnemonic: CHOPS** — **C**ircumferential, **H**yperemia, **O**bliteration of margins, **P**eripapillary exudates, **S**welling 1. **Stage 0:** Normal disc. 2. **Stage 1:** C-sign (circumferential halo of obscuration at disc margin). 3. **Stage 2:** Obscuration of nasal margin; hyperaemia of disc. 4. **Stage 3:** Complete obscuration of disc margins; exudates and hemorrhages. 5. **Stage 5:** Optic atrophy with persistent disc swelling. This patient shows Stage 3–4 papilloedema. ### Clinical Pearl **Clinical Pearl:** Papilloedema is a sign of raised ICP, not a diagnosis. The underlying cause (here, posterior fossa mass with obstructive hydrocephalus) must be identified and treated urgently. Neurosurgical consultation for mass resection or ventriculoperitoneal shunt is indicated. ### Management 1. **Urgent neurosurgery consultation** — posterior fossa mass with obstructive hydrocephalus. 2. **Imaging:** MRI brain with contrast; CT if MRI contraindicated. 3. **Lumbar puncture:** Contraindicated in this case (risk of herniation with mass effect). 4. **Acetazolamide:** May reduce CSF production; not definitive treatment. 5. **Surgical intervention:** Tumor resection ± ventriculoperitoneal shunt. [cite:Harrison 21e Ch 428; Neuro-Ophthalmology (Kaufman)] 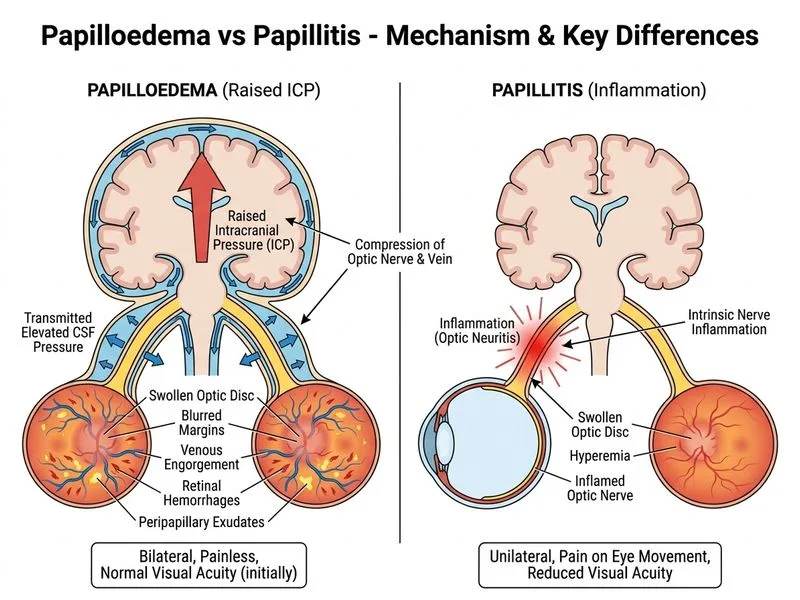
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.