## First-Line Structural Neuroimaging in Parkinson Disease **Key Point:** MRI brain with standard sequences (T1, T2, FLAIR) is the most appropriate first-line structural neuroimaging investigation in suspected Parkinson disease. It excludes structural mimics (tumors, stroke, hydrocephalus, atrophy patterns) and identifies red flags suggestive of atypical parkinsonian syndromes. **High-Yield:** MRI findings that raise suspicion for **atypical parkinsonism** rather than idiopathic PD include: - **Midbrain atrophy** (PSP) - **Putaminal rim sign** or **hot cross bun sign** (MSA) - **Cerebellar atrophy** (MSA-C) - **Cortical atrophy** (CBD) - **Periventricular white matter changes** (vascular parkinsonism) - **Ventriculomegaly** (normal-pressure hydrocephalus) **Clinical Pearl:** In idiopathic PD, MRI is typically **normal or shows only mild nonspecific changes**. The absence of red flags on MRI, combined with excellent levodopa response and asymmetric onset, supports the diagnosis of idiopathic PD. **Mnemonic:** MRI **rules out mimics** — structural lesions, atypical patterns, and secondary causes. It is the gatekeeper investigation before functional imaging. ## Role of Each Investigation in PD Diagnosis | Investigation | Purpose | When to Use | Limitation | | --- | --- | --- | --- | | MRI brain (T1/T2/FLAIR) | Exclude structural mimics; identify atypical patterns | **First-line** in all suspected PD | Does not assess dopaminergic function | | 123I-FP-CIT SPECT | Confirm dopaminergic denervation | After MRI if diagnosis remains uncertain | Functional imaging; requires nuclear medicine facility | | 18F-FDG PET | Identify metabolic patterns in atypical syndromes | Suspected atypical parkinsonism (PSP, MSA, CBD) | Not first-line for idiopathic PD confirmation | | Transcranial ultrasound | Assess substantia nigra echogenicity | Research tool; not routine clinical practice | Limited availability; operator-dependent | **Warning:** Do not skip MRI in the initial workup. Even though idiopathic PD is a clinical diagnosis, MRI is essential to exclude structural and secondary causes. Functional imaging (DaTscan) is reserved for cases where clinical diagnosis is uncertain after MRI has ruled out structural mimics. ## Diagnostic Algorithm ```mermaid flowchart TD A[Suspected Parkinson Disease]:::outcome --> B[Clinical assessment:<br/>asymmetric onset, rest tremor,<br/>rigidity, bradykinesia]:::action B --> C{Red flags for<br/>atypical syndrome?}:::decision C -->|Yes or uncertain| D[MRI brain with<br/>standard sequences]:::action C -->|No, typical PD| D D --> E{Structural lesion<br/>or atypical pattern?}:::decision E -->|Yes| F[Diagnosis: Secondary<br/>or atypical parkinsonism]:::outcome E -->|No| G{Clinical diagnosis<br/>still uncertain?}:::decision G -->|Yes| H[123I-FP-CIT SPECT<br/>DaTscan]:::action G -->|No| I[Diagnosis: Idiopathic PD]:::outcome H --> J{DAT loss<br/>present?}:::decision J -->|Yes| I J -->|No| K[Diagnosis: Essential tremor<br/>or other mimic]:::outcome ``` [cite:Harrison 21e Ch 429] 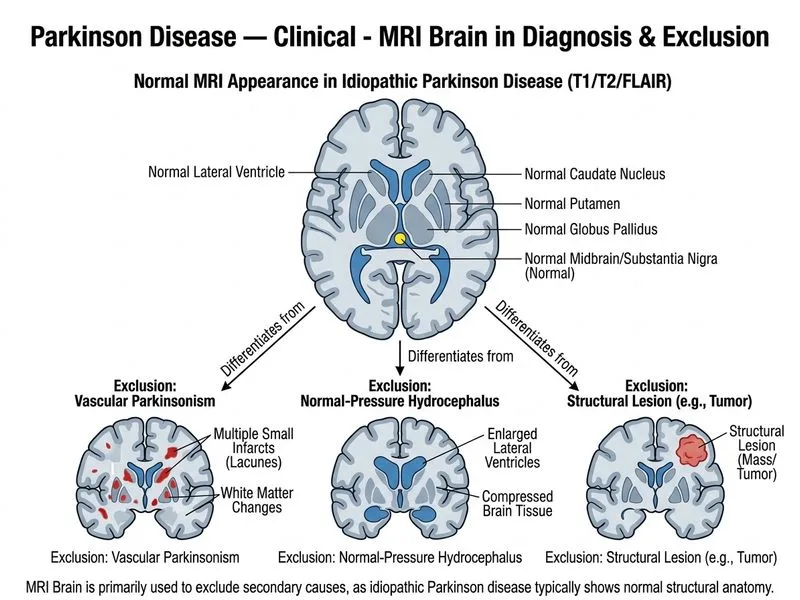
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.