## Clinical Diagnosis: Tubo-Ovarian Abscess (TOA) **Key Point:** This patient has a **tubo-ovarian abscess (TOA)** — a severe, localized suppurative collection within the adnexa, typically a complication of recurrent or inadequately treated PID. ### Diagnostic Criteria Present | Finding | Significance | |---------|-------------| | Recurrent PID history | Risk factor for abscess formation | | Fever + peritoneal signs | Acute inflammation/infection | | Palpable adnexal mass | Suggests localized collection | | Ultrasound: 6 cm complex cystic mass with internal echoes | Diagnostic for abscess (>4 cm = significant) | | Anemia (Hb 9.2) + leukocytosis | Chronic infection + acute inflammation | **High-Yield:** TOA occurs in 3.8% of PID cases and is the most common gynecologic surgical emergency in reproductive-age women [cite:Park 26e Ch 23]. ## Management Algorithm for TOA ```mermaid flowchart TD A[TOA diagnosed on imaging]:::outcome --> B{Abscess size & stability?}:::decision B -->|Small < 4 cm, stable| C[IV antibiotics alone]:::action B -->|Large ≥ 4 cm OR unstable| D[IV antibiotics + drainage]:::action C --> E[Repeat imaging at 72 hrs]:::action D --> F[Percutaneous/transvaginal drainage under ultrasound/CT]:::action E --> G{Response?}:::decision G -->|Good: fever down, WBC down| H[Continue IV antibiotics 48 hrs post-defervescence]:::action G -->|Poor: persistent fever/sepsis| I[Urgent drainage or surgery]:::urgent F --> J[Antibiotic course + follow-up imaging]:::action I --> K[Consider laparotomy if rupture/peritonitis]:::urgent ``` **Clinical Pearl:** The **4 cm threshold** is critical: - **< 4 cm:** Trial of antibiotics alone (success rate ~70%). - **≥ 4 cm:** Drainage + antibiotics (success rate > 90%) [cite:Harrison 21e Ch 137]. This patient's abscess is **6 cm** → **drainage is mandatory**. ## Antibiotic Regimen for TOA (IV) **Mnemonic:** **CFD** — *Cefoxitin + Fluoroquinolone (or doxycycline) + clindacin (Clindamycin)* | Agent | Dosing | Coverage | |-------|--------|----------| | Cefoxitin | 2 g IV Q6H | Gram-negative, anaerobes | | Doxycycline | 100 mg IV/PO BD | *Chlamydia*, gram-positive | | Clindamycin | 600 mg IV Q6–8H | Anaerobes, *Bacteroides* | **Why clindamycin?** TOA often involves polymicrobial infection with anaerobes; clindamycin provides superior anaerobic coverage compared to outpatient PID regimens. ## Drainage Technique - **Percutaneous catheter drainage** (PCD) via ultrasound or CT guidance is first-line. - **Transvaginal aspiration** is an alternative if abscess is accessible. - **Success rate:** 80–90% with antibiotics + drainage [cite:Park 26e Ch 23]. **Warning:** Surgery (hysterectomy/BSO) is reserved for: - Rupture with peritonitis/septic shock. - Failure of drainage + antibiotics. - Recurrent TOA despite adequate treatment. - This patient is not yet a surgical candidate. ## Why NOT the Other Options? **Option 2 (oral antibiotics alone):** Inadequate for a 6 cm abscess; requires IV therapy and drainage. **Option 3 (immediate hysterectomy/BSO):** Overly aggressive; fertility-sparing drainage + antibiotics should be attempted first. Surgery is a last resort. **Option 4 (IV antibiotics alone without drainage):** High failure rate (~40%) for large abscesses; risks rupture, septic shock, and prolonged hospitalization. 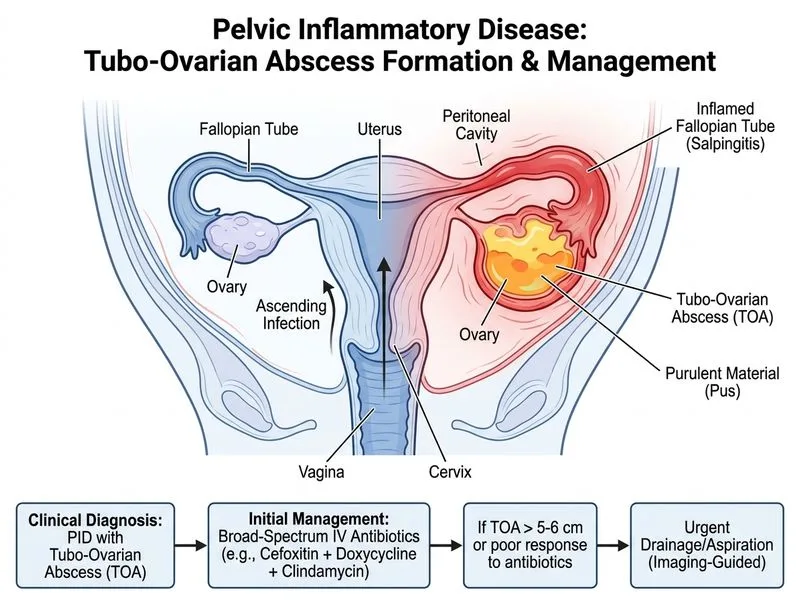
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.