## Diagnosis & Clinical Presentation **Key Point:** This patient meets diagnostic criteria for acute pelvic inflammatory disease (PID) with systemic toxicity (fever, elevated WBC, peritoneal signs) and imaging evidence of peritoneal involvement (free fluid). ## Diagnostic Criteria for PID Minimal criteria (any of the following in a woman with pelvic pain and no other cause identified): - Pelvic tenderness - Adnexal tenderness - Cervical motion tenderness Emphatic criteria supporting diagnosis: - Oral temperature >38.3°C - Abnormal cervical mucopurulent discharge or cervical friability - Presence of WBC on saline microscopy of vaginal fluid - Elevated erythrocyte sedimentation rate (ESR) - Elevated C-reactive protein (CRP) - Laboratory documentation of cervical infection with *N. gonorrhoeae* or *C. trachomatis* ## Management Algorithm ```mermaid flowchart TD A[Suspected PID]:::outcome --> B{Signs of systemic toxicity?}:::decision B -->|Yes: fever, elevated WBC, peritoneal signs| C[Inpatient parenteral antibiotics]:::action B -->|No: mild disease, reliable follow-up| D[Outpatient oral antibiotics]:::action C --> E[Ceftriaxone 250 mg IM/IV daily<br/>+ Doxycycline 100 mg PO BID<br/>± Metronidazole 500 mg PO/IV BID]:::action D --> F[Cefixime 400 mg PO single dose<br/>+ Azithromycin 1 g PO single dose]:::action E --> G[Transition to oral after clinical improvement]:::action F --> H[Re-evaluate at 48-72 hours]:::decision ``` ## Why Inpatient Parenteral Therapy? **High-Yield:** This patient has **severe PID** with: 1. Fever ≥38.5°C 2. Leukocytosis with left shift 3. Peritoneal signs (rebound tenderness) 4. Imaging evidence of peritonitis (free fluid) 5. Bilateral adnexal involvement These features indicate systemic toxicity and risk of progression to tubo-ovarian abscess or sepsis. Parenteral antibiotics achieve higher tissue concentrations and are mandatory. ## Antibiotic Regimen | Drug | Dose | Indication | |------|------|------------| | Ceftriaxone | 250 mg IM/IV daily | 3rd-generation cephalosporin; covers *N. gonorrhoeae* | | Doxycycline | 100 mg PO/IV BID | Covers *C. trachomatis*, atypical organisms | | Metronidazole | 500 mg PO/IV BID | Anaerobic coverage (optional but recommended) | **Clinical Pearl:** Transition to oral antibiotics (doxycycline 100 mg BID × 14 days total) once clinical improvement occurs (typically 24–48 hours of parenteral therapy). ## Follow-Up - Clinical reassessment at 48–72 hours - If no improvement: consider imaging (ultrasound/CT) to rule out tubo-ovarian abscess - Test of cure not routinely recommended; test for cure only if symptoms persist - Partner notification and treatment for sexually transmitted infections [cite:Park 26e Ch 16] 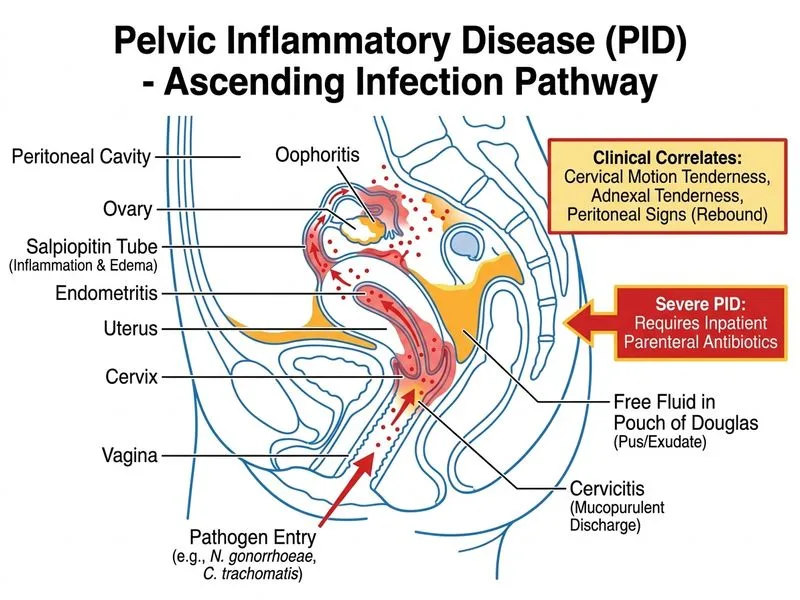
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.