## Clinical Presentation & Diagnosis **Key Point:** This patient has **tubo-ovarian abscess (TOA)**, a suppurative complication of PID, evidenced by: - Subacute presentation (10 days) - History of untreated chlamydial infection (major risk factor) - Pelvic tenderness with adnexal mass - Imaging: complex adnexal mass with internal echoes (pus) - Negative β-hCG (rules out ectopic pregnancy) ## Pathophysiology of TOA Formation ```mermaid flowchart TD A[Untreated chlamydial/gonococcal infection]:::outcome --> B[Ascending infection via fallopian tube]:::action B --> C[Acute salpingitis + endometritis]:::outcome C --> D{Delayed/inadequate treatment?}:::decision D -->|Yes| E[Localized suppuration in tube + ovary]:::action E --> F[Tubo-ovarian abscess formation]:::outcome D -->|No| G[Resolution with appropriate antibiotics]:::action F --> H{Rupture?}:::decision H -->|Yes| I[Peritonitis, sepsis, shock]:::urgent H -->|No| J[Percutaneous drainage ± antibiotics]:::action ``` ## Risk Factors for TOA | Risk Factor | Mechanism | |---|---| | Untreated/delayed-treatment STI | Allows ascending infection to progress | | Nulliparity | Tighter cervical os; impaired drainage | | IUD use | Increased risk of upper genital tract infection | | Recurrent PID | Repeated episodes increase abscess risk | | Immunosuppression | Reduced local/systemic immune response | **High-Yield:** TOA occurs in ~10–15% of women with acute PID, especially if treatment is delayed or inadequate. ## Imaging Characteristics **Ultrasound findings of TOA:** - Complex adnexal mass (4–10 cm typical) - Internal echoes (debris, pus, fibrin) - Thick, irregular walls - May be unilocular or multilocular - Free fluid in pouch of Douglas **Clinical Pearl:** The presence of a **complex adnexal mass** in the context of PID symptoms and history of untreated STI is pathognomonic for TOA until proven otherwise. ## Management of TOA ### Non-Ruptured TOA 1. **Inpatient parenteral antibiotics** (same as severe PID): - Ceftriaxone 250 mg IV daily - Doxycycline 100 mg IV/PO BID - Metronidazole 500 mg IV BID 2. **Duration:** 14 days total (parenteral until clinical improvement, then oral to complete course) 3. **Imaging follow-up:** Repeat ultrasound at 48–72 hours 4. **Percutaneous drainage:** Consider if: - No clinical improvement after 48–72 hours of antibiotics - Abscess >4 cm - Immunocompromised host - Ruptured abscess ### Ruptured TOA - **Surgical emergency** - Immediate exploratory laparotomy - Drainage of abscess ± hysterectomy ± bilateral salpingo-oophorectomy (depending on fertility desires) - High-dose parenteral antibiotics - ICU monitoring for sepsis **Mnemonic: TOAST** (TOA features) - **T**ender adnexal mass - **O**varian involvement (tubo-ovarian) - **A**bscess (suppurative collection) - **S**epsis risk (if ruptured) - **T**reatment: antibiotics ± drainage ## Differential Diagnosis Exclusion | Diagnosis | Why Excluded | |---|---| | Ovarian torsion | Acute severe pain (not 10-day subacute course); no fever; β-hCG negative; imaging shows complex mass, not hemorrhagic infarction | | Ruptured cyst | Chemical peritonitis is acute/severe; no fever; no adnexal mass; no history of STI | | Ovarian fibroid | Fibroids are benign, non-infected; no fever; no STI history; imaging appearance differs | [cite:Park 26e Ch 16; Berek & Novak 16e Ch 11] 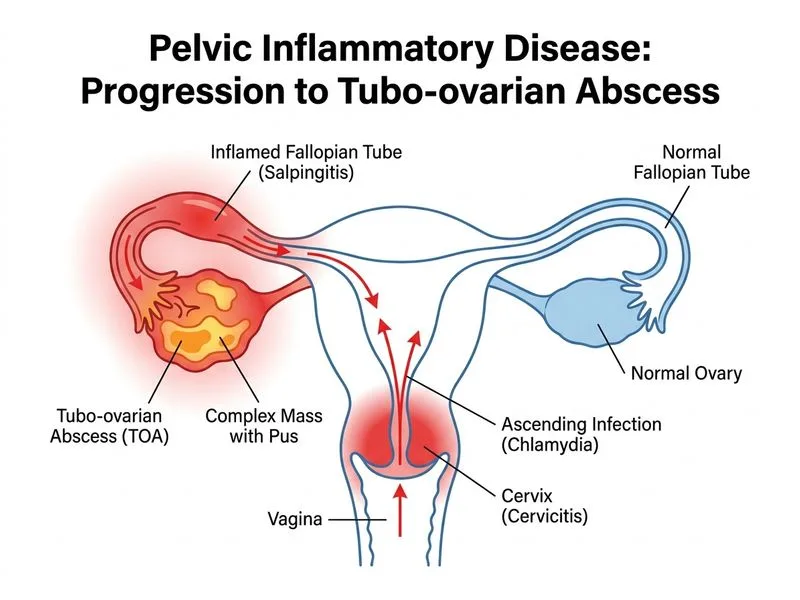
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.