## Pathogenic Mechanism of NSAID-Induced Peptic Ulcer **Key Point:** NSAIDs (including aspirin) inhibit cyclooxygenase (COX-1 and COX-2), blocking prostaglandin E~2~ (PGE~2~) and prostacyclin synthesis. This leads to: 1. Decreased mucus secretion 2. Reduced bicarbonate secretion by gastric epithelium 3. Impaired mucosal blood flow 4. Loss of the protective barrier ### Clinical Context in This Case - **NSAID exposure:** Daily aspirin for 3 months - **H. pylori negative:** Rules out infectious etiology - **Anterior duodenal ulcer with visible vessel:** Classic presentation of NSAID-induced ulcer; anterior wall ulcers are prone to erosion into the gastroduodenal artery, causing hemorrhage - **Anemia:** Suggests chronic blood loss from the ulcer ### Pathophysiology of NSAID-Induced Ulcers | Feature | NSAID-Induced | H. pylori-Induced | |---------|---------------|-------------------| | **Location** | Duodenum (anterior wall) | Antrum, lesser curve | | **Acid secretion** | Normal or ↓ | ↑ (due to gastritis) | | **Mechanism** | ↓ PGE~2~ → ↓ mucus/HCO~3~^−^ | Inflammation → ↑ gastrin | | **H. pylori serology** | Negative | Positive | | **Risk of perforation** | High (anterior wall) | Lower | **High-Yield:** NSAID-induced ulcers account for ~25% of peptic ulcer disease in developed countries. The anterior duodenal wall location is critical because the gastroduodenal artery runs posteriorly; anterior ulcers erode anteriorly and may perforate, while posterior ulcers erode into the artery causing hemorrhage. **Clinical Pearl:** The visible vessel at the base is a Forrest Ia/Ib lesion and indicates active or recent bleeding — a high-risk finding requiring endoscopic hemostasis. [cite:Robbins 10e Ch 17] 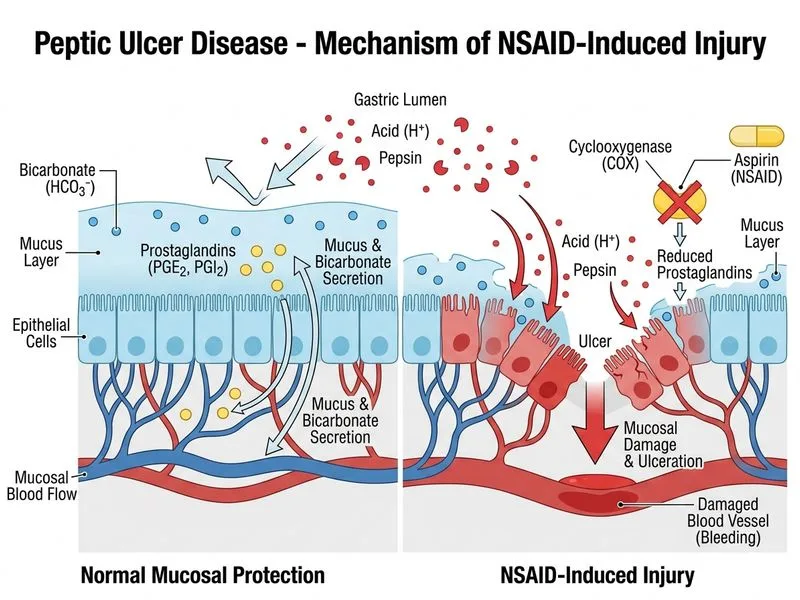
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.