## Clinical Presentation and Diagnosis The clinical and imaging findings are classic for a **branchial cleft cyst** — a congenital anomaly arising from incomplete obliteration of the second branchial cleft (most common type). The key diagnostic clues are: - **Age:** Typically presents in early childhood or young adulthood - **Location:** Anterior triangle of neck, just below the angle of the mandible (along the anterior border of sternocleidomastoid) - **Character:** Soft, compressible, transilluminant (fluid-filled) - **Imaging:** Ultrasound shows a simple cyst with no internal echoes ## Why Surgical Excision is the Correct Answer **Key Point:** Branchial cleft cysts do **not** regress spontaneously and carry a significant risk of recurrent infection, abscess formation, and fistula development if left untreated. The standard of care — as per Scott-Brown's Otorhinolaryngology, Bailey & Love's Surgery, and Cummings Otolaryngology — is **complete surgical excision** once the diagnosis is established. **High-Yield:** Unlike cystic hygromas (lymphangiomas), branchial cleft cysts: - Do NOT undergo spontaneous regression - Have a well-defined surgical indication regardless of symptoms - Carry risk of recurrent infection and, rarely, malignant transformation if untreated - Are best excised electively under general anaesthesia in a child who is otherwise well ## Why Other Options Are Incorrect 1. **Option A (Oral antibiotics and warm compresses):** Appropriate only if the cyst is acutely infected; not a definitive treatment and does not address the underlying anomaly. 2. **Option B (FNAC):** Ultrasound already confirms a simple cystic lesion; FNAC is not required and does not change management. Definitive treatment is surgical. 3. **Option D (Observation with serial ultrasound):** Appropriate for cystic hygromas (lymphangiomas) which can regress spontaneously, but NOT for branchial cleft cysts, which require excision to prevent complications. ## Distinguishing Branchial Cleft Cyst from Cystic Hygroma | Feature | Branchial Cleft Cyst | Cystic Hygroma | |---|---|---| | Origin | 2nd branchial cleft | Lymphatic malformation | | Location | Anterior SCM border | Posterior triangle / submandibular | | Transillumination | Yes | Yes | | Spontaneous regression | No | Up to 50–60% | | Management | Surgical excision | Observation ± sclerotherapy | **Clinical Pearl (Bailey & Love):** All branchial cleft cysts should be surgically excised once diagnosed, ideally in a quiescent (non-infected) period, to prevent recurrent infections and fistula formation. Delay increases surgical difficulty due to pericystic fibrosis from repeated infections. 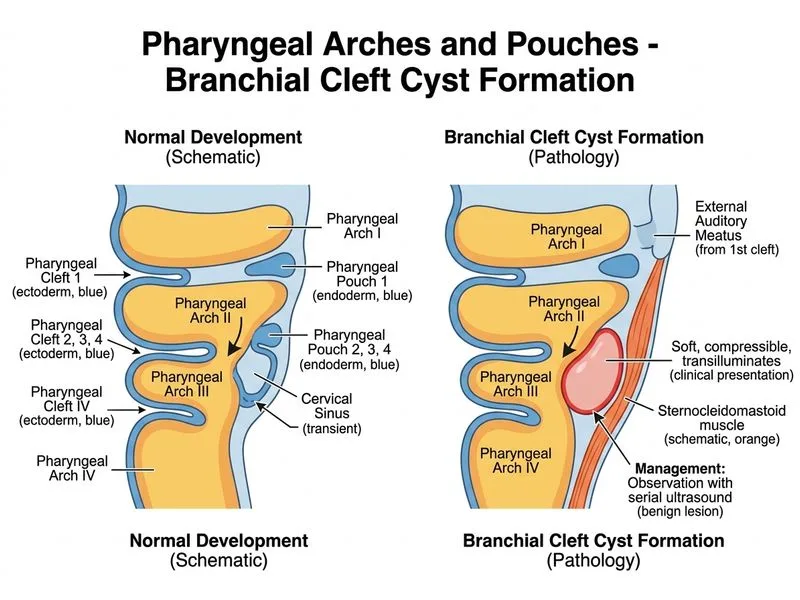
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.