## Maternal PKU and Fetal Damage: Mechanism ### Clinical Context: Maternal PKU Syndrome **Key Point:** Even if the fetus is heterozygous (carrier) or homozygous normal for phenylalanine hydroxylase, it can suffer severe damage from maternal hyperphenylalaninemia. This is called **maternal PKU syndrome** or **fetal PKU syndrome**. ### Pathophysiology The primary mechanism of fetal damage is **competitive inhibition of neutral amino acid transporters** in the placenta: ```mermaid flowchart TD A["Maternal hyperphenylalaninemia<br/>Phe > 10 mg/dL"]:::urgent --> B["Excessive placental uptake<br/>of phenylalanine"]:::outcome B --> C{"Competition for neutral<br/>amino acid transporters<br/>LAT1, LAT2, y+LAT"}:::decision C -->|"Phenylalanine wins<br/>competition"|D["Reduced placental transfer of:<br/>• Tyrosine<br/>• Tryptophan<br/>• Leucine<br/>• Other large neutral AAs"]:::urgent D --> E["Fetal tyrosine deficiency"]:::urgent E --> F["↓ Catecholamine synthesis<br/>↓ Melanin synthesis<br/>↓ Protein synthesis"]:::outcome F --> G["Microcephaly<br/>Intellectual disability<br/>Congenital heart defects<br/>Growth restriction"]:::urgent ``` ### Why Tyrosine Deficiency Matters in Fetal Development **High-Yield:** Tyrosine is **conditionally essential** during fetal development. Although normally synthesized from phenylalanine, the fetus cannot produce enough tyrosine when: 1. Maternal phenylalanine is elevated (competitive inhibition of placental transport) 2. The fetal liver has immature phenylalanine hydroxylase activity Tyrosine is critical for: - **Catecholamine synthesis** (noradrenaline, adrenaline, dopamine) — essential for fetal cardiac development and CNS maturation - **Melanin synthesis** — explains hypopigmentation in maternal PKU offspring - **Thyroid hormone synthesis** (T₃, T₄) — crucial for CNS myelination and growth - **Protein synthesis** — needed for normal fetal growth ### Fetal Outcomes in Uncontrolled Maternal PKU | Outcome | Incidence | Mechanism | |---------|-----------|----------| | Intellectual disability | 90% | Tyrosine deficiency + direct phenylalanine toxicity | | Microcephaly | 75% | Impaired CNS growth and myelination | | Congenital heart defects | 15–30% | Impaired catecholamine-dependent cardiac development | | Growth restriction | 40% | Reduced placental amino acid transfer | | Hypopigmentation | 70% | Reduced melanin synthesis | | Neonatal hypocalcaemia | Common | Impaired parathyroid development | **Clinical Pearl:** The fetus is **not protected** by the maternal blood–brain barrier. Phenylalanine crosses the placenta freely via amino acid transporters, and fetal plasma phenylalanine is typically **higher** than maternal levels (2–3× higher) due to placental accumulation and fetal inability to metabolize it. ### Management: Strict Maternal Dietary Control **Key Point:** Maternal PKU women should maintain plasma phenylalanine **<6 mg/dL** (ideally <4 mg/dL) **before conception and throughout pregnancy**. 1. **Preconception counselling** — optimize phenylalanine levels before pregnancy 2. **Phenylalanine-restricted diet** — low-protein foods, special medical foods 3. **Supplementation** — tyrosine (conditionally essential), vitamins, minerals 4. **Frequent monitoring** — plasma phenylalanine levels every 1–2 weeks during pregnancy 5. **Multidisciplinary care** — metabolic specialist, obstetrician, dietitian **Warning:** Even if the fetus inherits normal or heterozygous genotype for phenylalanine hydroxylase, it cannot escape maternal hyperphenylalaninemia. Genetic testing of the fetus does NOT predict fetal outcome; only maternal phenylalanine control matters. 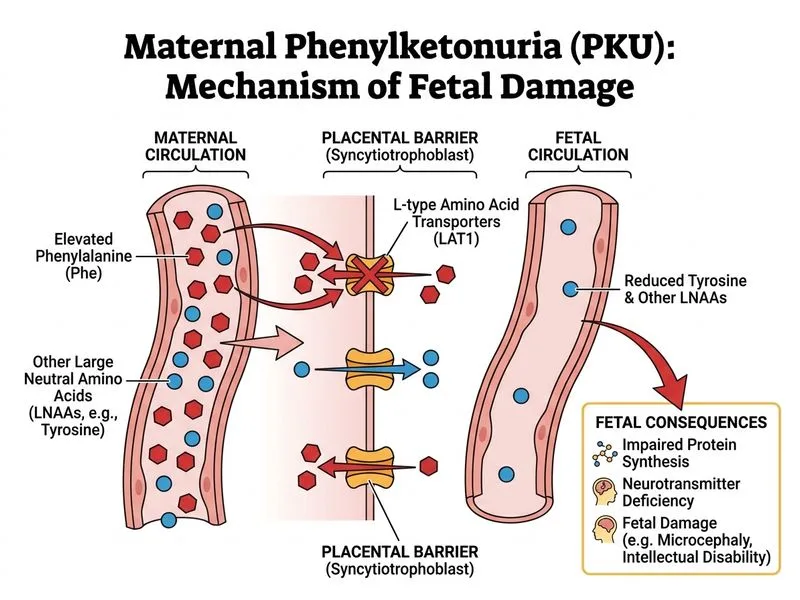
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.