## Acute Primary Angle-Closure Glaucoma: Emergency Management ### Clinical Presentation Recognition **Key Point:** The constellation of severe eye pain, corneal edema, mid-dilated non-reactive pupil, and markedly elevated IOP (58 mmHg) with narrow angles on the fellow eye is pathognomonic for acute angle-closure glaucoma (AACG). ### Immediate Medical Management (Before Definitive Laser) **High-Yield:** Acute AACG is an ophthalmologic emergency requiring rapid IOP lowering to prevent irreversible optic nerve damage. Medical therapy aims to shrink the vitreous volume and deepen the anterior chamber before laser peripheral iridotomy. **Clinical Pearl:** The order of medical intervention matters: 1. **Topical pilocarpine 4%** every 15 minutes (up to 6 doses) — causes pupillary miosis, pulling the iris away from the angle and deepening the chamber 2. **IV acetazolamide 500 mg** — reduces aqueous humor production by 50% 3. **Topical beta-blocker (timolol 0.5%)** — further reduces aqueous production 4. **Topical corticosteroid (dexamethasone)** — reduces inflammation and corneal edema, improving visualization for gonioscopy **Warning:** Do NOT give pilocarpine if corneal edema is severe (as here) — it will worsen the edema initially. However, once IOP begins to fall with other agents, pilocarpine becomes effective. Modern practice often uses pilocarpine cautiously or omits it if prostaglandin analogs are available. ### Why Medical First? **Key Point:** Medical therapy is the bridge to definitive laser treatment. Once IOP is controlled and corneal clarity improves (usually within 30–60 minutes), laser peripheral iridotomy can be performed safely. Attempting laser with corneal edema and very high IOP risks failure. ### Definitive Treatment After medical stabilization, **laser peripheral iridotomy** is the definitive treatment for the acute eye and prophylaxis for the fellow eye (which has narrow angles and is at risk for AACG). ### Mechanism of Angle Closure ```mermaid flowchart TD A[Narrow anterior chamber angle]:::outcome --> B[Pupillary block: iris apposed to lens]:::outcome B --> C[Aqueous flow obstruction]:::outcome C --> D[Rapid IOP rise]:::urgent D --> E[Iris pushed forward into angle]:::urgent E --> F[Complete angle closure]:::urgent F --> G[Corneal edema, mid-dilated pupil, severe pain]:::outcome G --> H{Medical control achieved?}:::decision H -->|Yes| I[Laser peripheral iridotomy]:::action H -->|No| J[Anterior chamber paracentesis]:::action I --> K[Angle reopens, IOP normalizes]:::outcome ``` ### Table: Medical vs. Surgical Timing | Intervention | Timing | Goal | | --- | --- | --- | | Medical therapy (pilocarpine, acetazolamide, beta-blocker, steroid) | Immediate (0–60 min) | Lower IOP, improve corneal clarity, deepen chamber | | Laser peripheral iridotomy | After medical control | Eliminate pupillary block, prevent recurrence | | Anterior chamber paracentesis | If IOP remains >40 mmHg after 1 hour of medical therapy | Emergency IOP reduction when laser cannot be performed | [cite:Khurana 6e Ch 10] 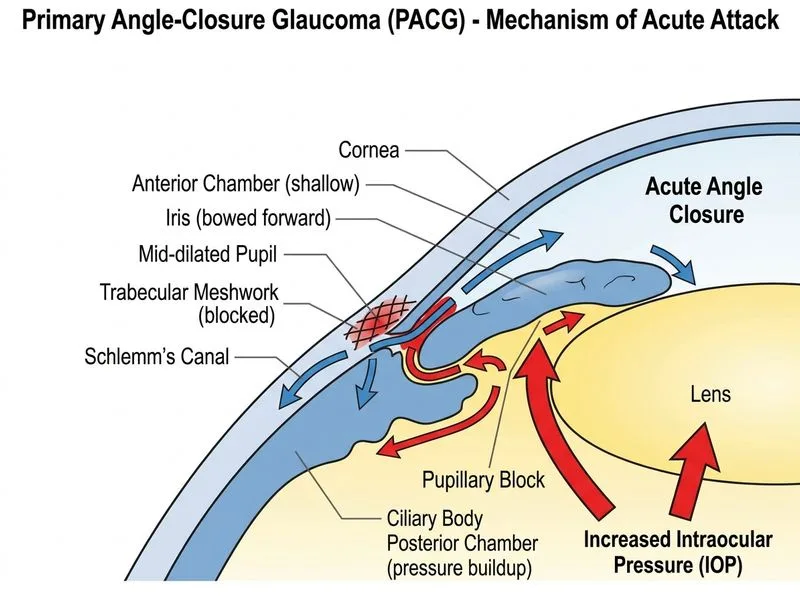
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.