## Acute Angle-Closure Glaucoma: Immediate Management ### Clinical Presentation Recognition **Key Point:** The triad of severe eye pain, blurred vision with halos, and mid-dilated fixed pupil in the setting of elevated IOP (>60 mmHg) and occludable angles is pathognomonic for acute angle-closure glaucoma. ### Immediate Medical Management Protocol **High-Yield:** Acute angle-closure requires **sequential medical therapy BEFORE definitive laser treatment** to lower IOP sufficiently to allow corneal clarity and safe gonioscopy. 1. **Topical agents** (onset: minutes to hours) - Pilocarpine 4% — causes pupillary constriction, pulling iris away from angle - Beta-blockers and prostaglandin analogs — reduce aqueous production 2. **Systemic agents** (onset: 30–60 minutes) - IV acetazolamide 500 mg — carbonic anhydrase inhibitor, reduces aqueous by ~50% - IV mannitol 20% — osmotic agent, shrinks vitreous volume - Oral glycerol — alternative osmotic agent 3. **Definitive treatment** (after IOP control) - YAG laser peripheral iridotomy — creates alternate aqueous drainage pathway - Performed once cornea clears (IOP typically <40–50 mmHg) ### Why This Sequence? ```mermaid flowchart TD A[Acute angle-closure diagnosed]:::outcome --> B[IOP > 60 mmHg + corneal edema]:::outcome B --> C[Medical therapy: topical + IV agents]:::action C --> D{IOP controlled + cornea clear?}:::decision D -->|Yes| E[YAG laser peripheral iridotomy]:::action D -->|No| F[Repeat IV mannitol/acetazolamide]:::action F --> D E --> G[Prophylactic iridotomy contralateral eye]:::action G --> H[Prevent recurrence]:::outcome ``` **Clinical Pearl:** Attempting YAG laser when cornea is severely edematous will fail — the laser beam cannot penetrate. Medical therapy must precede laser. ### Why Option 1 Alone Is Insufficient Direct laser without IOP reduction risks: - Inability to visualize angle through edematous cornea - Lens-cornea contact during procedure - Posterior synechiae formation ### Contraindication to Pilocarpine Monotherapy Pilocarpine alone is **insufficient** in acute angle-closure because: - Extremely elevated IOP (>60 mmHg) causes iris ischemia and paralysis - Pupil becomes unresponsive to miotics - Requires IOP reduction to <50 mmHg first via systemic agents **Mnemonic: PACE** — **P**ilocarpine (topical), **A**cetazolamide (IV), **C**orneal clarity (goal), **E**ventually iridotomy [cite:Khurana Ophthalmology Ch 8] 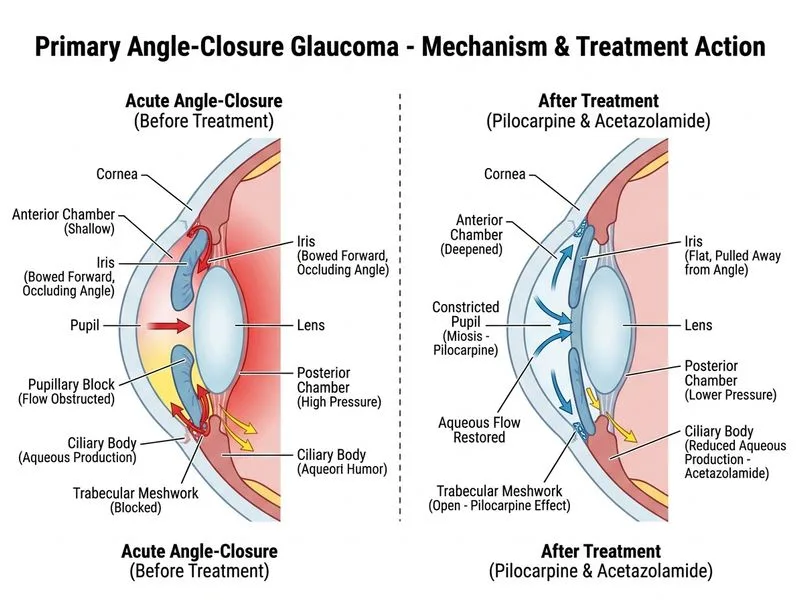
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.