## Acute Primary Angle-Closure Glaucoma: Emergency Management ### Clinical Presentation Recognition **Key Point:** The constellation of sudden severe eye pain, blurred vision, halos, corneal edema, mid-dilated fixed pupil, and markedly elevated IOP (>50 mmHg) is pathognomonic for acute angle-closure glaucoma. ### Immediate Management Algorithm ```mermaid flowchart TD A[Acute angle-closure glaucoma diagnosed]:::outcome --> B[Reduce IOP medically FIRST]:::action B --> C[Topical agents: pilocarpine, beta-blockers, CAIs]:::action B --> D[Systemic: IV acetazolamide, oral osmotic agents]:::action C --> E{IOP controlled?}:::decision D --> E E -->|Yes| F[Perform YAG laser peripheral iridotomy]:::action E -->|No| G[Consider anterior chamber paracentesis]:::urgent F --> H[Treat fellow eye prophylactically]:::action H --> I[YAG iridotomy on contralateral eye]:::action ``` ### Rationale for Two-Stage Approach **High-Yield:** Medical therapy MUST precede laser in acute angle-closure because: 1. Corneal edema from severe IOP elevation obscures the angle and makes laser difficult 2. Pilocarpine causes pupillary constriction, pulling the iris away from the angle and opening it mechanically 3. IOP reduction improves corneal clarity for better laser visualization 4. Reduces risk of posterior synechiae formation during the acute phase ### Medical Phase (Immediate) | Agent | Mechanism | Dosing | |-------|-----------|--------| | Pilocarpine 1% | Pupillary constriction; angle opening | 1 drop Q15min × 1 hour, then Q6h | | Timolol 0.5% | Aqueous suppression | 1 drop BD | | Dorzolamide/Brinzolamide | CAI (topical) | 1 drop TID | | IV Acetazolamide | CAI (systemic); osmotic effect | 500 mg IV/IM | | Oral Mannitol or Glycerol | Osmotic dehydration of vitreous | 1–1.5 g/kg PO | **Clinical Pearl:** Avoid mydriatics (atropine, cyclopentolate) — they worsen angle-closure by pushing the iris forward. ### Laser Phase (After IOP Control) **Key Point:** YAG laser peripheral iridotomy is definitive treatment once IOP is reduced and corneal clarity improves (typically within 1–2 hours of medical therapy). - **Right eye:** Treat the affected eye - **Left eye:** Prophylactic iridotomy on the fellow eye with narrow angle (prevents acute attack in ~50% of untreated narrow-angle eyes within 5 years) ### Why NOT the Other Options 1. **Iridotomy on right eye only (Option 0):** Omits prophylactic treatment of the high-risk fellow eye; leaves it vulnerable to acute attack. 2. **Anterior chamber paracentesis (Option 2):** Reserved for cases where medical therapy fails or corneal edema is so severe that laser cannot be performed; not first-line. 3. **Trabeculectomy (Option 3):** Surgical filtration is NOT the first-line definitive treatment; YAG iridotomy is. Trabeculectomy is reserved for angle-closure refractory to iridotomy or chronic angle-closure with residual elevated IOP. [cite:Khurana 6e Ch 12] 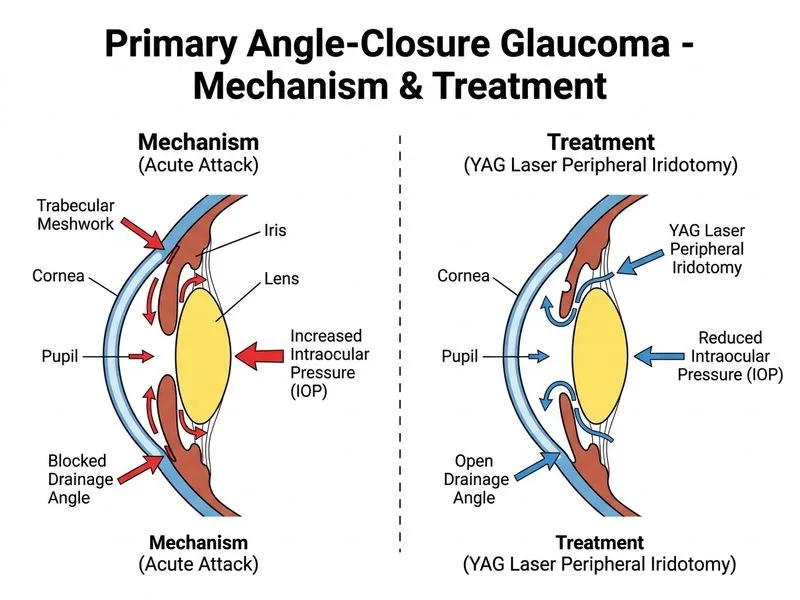
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.