## Biochemical Basis of Recurrent Gout **Key Point:** Gout results from monosodium urate crystal deposition in joints, triggered by hyperuricemia (serum uric acid >6.8 mg/dL). The PRIMARY cause in approximately **85–90% of gout patients** is **decreased renal clearance (underexcretion)** of uric acid — not overproduction. ### Purine Metabolism and Uric Acid Handling ``` Dietary Purines + De Novo Synthesis ↓ Hypoxanthine / Xanthine ↓ [Xanthine Oxidase] Uric Acid ↓ Renal Excretion ← PRIMARY CONTROL POINT ``` ### Causes of Hyperuricemia | Mechanism | Frequency | Examples | |-----------|-----------|----------| | **Underexcretion** | **85–90%** | Reduced tubular secretion, CKD, diuretics, alcohol, genetic polymorphisms in URAT1/OAT transporters | | **Overproduction** | 10–15% | HGPRT deficiency (Lesch-Nyhan), PRPP synthetase overactivity, malignancy, hemolysis, high purine diet | ### Why Option A is Correct This patient has **classic primary gout** — middle-aged male, recurrent attacks, elevated serum uric acid, negatively birefringent needle-shaped crystals (monosodium urate). The stem provides **no clues** suggesting an overproduction etiology (no malignancy, no hemolysis, no mention of high purine diet, no neurological features suggesting Lesch-Nyhan syndrome). By epidemiology and biochemistry, the PRIMARY cause of his recurrent hyperuricemia and gout attacks is **reduced renal clearance of uric acid** — the kidneys fail to excrete sufficient uric acid, leading to accumulation, crystal deposition, and recurrent inflammatory attacks. **High-Yield:** Reduced renal clearance is mediated by impaired tubular secretion of urate (via URAT1 transporter), not necessarily reduced GFR. This is the dominant mechanism in idiopathic/primary gout. ### Why the Other Options Are Incorrect - **Option B (HGPRT deficiency):** Causes Lesch-Nyhan syndrome (severe neurological features, self-mutilation) — not present here. Partial deficiency causes gout but is rare. - **Option C (Xanthine oxidase overactivity):** An overproduction mechanism accounting for only ~10–15% of cases. No clinical clues in this stem support this etiology. While allopurinol targets xanthine oxidase, this does not mean overactivity is the primary cause — it is used because blocking the final step reduces uric acid regardless of etiology. - **Option D (PRPP synthetase overactivity):** A rare X-linked overproduction cause; no supporting features in the stem. **Clinical Pearl:** Uricosuric agents (probenecid) and URAT1 inhibitors (lesinurad) are effective in gout precisely because underexcretion is the dominant mechanism. Allopurinol/febuxostat work downstream and are effective regardless of mechanism. **Mnemonic:** **90% of Gout = Renal Underexcretion** — "Kidneys Can't Clear Urate." [cite: Harrison's Principles of Internal Medicine, 21st ed., Chapter on Gout and Hyperuricemia; Lehninger Principles of Biochemistry, Ch 22] 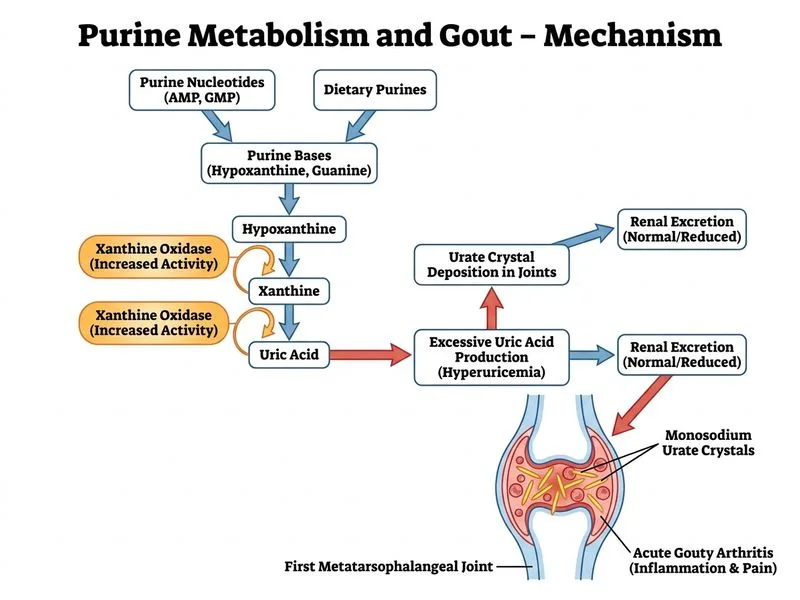
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.