## Clinical Presentation This patient has a **small, localized renal cell carcinoma (T1a, <4 cm)** with: - Tumor size 3.5 cm (well below 4 cm threshold) - No evidence of metastatic disease (M0) - Good performance status and normal renal function - No contraindications to nephron-sparing surgery ## Nephron-Sparing Surgery: The Standard of Care for T1a RCC **Key Point:** Partial nephrectomy (nephron-sparing surgery) is the gold standard for T1a tumors (<4 cm) in patients with normal contralateral kidney function [cite:Robbins 10e Ch 20]. **High-Yield:** Partial nephrectomy achieves equivalent oncologic outcomes to radical nephrectomy while preserving renal parenchyma and reducing long-term cardiovascular and renal morbidity. ## Comparison of Management Options for T1a RCC | Modality | Indication | Outcome | Limitation | |----------|-----------|---------|------------| | **Partial nephrectomy** | T1a, fit patient, normal contralateral kidney | Gold standard; equivalent OS/DFS to radical nephrectomy | Requires surgical expertise | | Active surveillance | Elderly, unfit, or patient preference | Acceptable for very small (<2 cm) or slow-growing tumors | Risk of progression; requires close imaging | | Ablation (RFA/cryo) | T1a, unfit for surgery, or solitary kidney | Local control ~90–95% | Higher recurrence than surgery; limited for tumors >4 cm | | Adjuvant TKI | High-risk resected RCC (T3–T4, N+) | Modest DFS benefit in selected cases | Not standard for T1a; no OS benefit demonstrated | ## Why Partial Nephrectomy Is Correct 1. **Tumor size** — At 3.5 cm, this is ideal for nephron-sparing approach. 2. **Oncologic equivalence** — Partial nephrectomy achieves the same cancer-free survival as radical nephrectomy for T1a tumors. 3. **Functional benefit** — Preserves renal mass, reducing long-term CKD risk and cardiovascular events. 4. **Fit patient** — No contraindications to open or robot-assisted partial nephrectomy. **Clinical Pearl:** Modern series show that partial nephrectomy can be performed open, laparoscopic, or robot-assisted with low morbidity and excellent oncologic outcomes for T1a tumors. ## Why Other Options Are Incorrect 1. **Active surveillance** — Acceptable only for very small tumors (<2 cm) or in elderly/unfit patients who decline intervention. A 3.5 cm tumor in a fit patient warrants definitive treatment. Surveillance risks progression and metastasis. 2. **Radiofrequency ablation** — While acceptable for T1a tumors in unfit patients, it is not first-line in a fit patient. Ablation has higher local recurrence rates (~5–10%) compared to surgery (~1–2%) and is less suitable for tumors approaching 4 cm. 3. **Adjuvant sunitinib** — Not indicated for T1a disease. Adjuvant TKI is reserved for high-risk resected RCC (T3–T4, N+, or grade 4) and has not shown OS benefit in T1a patients. Giving systemic therapy to a patient with completely resected low-risk disease increases toxicity without proven benefit. 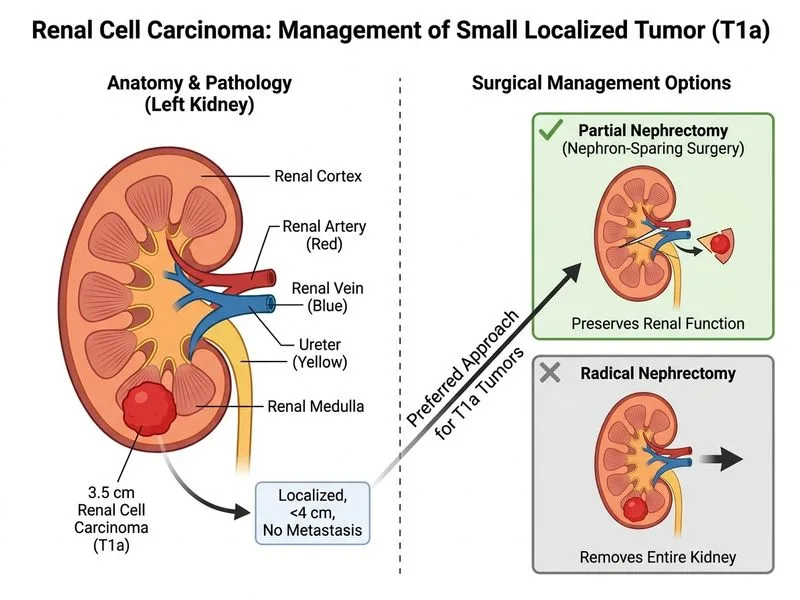
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.