## Management of Small Localized Renal Cell Carcinoma ### Clinical Context **Key Point:** This is a **Stage I RCC** (T1a, <4 cm, confined to kidney, no metastases). The mass shows typical imaging features of RCC: arterial phase enhancement with delayed washout ("enhancement kinetics" characteristic of hypervascular renal tumors). ### Treatment Algorithm for Localized RCC ```mermaid flowchart TD A[Localized RCC]:::outcome --> B{Tumor size?}:::decision B -->|>7 cm or T2-T4| C[Radical nephrectomy]:::action B -->|4-7 cm| D{Renal function normal?}:::decision B -->|<4 cm| E{Renal function normal?}:::decision D -->|Yes| F[Partial nephrectomy preferred]:::action D -->|No| G[Radical nephrectomy]:::action E -->|Yes| H[Partial nephrectomy preferred]:::action E -->|No| I[Active surveillance or ablation]:::action H --> J[Nephron-sparing approach]:::outcome F --> J ``` ### Why Partial Nephrectomy is Preferred **High-Yield:** Current guidelines (EAU, NCCN, ASCO) recommend **nephron-sparing surgery (NSS)** for: - Tumors <4 cm (T1a) with normal renal function - Solitary kidney or bilateral disease - Chronic kidney disease or diabetes - Young patients (<60 years) with normal contralateral kidney **Clinical Pearl:** Partial nephrectomy offers equivalent oncological outcomes to radical nephrectomy for T1a tumors while preserving renal parenchyma. Studies show: - **5-year cancer-specific survival:** ~95% for T1a tumors (equivalent with either approach) - **Renal function preservation:** Partial nephrectomy preserves ~80–90% of renal function vs. ~50% with radical nephrectomy - **Cardiovascular outcomes:** Preserved renal function reduces long-term cardiovascular morbidity and mortality ### Comparison of Management Options | Approach | Indication | Pros | Cons | |----------|-----------|------|------| | **Partial nephrectomy** | T1a, normal renal function, young patient | Preserves renal function, equivalent oncology | Technically demanding, longer operative time | | **Radical nephrectomy** | T1b–T4, advanced disease, poor renal function | Simpler, complete tumor removal | Permanent renal function loss, cardiovascular risk | | **Active surveillance** | Very elderly, comorbidities, <2 cm | Non-invasive, avoids surgery | Risk of progression, delayed treatment | | **Ablation (RFA/cryoablation)** | Elderly, solitary kidney, poor surgical candidate | Minimally invasive, outpatient | Incomplete ablation (5–10%), local recurrence | **Warning:** Active surveillance is NOT appropriate for a fit 62-year-old with normal renal function and a 3.5 cm mass. This patient is a good surgical candidate and should undergo definitive treatment. ### Surgical Approach **Key Point:** Partial nephrectomy can be performed via: 1. **Open partial nephrectomy** — gold standard, best outcomes 2. **Laparoscopic partial nephrectomy** — reduced morbidity, equivalent oncology 3. **Robot-assisted partial nephrectomy** — improved precision, shorter warm ischemia time ### Oncological Outcomes **Mnemonic for T1 RCC outcomes:** **"PARTIAL = Preserved Renal function And Retained Tumor-free Interval, Ideal for Localized disease."** - **Local recurrence:** <2% with partial nephrectomy - **Metastatic recurrence:** ~5–10% at 5 years for T1a - **Cancer-specific survival:** ~95% at 5 years [cite:Harrison 21e Ch 297; EAU Guidelines on RCC 2023] 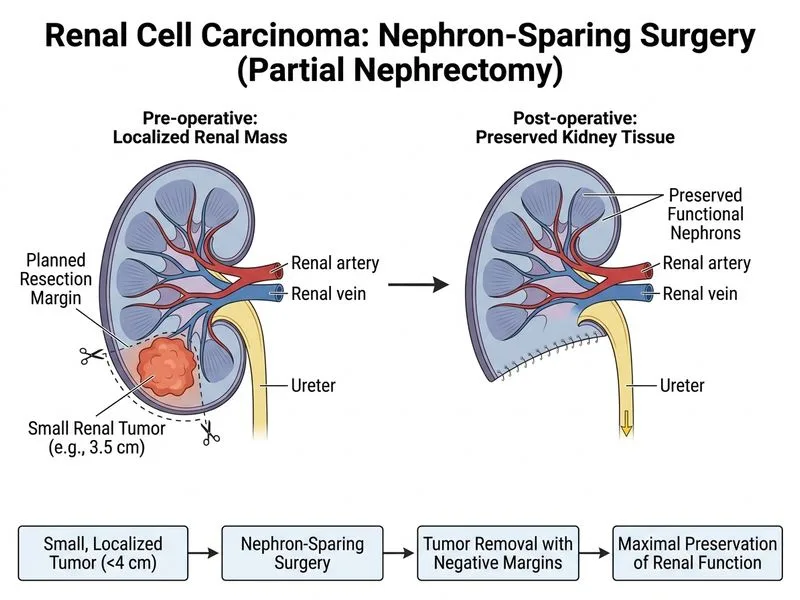
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.