## Clinical Assessment This patient has a **rhegmatogenous retinal detachment (RRD)** with a clear retinal break and vitreous hemorrhage. The superior temporal location and high myopia (−8.0 D) with lattice degeneration are classic risk factors. ### Key Diagnostic Features **Key Point:** The presence of a retinal break (identified on fundoscopy), vitreous hemorrhage, and the characteristic presentation of floaters + photopsia confirm acute RRD. **High-Yield:** Although the macula is currently **uninvolved (macula-on)**, this is a **macula-off risk** — the superior temporal detachment can progress rapidly to involve the macula within hours to days. Preserving macula-on status is the primary urgency driver; once the macula detaches, visual prognosis worsens significantly even after successful reattachment. ### Management Principles **Clinical Pearl:** In RRD with vitreous hemorrhage obscuring the inferior retina, **urgent vitreoretinal consultation is mandatory** — the surgeon must decide between: - **Primary vitrectomy** if vitreous hemorrhage is dense or if inferior breaks are suspected - **Pneumatic retinopexy** if the break is superior and isolated - **Scleral buckle** if breaks are localized and vitreous is clear **Key Point:** Bed rest with **head positioning** (positioning the break in a dependent position to allow gravity to tamponade the break) is a critical temporizing measure while awaiting surgical consultation. This can prevent macula involvement and buy time for preoperative assessment. ### Why Option D is Correct Urgent referral with **head positioning** (break in dependent position) and **vitreoretinal consultation** is the standard of care. This allows: 1. Rapid surgeon evaluation 2. Preoperative imaging (B-scan ultrasound if vitreous hemorrhage obscures the view) 3. Temporizing positioning to prevent macula involvement 4. Definitive surgical planning (vitrectomy vs. buckle vs. pneumatic retinopexy) ### Why Other Options Are Incorrect - **Option A (Primary PPV immediately):** While PPV may ultimately be the chosen surgery, the immediate step is urgent consultation — the vitreoretinal surgeon decides the surgical approach after full evaluation. Selecting PPV without consultation bypasses the decision-making process. - **Option B (Laser photocoagulation):** Laser alone cannot reattach the retina — it only demarcates the detachment. It is NOT definitive treatment for RRD with an active break and is contraindicated as sole management here. - **Option C (Observation):** Inappropriate because the detachment is progressive (superior temporal location with clear break), vitreous hemorrhage obscures the inferior retina (inferior breaks may be present), and macula-off conversion is imminent. [cite: Khurana Ophthalmology, 6th Ed., Ch. 11; American Academy of Ophthalmology Preferred Practice Pattern — Posterior Vitreous Detachment, Retinal Breaks, and Lattice Degeneration] 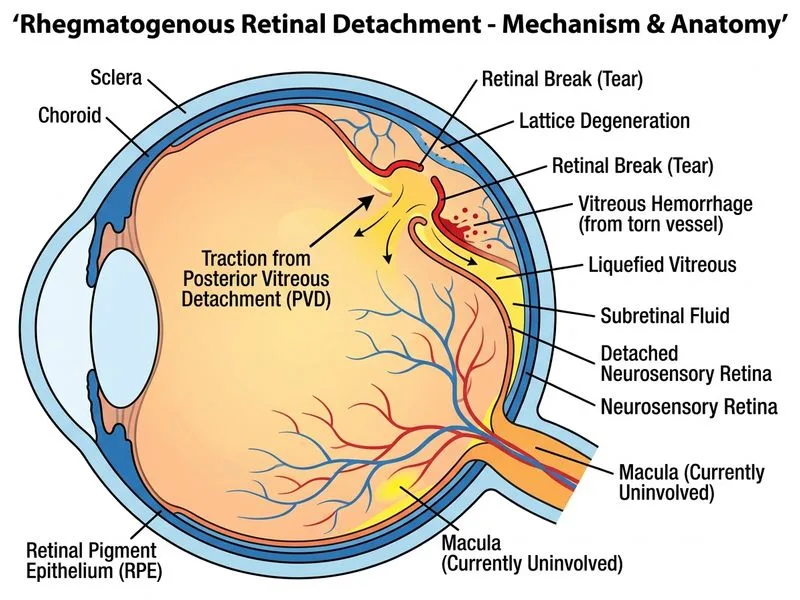
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.