## Clinical Presentation & Key Diagnostic Features This patient has **tractional retinal detachment (TRD)** secondary to PDR: ### Distinguishing Features of TRD | Feature | Tractional RD | Rhegmatogenous RD | Exudative RD | |---------|---------------|-------------------|---------------| | **Retinal breaks** | Absent | Present (essential) | Absent | | **Subretinal fluid** | Localized, under traction | Diffuse, spreads by gravity | Localized | | **Retinal elevation** | Smooth, immobile, funnel-shaped | Convex, mobile | Smooth, shallow | | **B-scan appearance** | Smooth, dome-shaped, no echoes | Variable echoes (PVD, hemorrhage) | Smooth, no internal echoes | | **Symptoms** | Gradual vision loss, no photopsia | Acute floaters, photopsia | Gradual, painless | | **Associated disease** | PDR, ROP, trauma, advanced RVO | Myopia, aphakia, trauma | Diabetes, hypertension, inflammation | | **Macula involvement** | Often spared initially | May be on or off | Often spared | **Key Point:** The **absence of retinal breaks** is the critical diagnostic feature that rules out rhegmatogenous RD. Traction from fibrovascular membranes mechanically pulls the retina inward. ### Why This Is TRD, Not RRD 1. **No retinal breaks** on dilated fundoscopy (RRD requires breaks) 2. **Smooth, dome-shaped elevation** on B-scan (characteristic of traction) 3. **Gradual onset** without photopsia or acute floaters (RRD typically presents acutely) 4. **PDR history** (fibrovascular proliferation causes traction) 5. **Inferior nasal location** (typical for PDR-related TRD; gravity-dependent spread is seen in RRD, not TRD) **Clinical Pearl:** In PDR, fibrovascular membranes contract over time, creating **tangential traction** that pulls the retina inward. Unlike RRD (which spreads by gravity), TRD elevation is localized and immobile. ## Management Implications ```mermaid flowchart TD A[Retinal Detachment]:::outcome --> B{Retinal breaks present?}:::decision B -->|Yes| C[Rhegmatogenous RD]:::outcome B -->|No| D{Vitreous traction evident?}:::decision D -->|Yes| E[Tractional RD]:::outcome D -->|No| F{Subretinal exudate/fluid?}:::decision F -->|Yes| G[Exudative RD]:::outcome C --> H[Urgent vitrectomy ± buckle]:::action E --> I[Vitrectomy if macula threatened]:::action G --> J[Treat underlying cause]:::action I --> K[Reattachment via membrane removal]:::outcome J --> K ``` **High-Yield:** **TRD management is conservative** unless the macula is threatened or detaching. Unlike RRD (which requires urgent surgery), TRD may be observed if the macula is attached and stable. Surgery (vitrectomy with membrane peeling) is reserved for progressive cases or macula-off TRD. ## Why Other Options Are Incorrect 1. **Rhegmatogenous RD with large break** (option 0): RRD requires visible retinal breaks. This patient has **no breaks** on examination. Additionally, RRD typically presents with acute floaters and photopsia, which are absent here. The smooth, dome-shaped B-scan appearance is inconsistent with RRD. 2. **Exudative RD due to diabetic macular edema** (option 2): While diabetes causes exudative RD, the clinical picture here is dominated by **mechanical traction**, not exudation. Exudative RD typically presents with shallow, localized elevation and gradual vision loss, but the B-scan appearance and the presence of fibrovascular traction in PDR strongly favor TRD. Also, diabetic macular edema does not typically cause large areas of subretinal fluid with retinal elevation in the inferior nasal quadrant. 3. **Hemorrhagic RD from neovascular glaucoma** (option 3): Neovascular glaucoma causes elevated intraocular pressure and iris neovascularization, not retinal detachment. While PDR can lead to neovascular glaucoma, the clinical presentation here (smooth retinal elevation, no breaks, traction evident) is classic for TRD, not hemorrhagic detachment or glaucoma. ## Clinical Pearls on PDR Complications **Mnemonic: PDR-TRD** — **P**roliferative **D**iabetic **R**etinopathy causes **T**ractional **R**etinal **D**etachment via fibrovascular membrane contraction. - **TRD is the most common cause of vision loss in PDR** (after vitreous hemorrhage) - **Fibrovascular membranes** originate at the optic disc and major vascular arcades - **Contraction over months to years** causes gradual, progressive detachment - **Macula-sparing TRD** can be observed; **macula-threatening or macula-off TRD** requires urgent vitrectomy 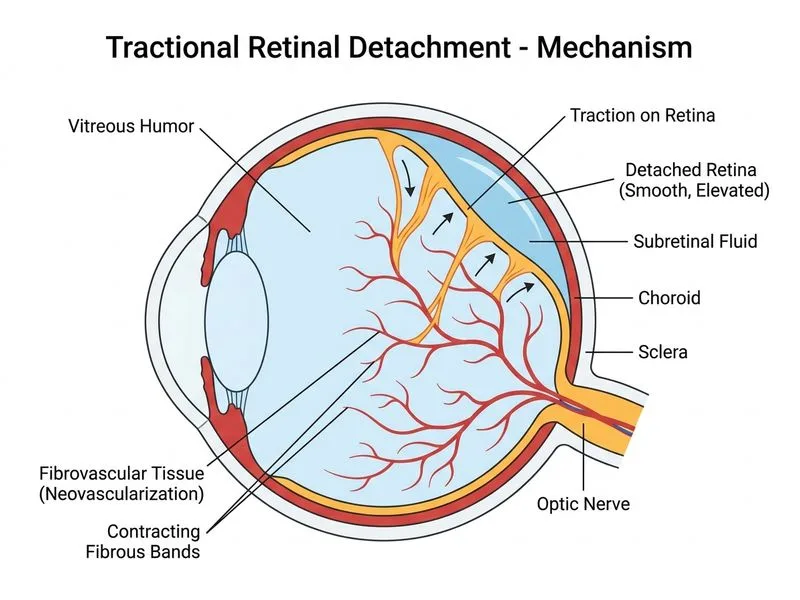
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.