## Clinical Diagnosis: Scrub Typhus ### Key Clinical Features Pointing to Scrub Typhus **Key Point:** The pathognomonic finding is the **eschar** (tache noire) — a painless, necrotic lesion with a black crust and surrounding erythema at the site of mite bite. **High-Yield:** Scrub typhus is endemic in the "tsutsugamushi triangle" (from northern Japan and far-eastern Russia in the north, to northern Australia in the south, and to Afghanistan and Pakistan in the west). Tamil Nadu falls within this endemic zone. ### Characteristic Triad of Scrub Typhus | Feature | Scrub Typhus | RMSF | Murine Typhus | |---------|--------------|------|---------------| | **Eschar (tache noire)** | Present (painless, black crust) | Absent | Absent | | **Rash onset** | Day 5–7 (trunk → extremities) | Day 2–4 (extremities → trunk) | Day 5–6 (sparse) | | **Lymphadenopathy** | Prominent, regional | Absent or mild | Absent | | **Vector** | Larval trombiculid mite | Hard tick (*Dermacentor*) | Rat flea | | **Mortality (untreated)** | 1–6% | 20–30% | < 2% | ### Pathophysiology 1. Larval trombiculid mite bite → *Orientia tsutsugamushi* inoculation 2. Local multiplication → eschar formation (Day 3–7) 3. Hematogenous spread → fever, rash, systemic inflammation 4. Vasculitis of small vessels → thrombocytopenia, transaminitis **Clinical Pearl:** The eschar may be missed if located in hidden areas (axilla, groin, scalp). Always examine the entire body, especially skin folds. ### Laboratory Findings in This Case - **Thrombocytopenia:** Due to vasculitis and bone marrow involvement - **Elevated transaminases:** Hepatic involvement (hepatitis pattern) - **Lymphocytosis:** Often present in peripheral blood ### Diagnostic Confirmation - **Weil-Felix test:** Heterophile agglutination (positive in scrub typhus, RMSF; negative in murine typhus) - **Immunofluorescence:** Gold standard; detects IgM and IgG antibodies - **PCR:** Most sensitive and specific **High-Yield:** Doxycycline 100 mg BD for 7 days is the drug of choice. Early treatment (within 5 days of fever onset) dramatically reduces mortality and prevents complications. ### Why This Is Scrub Typhus and Not the Others - **Eschar is pathognomonic** — RMSF and murine typhus do not present with eschar - **Prominent lymphadenopathy** — more typical of scrub typhus than RMSF - **Geographic context** — endemic in Tamil Nadu (part of tsutsugamushi triangle) - **Occupational exposure** — agricultural worker at risk of mite bite in scrub vegetation 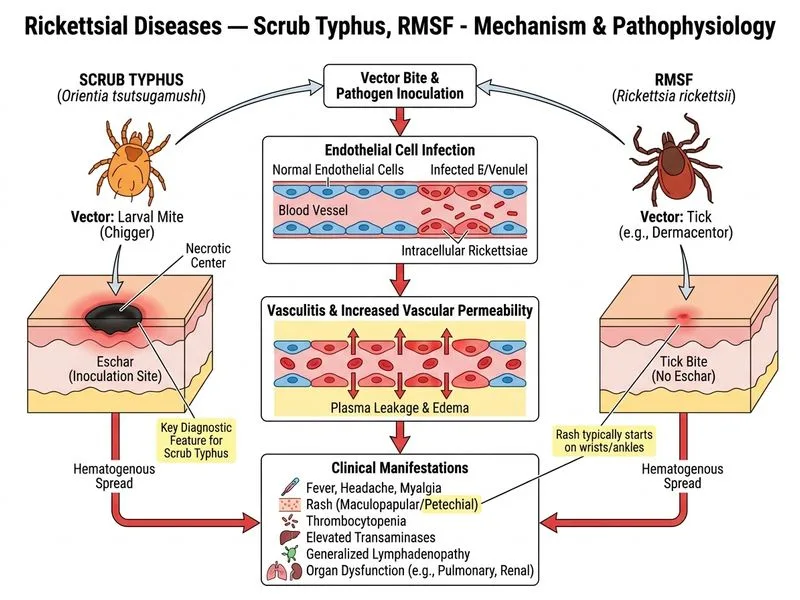
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.