## Clinical Diagnosis: Scrub Typhus ### Key Clinical Features Pointing to Scrub Typhus **Key Point:** The pathognomonic finding here is the **black eschar (tache noire)** at the site of mite bite, combined with fever, headache, myalgia, and rash in an endemic region. **High-Yield:** Scrub typhus is endemic in the **"Tsutsugamushi Triangle"** — a region spanning from northern Japan and far-eastern Russia in the north, to northern Australia in the south, and to Afghanistan and Pakistan in the west. India (especially the Western Ghats, Himalayas, and coastal regions) is a known endemic zone. ### Pathophysiology & Epidemiology 1. **Causative agent:** *Orientia tsutsugamushi* (formerly *Rickettsia tsutsugamushi*) — an obligate intracellular gram-negative coccobacillus 2. **Vector:** Larval trombiculid mites (chiggers) — found in scrubland, grassland, and forest fringes 3. **Transmission:** Mite bite during outdoor activities; no human-to-human transmission 4. **Incubation period:** 6–21 days (average 10–12 days) — consistent with this patient's timeline ### Clinical Presentation | Feature | Scrub Typhus | RMSF | Murine Typhus | |---------|--------------|------|----------------| | **Eschar** | Present (tache noire) at bite site | Absent | Absent | | **Rash onset** | Day 4–6 of fever | Day 2–4 of fever | Day 5–8 of fever | | **Rash distribution** | Trunk → limbs, spares palms/soles | Wrists/ankles → trunk (includes palms/soles) | Trunk, spares palms/soles | | **Lymphadenopathy** | Regional (draining) — prominent | Absent | Absent | | **Geographic risk** | Tsutsugamushi Triangle (Asia-Pacific) | North America (especially SE USA) | Worldwide (urban/periurban) | | **Vector** | Larval mites | Tick (*Dermacentor*) | Flea (*Xenopsylla*) | **Clinical Pearl:** The **eschar is the most specific sign** of scrub typhus — it appears as a painless, indurated, blackened papule with surrounding erythema and edema. It may be missed if located in inconspicuous areas (axilla, groin, scalp). ### Diagnosis - **Serology:** Weil-Felix test (non-specific, positive in rickettsial infections), IgM ELISA (specific, positive from day 5 onwards) - **PCR:** Real-time PCR on blood/eschar biopsy (gold standard, high sensitivity and specificity) - **Culture:** Difficult; requires BSL-3 facilities - **Blood cultures:** Negative (as in this case) — rickettsiae are intracellular ### Treatment **High-Yield:** Doxycycline is the **drug of choice** for all rickettsial infections in non-pregnant adults. - **First-line:** Doxycycline 100 mg BD for 7–14 days - **Alternative (pregnancy/allergy):** Chloramphenicol 500 mg QID for 7–14 days - **Pediatric:** Azithromycin 10 mg/kg/day (doxycycline avoided in children <8 years) **Warning:** Delayed or inadequate treatment increases risk of complications (ARDS, myocarditis, renal failure, DIC). ### Why Scrub Typhus (Not the Others)? The **eschar is pathognomonic** — it is present in 50–80% of scrub typhus cases but **absent in RMSF and murine typhus**. The combination of eschar + fever + rash + regional lymphadenopathy + Western Ghats exposure makes scrub typhus the definitive answer. 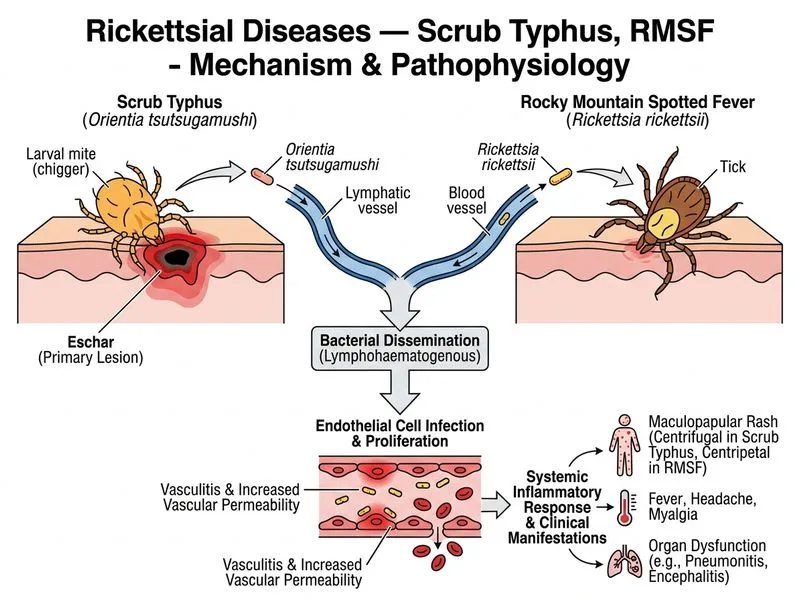
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.