## Clinical Presentation & Diagnosis **Key Point:** A scaphoid fracture is a clinical diagnosis in the setting of a FOOSH injury with anatomical snuffbox tenderness, even when initial plain radiographs are normal. Up to 25% of scaphoid fractures are radiographically occult on initial imaging. **High-Yield:** The gold standard for detecting occult scaphoid fractures is **repeat radiographs at 10–14 days**, when bone resorption at the fracture site becomes visible. This is the standard of care in most Indian orthopedic units and is cost-effective. ## Management Algorithm ```mermaid flowchart TD A[FOOSH injury + snuffbox tenderness]:::outcome --> B{Initial X-rays normal?}:::decision B -->|Yes| C[Treat as scaphoid fracture]:::action C --> D[Immobilize in thumb spica cast]:::action D --> E[Repeat X-rays at 10-14 days]:::action E --> F{Fracture visible?}:::decision F -->|Yes| G[Continue immobilization 8-12 weeks]:::action F -->|No| H[Discharge; no fracture]:::outcome B -->|No| I[Confirm fracture type & location]:::action ``` **Clinical Pearl:** Anatomical snuffbox tenderness (pain with thumb retropulsion test) and pain on axial thumb loading are highly sensitive clinical signs for scaphoid injury, regardless of radiographic findings. **Mnemonic:** **FOOSH** = Fall On OutStretched Hand — the classic mechanism for scaphoid fracture. ## Why Immobilization First? - Early immobilization prevents displacement and reduces nonunion risk - Thumb spica cast (or orthosis) is the standard for suspected undisplaced fractures - Repeat imaging at 10–14 days is the most cost-effective and practical approach in resource-limited settings - MRI and CT are reserved for: - Confirmation of complex/displaced fractures - Preoperative planning for surgical cases - Evaluation of complications (nonunion, avascular necrosis) [cite:Rockwood & Green's Fractures in Adults, Ch 8] 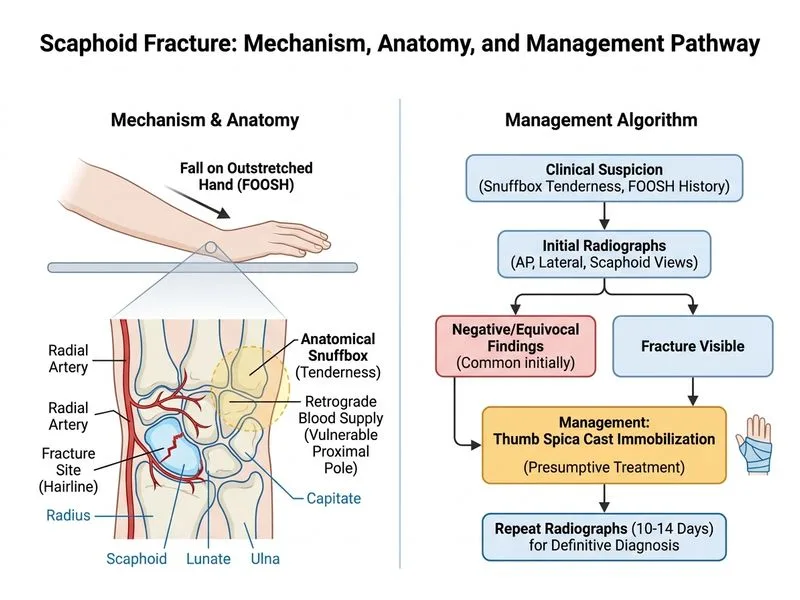
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.