## Scaphoid Fracture Complications **Key Point:** Avascular necrosis (AVN) is the most serious long-term complication of untreated or inadequately treated scaphoid fractures, particularly those involving the proximal pole. The proximal pole has a tenuous blood supply, making it vulnerable to ischemic necrosis. **High-Yield:** Scaphoid fractures at the **waist or proximal pole** carry the highest risk of AVN because the blood supply enters distally and retrograde flow to the proximal pole is compromised when the fracture disrupts vascular continuity. ## Vascular Anatomy & Risk Factors | Fracture Location | Blood Supply Pattern | AVN Risk | Healing Time | |---|---|---|---| | **Distal third** | Excellent (multiple entry points) | <1% | 6–8 weeks | | **Middle/waist** | Moderate (primarily distal entry) | 5–10% | 10–12 weeks | | **Proximal pole** | Poor (retrograde only) | 20–50% | 12–16 weeks | **Clinical Pearl:** The scaphoid is unique among carpal bones in having **retrograde blood supply** — the nutrient vessels enter at the distal pole and travel proximally. A fracture at the waist or proximal pole interrupts this flow, leaving the proximal fragment ischemic. ## Pathophysiology of AVN in Scaphoid Fractures ```mermaid flowchart TD A[Scaphoid waist/proximal fracture]:::outcome --> B[Disruption of retrograde blood supply]:::action B --> C[Proximal pole becomes ischemic]:::urgent C --> D{Fracture immobilized adequately?}:::decision D -->|No| E[Nonunion develops]:::urgent E --> F[Prolonged ischemia of proximal pole]:::urgent F --> G[Avascular necrosis]:::outcome D -->|Yes| H[Union occurs, AVN prevented]:::outcome ``` **Mnemonic:** **SCAPHOID AVN RISK** = **Waist and Proximal pole** fractures with **delayed/inadequate immobilization** and **nonunion**. ## Clinical Presentation of AVN - Persistent pain despite immobilization - Loss of grip strength - Clicking or clunking sensation in the wrist - Radiographic changes (sclerosis, fragmentation) appearing weeks to months after injury - Progressive wrist dysfunction ## Why This Patient Is at High Risk 1. **Fracture location:** Waist fracture — moderate-to-high AVN risk 2. **Delayed diagnosis:** Initial imaging was inconclusive; fracture may have been untreated for weeks 3. **Prolonged symptoms:** 3-month history suggests nonunion or delayed union 4. **Clinical signs:** Persistent snuffbox tenderness and scaphoid shift test positivity indicate ongoing instability ## Prevention & Management - **Early diagnosis and immobilization** are critical to prevent AVN - Thumb spica immobilization for 8–12 weeks (longer for proximal pole fractures) - Repeat imaging at 10–14 days and 6–8 weeks to confirm healing - Surgical fixation (percutaneous screw) for displaced fractures or nonunion - MRI or CT to detect early AVN changes (sclerosis, fragmentation) [cite:Rockwood & Green's Fractures in Adults, Ch 8; Campbell's Operative Orthopaedics, Ch 56] 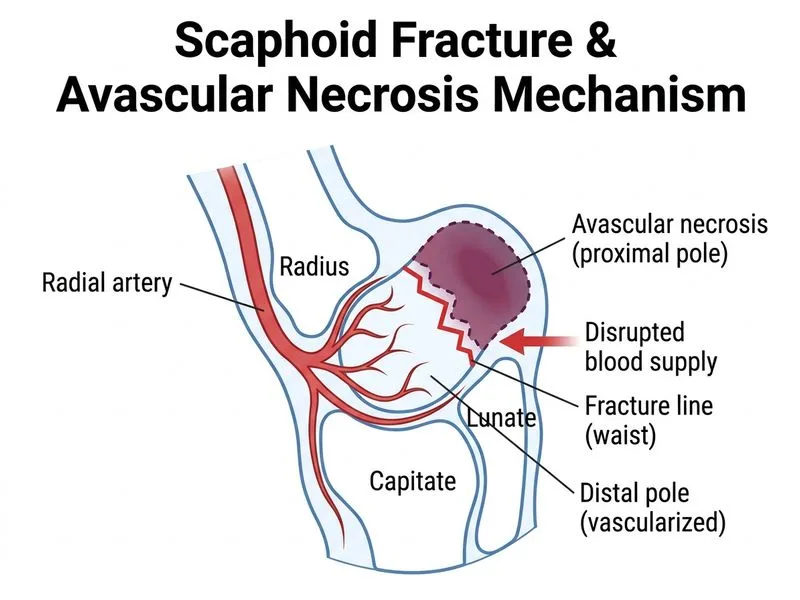
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.