## Complication Recognition & Management **Key Point:** A scaphoid waist fracture with a 2 mm gap and absence of callus at 8 weeks indicates **nonunion**. The waist is the most common site of nonunion (accounting for ~60% of scaphoid nonunions), and delayed diagnosis increases the risk significantly. ## Pathophysiology of Scaphoid Nonunion ```mermaid flowchart TD A[Scaphoid fracture]:::outcome --> B{Immediate immobilization?}:::decision B -->|Yes| C[Fracture healing: 12 weeks]:::action B -->|No| D[Delayed/missed diagnosis]:::urgent D --> E[Loss of fracture site vascularity]:::outcome E --> F[Fibrous tissue instead of bone callus]:::outcome F --> G[Nonunion develops]:::urgent C --> H{Union achieved?}:::decision H -->|Yes| I[Full recovery]:::outcome H -->|No| J[Nonunion: operative fixation needed]:::urgent G --> K[Operative fixation: screw or pin]:::action J --> K ``` **High-Yield:** Scaphoid nonunion is defined as **absence of radiographic union after 4–6 months** or **persistent fracture gap with no callus at 8+ weeks**. This patient meets criteria for nonunion. ## Risk Factors for Scaphoid Nonunion | Risk Factor | Impact | |-------------|--------| | **Delayed diagnosis** | Highest risk; fracture site loses vascularity | | **Proximal pole fracture** | Retrograde blood supply; ~10% nonunion rate | | **Waist fracture with displacement** | Intermediate risk; ~5–8% nonunion rate | | **Smoking** | Impairs bone healing | | **Poor immobilization compliance** | Fracture site micromotion prevents union | | **Fracture gap >2 mm** | Indicates displacement; higher nonunion risk | **Clinical Pearl:** The scaphoid has a **retrograde blood supply** (enters distally, flows proximally). Proximal pole fractures are at highest risk for AVN because the proximal fragment may lose its blood supply entirely. Waist fractures have intermediate risk; distal fractures have the best prognosis. ## Definitive Management of Nonunion **Key Point:** Operative fixation is the standard of care for scaphoid nonunion. Options include: 1. **Percutaneous screw fixation** (Herbert screw, cannulated screw) — **gold standard** - Allows early mobilization - High union rates (>90%) - Minimally invasive 2. **Open reduction + internal fixation with screw** - Indicated if percutaneous approach fails or anatomy unfavorable 3. **Percutaneous pinning** (K-wires) - Alternative if screw fixation not possible - Requires longer immobilization 4. **Bone graft + fixation** - Considered if nonunion is chronic (>1 year) or if there is bone loss - Particularly important for proximal pole nonunion (higher AVN risk) **Mnemonic — Scaphoid Nonunion Management: **SCREW** = Screw fixation (percutaneous preferred), Consider bone graft if chronic, Retrograde blood supply at risk (especially proximal), Early mobilization post-fixation, Wrist immobilization 6–12 weeks depending on fracture location. ## Why This Is Nonunion, Not AVN **Warning:** Do not confuse nonunion with avascular necrosis (AVN). | Feature | Nonunion | AVN | |---------|----------|-----| | **Definition** | Fracture fragments fail to unite; fibrous tissue at fracture site | Proximal fragment loses blood supply; bone necrosis | | **Radiographic finding** | Persistent fracture gap, no callus | Sclerosis, collapse of proximal pole (late) | | **Timeline** | Evident by 4–6 months | May take months to years to manifest | | **This patient** | 2 mm gap, no callus at 8 weeks = **nonunion** | No mention of sclerosis or collapse; AVN not yet evident | | **Management** | Operative fixation ± bone graft | Operative fixation ± proximal pole excision or fusion | **Clinical Pearl:** AVN of the scaphoid proximal pole is a **late complication** that may develop even after union occurs. It is not the primary diagnosis in this acute nonunion case. ## Why Other Options Are Incorrect - **Avascular necrosis (AVN):** While proximal pole AVN is a serious complication, it typically presents with sclerosis and collapse on imaging, which are not mentioned here. AVN is a late complication; nonunion is the acute problem. Arthroscopic debridement is not standard treatment for AVN. - **Malunion with dorsal angulation:** Malunion occurs when fracture fragments unite in an abnormal position. This patient has a **gap** with no callus, indicating nonunion (no union at all), not malunion (abnormal union). Corrective osteotomy is used for malunion, not nonunion. - **Post-traumatic arthritis + wrist fusion:** Arthritis and fusion are late sequelae of untreated scaphoid nonunion or AVN. The immediate management of active nonunion is operative fixation, not fusion. Fusion is reserved for cases with established arthritis or failed prior fixation. 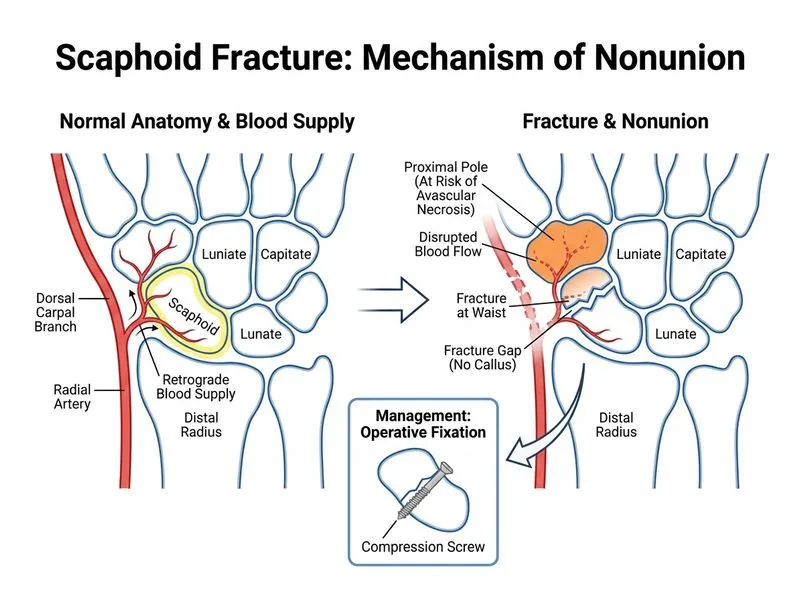
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.