## Clinical Presentation & Diagnosis **Key Point:** Scaphoid fractures are notoriously difficult to detect on initial plain radiographs, especially non-displaced or minimally displaced fractures. Clinical suspicion based on mechanism (FOOSH), anatomical snuffbox tenderness, and pain with axial thumb loading is sufficient to warrant empirical immobilization even when radiographs are negative. **High-Yield:** Approximately 15–20% of scaphoid fractures are radiographically occult on initial imaging. Delaying diagnosis and treatment increases the risk of complications such as nonunion, avascular necrosis (AVN), and chronic wrist dysfunction. ## Management Algorithm ```mermaid flowchart TD A[FOOSH injury + snuffbox tenderness]:::outcome --> B{Plain radiographs show fracture?}:::decision B -->|Yes| C[Confirm type & displacement]:::action B -->|No| D{High clinical suspicion?}:::decision D -->|Yes| E[Immobilize in thumb spica cast]:::action D -->|No| F[Discharge with analgesia]:::action E --> G[Repeat radiographs at 10-14 days]:::action G --> H{Fracture now visible?}:::decision H -->|Yes| I[Continue immobilization 8-12 weeks]:::action H -->|No| J[Consider MRI or CT if symptoms persist]:::action C --> K[Assess displacement & blood supply]:::action K --> L{Displaced or proximal pole?}:::decision L -->|Yes| M[Surgical fixation]:::urgent L -->|No| N[Cast immobilization]:::action ``` ## Why Immobilization First? 1. **Cost-effective:** Repeat radiographs at 10–14 days are significantly cheaper than immediate advanced imaging. 2. **Therapeutic benefit:** Immobilization in a thumb spica cast (below-elbow, including thumb IP joint) reduces pain and prevents further displacement. 3. **Healing promotion:** Early immobilization improves union rates even if the fracture is not yet radiographically visible. 4. **Standard of care:** This is the recommended approach in most orthopedic guidelines for suspected scaphoid fractures with negative initial radiographs [cite:Campbell's Orthopedic Surgery 13e Ch 57]. ## Imaging Progression | Timing | Modality | Indication | |--------|----------|------------| | **Initial (0 hrs)** | Plain radiographs (PA, lateral, scaphoid views) | First-line; ~80% sensitivity | | **10–14 days** | Repeat plain radiographs | Callus formation makes fracture visible | | **If still negative + persistent symptoms** | MRI or CT | High sensitivity; rules out other injuries | **Clinical Pearl:** The "scaphoid view" (PA with 20° ulnar deviation) improves fracture visualization by projecting the scaphoid free of overlying carpal bones. However, even with optimal technique, non-displaced fractures may not be apparent initially. ## Complications of Delayed Diagnosis **Warning:** Missing a scaphoid fracture and failing to immobilize leads to: - **Nonunion** (5–10% of scaphoid fractures) - **Avascular necrosis** (especially proximal pole fractures due to retrograde blood supply) - **Post-traumatic arthritis** (scapholunate dissociation, SLAC wrist) - **Chronic wrist pain and loss of grip strength** **Mnemonic:** **SCAN** — **S**nuffbox tenderness, **C**linical suspicion, **A**void missing it, **N**eed immobilization even if radiographs negative. 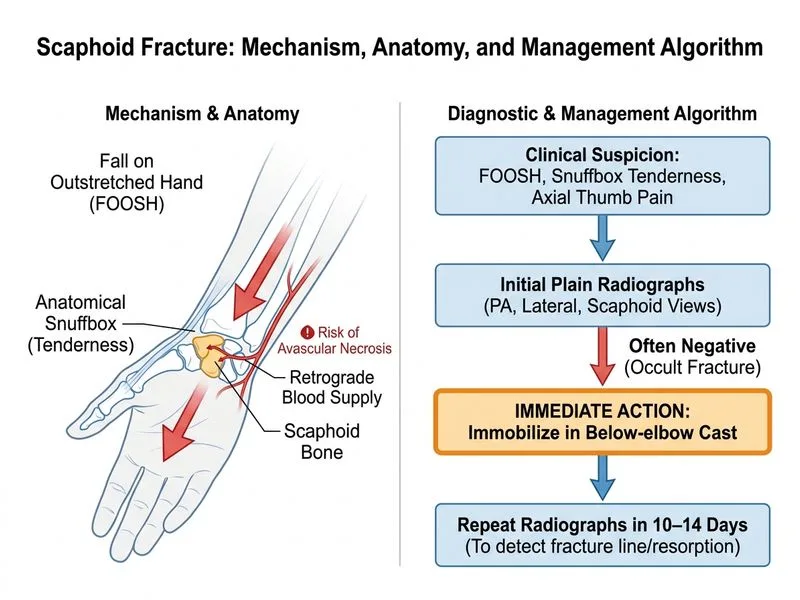
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.