## Scaphoid Fracture Complications **Key Point:** Proximal pole scaphoid fractures carry a high risk of nonunion and avascular necrosis (AVN) due to retrograde blood supply. The proximal pole receives blood supply only from distal-to-proximal vessels; fractures at this level interrupt the primary blood supply, predisposing to AVN in up to 50% of cases [cite:Rockwood & Green's Fractures in Adults 9e Ch 9]. **High-Yield:** Nonunion is defined as absence of bridging callus on radiographs after 12 weeks of immobilization. Proximal pole fractures are at highest risk (10–15% nonunion rate) compared to middle third (5%) or distal pole (<1%). ## Vascular Supply of the Scaphoid ```mermaid flowchart TD A[Scaphoid fracture]:::outcome --> B{Fracture location?}:::decision B -->|Distal pole| C[Anterograde blood supply intact]:::action B -->|Middle third| D[Variable blood supply]:::action B -->|Proximal pole| E[Retrograde supply only]:::urgent C --> F[Low AVN risk]:::outcome D --> G[Moderate AVN risk]:::outcome E --> H[High AVN risk 40-50%]:::urgent H --> I[Nonunion + AVN likely if immobilization fails]:::urgent I --> J{Diagnosis confirmed?}:::decision J -->|Yes| K[Surgical fixation + bone graft]:::action K --> L[Vascularized bone graft preferred]:::action ``` ## Clinical Features of Nonunion with AVN | Feature | Finding | |---------|----------| | **Radiographic sign** | Absence of callus at 12 weeks; sclerosis at fracture margins (AVN sign) | | **Symptoms** | Persistent pain, swelling, reduced grip strength | | **Mechanism** | Interrupted blood supply → bone necrosis → failure of healing | | **Risk factors** | Proximal pole location, displacement, delayed/inadequate immobilization | | **Incidence (proximal pole)** | 10–15% nonunion; 40–50% AVN | **Clinical Pearl:** The **sclerotic margins** seen on radiographs in AVN represent reactive bone formation around dead bone — a pathognomonic sign of established AVN. ## Management of Nonunion with AVN **Surgical fixation is indicated** when: 1. No callus formation after 12 weeks of immobilization 2. Proximal pole location (high AVN risk) 3. Symptomatic nonunion (pain, loss of function) 4. Radiographic evidence of AVN (sclerotic margins, cystic changes) ### Surgical Options 1. **Vascularized bone graft (VBG)** — **Gold standard** for proximal pole nonunion with AVN - Restores blood supply to necrotic bone - Union rates >90% - Sources: medial femoral condyle (MFC), distal radius (volar carpal artery pedicle) 2. **Non-vascularized bone graft** — For distal/middle third nonunion without AVN - Lower success rate if AVN present - Union rates 60–70% 3. **Percutaneous screw fixation** ± bone graft - Provides rigid fixation - Often combined with VBG for proximal pole 4. **Salvage procedures** (if nonunion persists despite VBG) - Scaphoidectomy with 4-corner fusion - Proximal row carpectomy - Wrist arthrodesis (last resort) **Mnemonic:** **PROX** — **P**roximal pole, **R**etrograde supply, **O**ccult AVN, **X** = eXcision or fusion if VBG fails. ## Why This Case Warrants Surgical Intervention 1. **Proximal pole location** — Highest AVN risk 2. **8 weeks immobilization without callus** — Nonunion is developing 3. **Persistent symptoms** — Functional deficit 4. **Radiographic evidence** — No bridging callus = failed conservative treatment **Warning:** Continuing immobilization beyond 12 weeks without callus formation is futile and delays definitive treatment. Vascularized bone graft has the best outcomes for proximal pole nonunion with AVN. 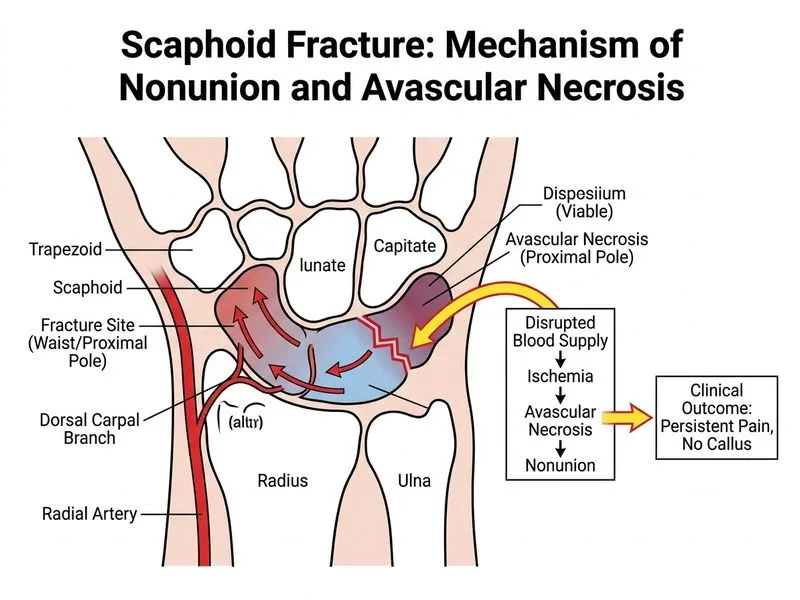
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.