## Clinical Presentation of Suspected Scaphoid Fracture **Key Point:** Scaphoid fractures present with a classic triad: (1) fall on outstretched hand (FOOSH), (2) tenderness in the anatomical snuffbox, and (3) pain on axial loading of the thumb (scaphoid compression test). ## Radiographic Findings in Acute Scaphoid Fracture **High-Yield:** Up to 25% of scaphoid fractures are **radiographically occult** on initial plain films, especially non-displaced or minimally displaced fractures. The fracture line may not be visible in the first 10–14 days due to minimal displacement and the complex anatomy of the scaphoid. ## Management Algorithm for Suspected Scaphoid Fracture ```mermaid flowchart TD A[FOOSH + Snuffbox tenderness + Scaphoid compression pain]:::outcome --> B{Plain radiographs show fracture?}:::decision B -->|Yes| C[Classify by location and displacement]:::action B -->|No| D{High clinical suspicion?}:::decision D -->|Yes| E[Immobilize in thumb spica cast]:::action D -->|No| F[Reassure and discharge] E --> G[Repeat radiographs in 10-14 days]:::action G --> H{Fracture now visible?}:::decision H -->|Yes| I[Continue immobilization based on type]:::action H -->|No| J[Consider MRI or CT if persistent symptoms]:::action C --> K[Determine treatment: cast vs surgery]:::action ``` **Clinical Pearl:** In a young, active patient with a clear mechanism of injury and classic clinical signs (snuffbox tenderness + scaphoid compression pain), **clinical diagnosis trumps initial radiographs**. Immobilization should not be delayed while waiting for imaging confirmation. **Mnemonic: FOOSH-SNAP** — **F**all **O**n **O**utstretched **S**hand → **S**nuffbox tenderness, **N**o fracture on X-ray, **A**lways immobilize, **P**icture again in 2 weeks. ## Why MRI or CT Immediately? **Warning:** While MRI is more sensitive (95–100%) for detecting occult fractures, it is **not the first-line next step** in uncomplicated suspected scaphoid fractures. MRI is reserved for: - Persistent symptoms after 2 weeks of immobilization with negative repeat radiographs - Need for urgent diagnosis in high-level athletes - Evaluation of complications (avascular necrosis, nonunion) CT is useful for **characterizing** a known fracture but is not indicated for screening occult fractures. ## Standard of Care The **gold standard approach** for clinically suspected but radiographically occult scaphoid fracture is: 1. Immobilize in a **thumb spica cast** (above-elbow or below-elbow depending on fracture location) 2. **Repeat radiographs in 10–14 days** — by this time, callus formation makes the fracture visible 3. If repeat films are negative and symptoms persist, proceed to MRI or CT [cite:Rockwood & Green's Fractures in Adults 9e Ch 8] 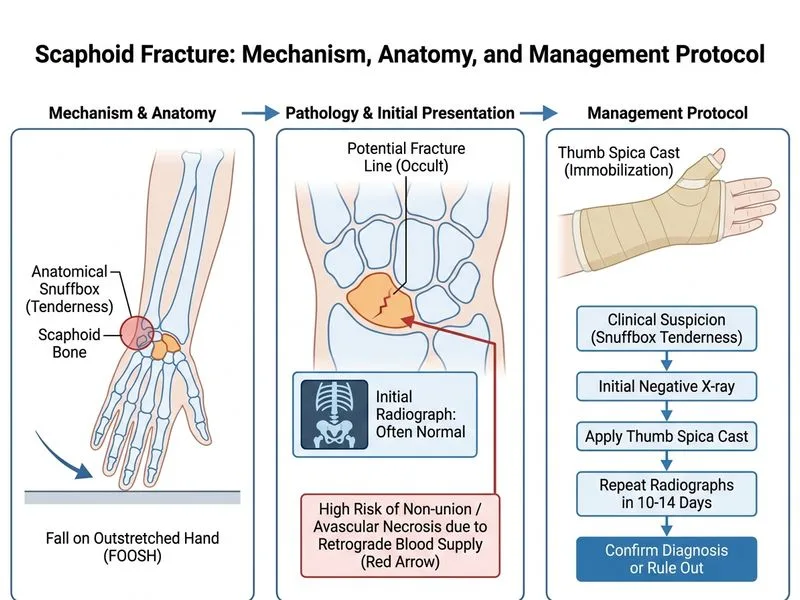
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.