## Classification and Location of Scaphoid Fracture **Key Point:** Scaphoid fractures are classified by **anatomical location** (proximal, middle/waist, distal) and by **displacement**. The waist is the most common site (60–70% of fractures) and has the highest risk of complications due to tenuous blood supply. ## Blood Supply and Healing Implications **High-Yield:** The scaphoid has a **retrograde blood supply** that enters through the distal pole and waist. Proximal pole fractures are at highest risk for avascular necrosis (AVN) because the proximal fragment may lose its blood supply entirely. Waist and distal fractures generally have better healing potential if immobilized adequately. ## Treatment Algorithm by Fracture Type and Displacement ```mermaid flowchart TD A[Scaphoid fracture confirmed]:::outcome --> B{Displaced or comminuted?}:::decision B -->|Yes| C[ORIF with scaphoid screw]:::action B -->|No| D{Location?}:::decision D -->|Distal third| E[Immobilization 6-8 weeks]:::action D -->|Waist| F[Immobilization 10-12 weeks]:::action D -->|Proximal third| G[Immobilization 12-16 weeks or ORIF]:::action E --> H[Repeat radiographs every 4 weeks]:::action F --> H G --> H H --> I{Union achieved?}:::decision I -->|Yes| J[Gradual mobilization]:::action I -->|No| K[Consider ORIF or other interventions]:::action ``` **Clinical Pearl:** Non-displaced scaphoid waist fractures are treated **conservatively with immobilization alone**. The duration depends on location: distal (6–8 weeks), waist (10–12 weeks), proximal (12–16 weeks). Regular radiographic follow-up every 4 weeks is essential to confirm union. ## Why Surgery Is NOT Indicated Here **Mnemonic: ORIF Indications = DISC** - **D**isplaced fracture (>2 mm) - **I**nstability or comminution - **S**egmental loss - **C**omplications (AVN, nonunion, malunion) This patient has a **non-displaced waist fracture** with no complications yet. She has only been immobilized for 4 weeks; waist fractures require 10–12 weeks total. Continuing immobilization with radiographic surveillance is the standard of care. ## Immobilization Duration by Location | Fracture Location | Immobilization Duration | Healing Rate | Complication Risk | |---|---|---|---| | **Distal third** | 6–8 weeks | 95–100% | Low | | **Waist** | 10–12 weeks | 85–95% | Moderate (AVN risk) | | **Proximal third** | 12–16 weeks | 60–80% | High (AVN risk) | **Warning:** Premature mobilization or discontinuation of immobilization in a waist fracture significantly increases the risk of nonunion and delayed union. The patient's continued pain is expected and does not indicate failure of conservative management. ## Monitoring for Complications **High-Yield:** During immobilization, watch for signs of: 1. **Nonunion** — fracture line remains visible on radiographs after 12 weeks 2. **Delayed union** — fracture line visible after 8 weeks but healing progresses 3. **Avascular necrosis** — sclerosis and collapse of proximal pole (more common in proximal fractures) If union is not achieved by 12 weeks, ORIF with a scaphoid screw becomes indicated. [cite:Rockwood & Green's Fractures in Adults 9e Ch 8; Campbell's Operative Orthopaedics 13e] 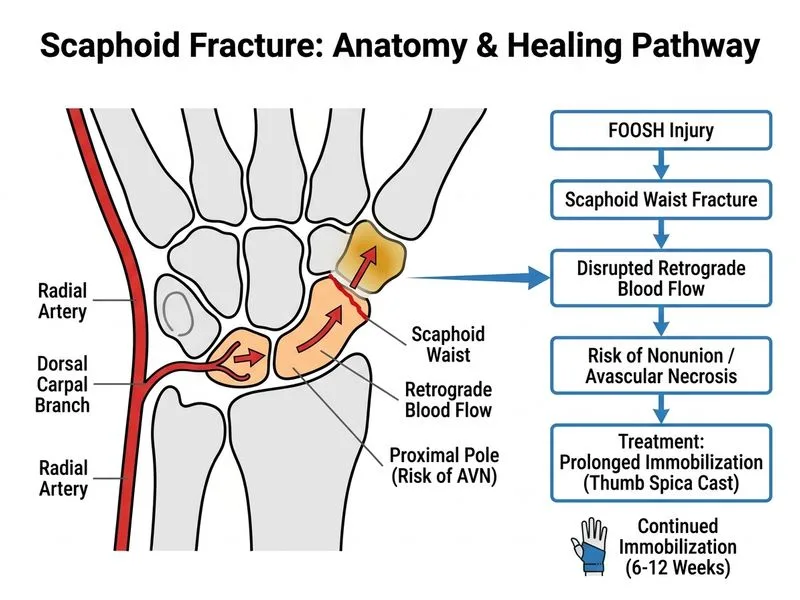
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.