## Diagnosis & Clinical Reasoning **Key Point:** This is acute septic arthritis (pyogenic arthritis) with a clear inoculation injury and classic synovial fluid findings. The Gram-positive cocci in clusters and clinical context strongly suggest *Staphylococcus aureus*. ## Diagnostic Criteria Met | Feature | Finding | Significance | |---------|---------|---------------| | **Synovial WBC** | 85,000/μL | >50,000 is highly suggestive of septic arthritis | | **Neutrophil %** | 95% | >90% supports bacterial infection | | **Glucose ratio** | 22 mg/dL (serum 110) | <50% serum glucose is typical for septic joint | | **Protein** | 6.2 g/dL | Elevated; reflects inflammation | | **Gram stain** | Gram+ cocci clusters | *S. aureus* pattern | | **Portal of entry** | Puncture wound | Direct inoculation 5 days prior | ## Why Arthroscopic Irrigation & Debridement? **High-Yield:** Septic arthritis is a **surgical emergency**. Purulent material must be drained completely to: 1. Relieve intra-articular pressure (prevents cartilage necrosis) 2. Remove bacteria and inflammatory mediators 3. Prevent permanent joint damage Arthroscopic approach is preferred over needle aspiration alone because: - Better visualization and complete evacuation - Allows assessment of cartilage damage - Lower recurrence rate ## Antibiotic Coverage **Clinical Pearl:** Empiric therapy must cover *S. aureus* (including MRSA risk) until culture/sensitivities return. - **Vancomycin** 15–20 mg/kg IV Q8–12H (for MRSA coverage) - **Ceftriaxone** 1–2 g IV Q12H (for Gram-negative and additional Gram-positive coverage) Once culture confirms *S. aureus* and sensitivities are known, can narrow to cefazolin if methicillin-sensitive. ## Timeline **Key Point:** Early intervention (within 24–48 hours of symptom onset) is critical to prevent irreversible cartilage damage and joint destruction. [cite:Robbins 10e Ch 26] 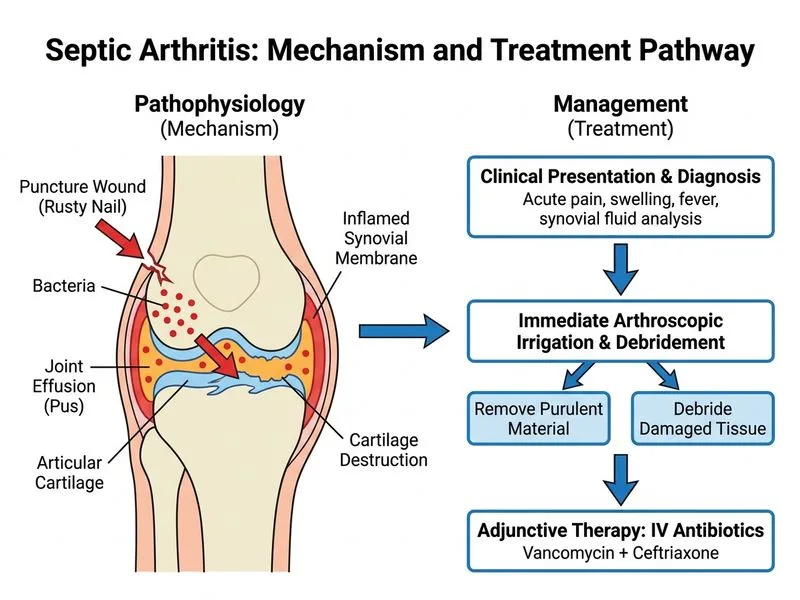
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.