## Clinical Assessment This patient presents with **septic shock** secondary to community-acquired pneumonia with sepsis-induced hyperglycemia and altered mental status. ### Key Diagnostic Features **High-Yield:** - Warm shock (warm skin, flushed appearance) with hypotension and tachycardia - Elevated lactate (4.2 mmol/L) indicating tissue hypoperfusion and anaerobic metabolism - SIRS criteria met: fever, tachycardia, tachypnea, elevated WBC - Persistent hypotension despite 2 L fluid resuscitation - Clinical context: fever, respiratory infection, bilateral infiltrates ### Shock Classification | Feature | Septic Shock | Hypovolemic | Cardiogenic | Anaphylactic | |---------|---|---|---|---| | Skin | Warm, flushed | Cold, clammy | Cold, clammy | Warm, urticarial | | Lactate | Elevated | Elevated | Elevated | Elevated | | Response to fluids | Often inadequate | Responsive | Worsens | Responsive | | Vasopressor need | Early | Late | Early | Rare | **Key Point:** Septic shock is defined as sepsis with persistent hypotension requiring vasopressors to maintain MAP ≥65 mmHg AND lactate >2 mmol/L despite adequate fluid resuscitation. ### Pathophysiology of Septic Shock 1. Bacterial endotoxin triggers TLR4 → NF-κB activation 2. Massive release of TNF-α, IL-1, IL-6 → capillary leak, vasodilation 3. Decreased systemic vascular resistance (SVR) and myocardial depression 4. Distributive shock: maldistribution of blood flow despite adequate CO 5. Microvascular thrombosis and tissue hypoxia → lactate accumulation ### Management Algorithm ```mermaid flowchart TD A[Sepsis suspected]:::outcome --> B[Fluid resuscitation:<br/>30 mL/kg crystalloid<br/>over first hour]:::action B --> C{BP ≥90/60 or MAP ≥65<br/>AND lactate normalized?}:::decision C -->|Yes| D[Continue antibiotics<br/>Source control<br/>Supportive care]:::action C -->|No| E[Initiate vasopressor:<br/>Noradrenaline first-line]:::action E --> F[Target MAP ≥65 mmHg<br/>Lactate clearance]:::action F --> G[Consider hydrocortisone<br/>if refractory shock<br/>after 1 hour]:::urgent ``` **Clinical Pearl:** The Surviving Sepsis Campaign (SSC) 2021 guidelines mandate vasopressor initiation when hypotension persists despite fluid resuscitation. Noradrenaline is the first-line agent due to its combined α-adrenergic (increases SVR) and β-adrenergic (maintains CO) effects. ### Why Noradrenaline? - **α-adrenergic effect:** restores SVR and perfusion pressure - **β-adrenergic effect:** maintains cardiac output (unlike pure α-agonists) - **Evidence:** SOAP II trial showed noradrenaline superior to dopamine in septic shock - **Dosing:** 0.01–0.5 μg/kg/min IV infusion, titrated to MAP target **Warning:** Do NOT delay vasopressor initiation waiting for a second fluid bolus if MAP remains <65 mmHg after adequate initial resuscitation. Further fluid in the presence of capillary leak may worsen pulmonary edema without improving perfusion. ### Adjunctive Measures (Not First-Line) - **Hydrocortisone:** Reserved for refractory septic shock (persistent hypotension despite 1 hour of vasopressors) — NOT initiated before vasopressors - **Echocardiography:** Useful if cardiogenic component suspected (history of MI, arrhythmia, murmur) — NOT indicated here given clear septic picture - **Second fluid bolus:** Already received adequate initial resuscitation; further bolus risks pulmonary edema **High-Yield:** Lactate clearance is a prognostic marker — failure to clear lactate within 6 hours predicts higher mortality and guides intensification of therapy. 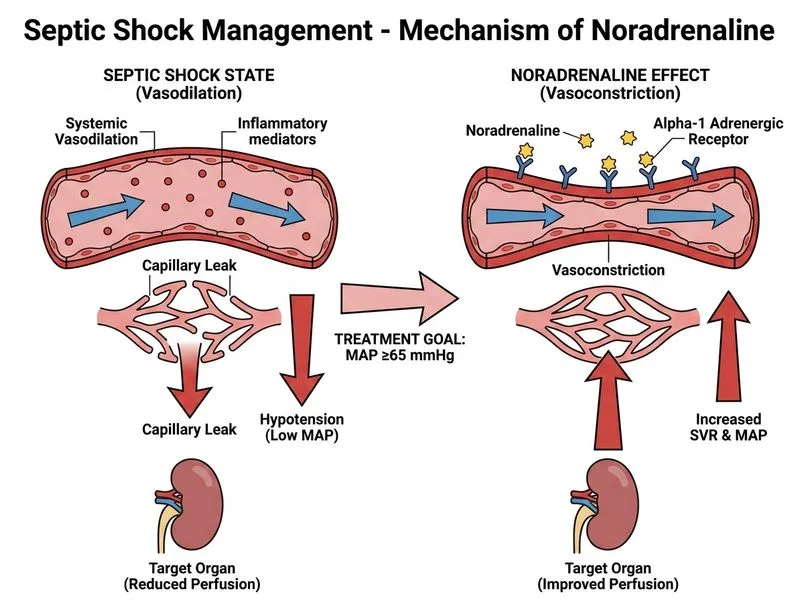
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.