## Clinical Diagnosis: Organophosphate Poisoning — Persistent Cholinergic Crisis ### Recognition of Cholinergic Crisis This patient presents with **acute organophosphate (OP) poisoning** causing a cholinergic toxidrome: pinpoint pupils, bronchospasm, salivation, lacrimation, bradycardia, and agitation — classic **SLUDGE + BBB** (Bradycardia, Bronchospasm, Bronchorrhea). **High-Yield:** The classic triad of OP poisoning: 1. **Muscarinic signs:** miosis, bronchospasm, salivation, lacrimation, bradycardia, urination, defecation 2. **Nicotinic signs:** muscle fasciculations, weakness, paralysis 3. **CNS signs:** agitation, anxiety, confusion, seizures ### Why Repeat Atropine Is the Correct Next Step **Key Point:** Atropine is the **primary and most urgent antidote** for OP poisoning. It competitively blocks muscarinic receptors, directly reversing bronchospasm, bradycardia, and secretions. The therapeutic endpoint is **drying of secretions and HR >80 bpm** — NOT pupil dilation. The patient received only **one dose of 2 mg atropine** 10 minutes ago and still has: - Active bronchospasm (RR 32, audible wheezing) - Bradycardia (HR 52) - Ongoing secretions Per standard toxicology guidelines (Goldfrank's Toxicologic Emergencies; WHO OP poisoning protocol), atropine should be **repeated every 5–10 minutes** in escalating doses (2–5 mg IV) until secretions dry. Severely poisoned patients may require **hundreds of milligrams** of atropine over hours. A single 2 mg dose is grossly insufficient for moderate-to-severe OP poisoning. | Drug | Mechanism | Priority | Dose | |------|-----------|----------|------| | **Atropine** | Muscarinic antagonist; blocks excess ACh at M receptors | **FIRST-LINE, immediate** | 2–5 mg IV q5–10 min, titrate to drying of secretions | | **Pralidoxime (2-PAM)** | Reactivates AChE before aging | Second-line, adjunct | 1–2 g IV over 15–30 min, then infusion | ### Why Pralidoxime Is NOT the Best "Next" Step Here **Clinical Pearl:** While pralidoxime (2-PAM) is an important adjunct in OP poisoning, its role as the *immediate next* intervention over repeat atropine is debated and not universally supported: 1. **Atropine is the primary antidote** — it directly and rapidly reverses life-threatening bronchospasm and bradycardia. Pralidoxime does not act fast enough to address the acute muscarinic crisis. 2. **Pralidoxime efficacy is controversial:** Multiple randomized controlled trials (including the landmark Sri Lanka trial, Eddleston et al., *Lancet* 2008) found no mortality benefit from pralidoxime in OP poisoning. WHO guidelines and many toxicology references now consider it an adjunct, not a replacement for atropine titration. 3. **The patient needs more atropine NOW:** Persistent bronchospasm and bradycardia after only one 2 mg dose means atropinization has not been achieved. The correct response is to repeat atropine immediately. 4. **Pralidoxime is given alongside atropine**, not instead of it — but the *next* step when atropine has not achieved its endpoint is **more atropine**. ### Why Each Other Option Is Wrong **Option A (Epinephrine for anaphylaxis):** Incorrect diagnosis. This is OP poisoning, not anaphylaxis. Epinephrine is not indicated and may worsen arrhythmias. **Option B (Intubation):** Premature. The patient is conscious and maintaining her airway. PaO₂ 65 mmHg with bronchospasm should respond to atropine. Intubation is reserved for respiratory failure refractory to medical therapy. Note: if intubation is needed, **avoid succinylcholine** (pseudocholinesterase inhibition prolongs paralysis); use rocuronium. **Option C (Pralidoxime):** An important adjunct but NOT the immediate next step when atropinization has not been achieved. Repeat atropine takes priority to control life-threatening bronchospasm and bradycardia. ### Management Algorithm 1. **Decontamination** — remove clothing, wash skin 2. **Atropine** 2–5 mg IV every 5–10 minutes → titrate to drying of secretions (endpoint: dry secretions, HR >80) 3. **Pralidoxime** 1–2 g IV over 15–30 min (adjunct, given alongside atropine) 4. **Benzodiazepines** for seizures 5. **Intubation** (with rocuronium) only if respiratory failure develops **Mnemonic:** **SLUDGE** (Salivation, Lacrimation, Urination, Defecation, GI upset, Emesis) + Bradycardia + Bronchospasm + Miosis = Organophosphate poisoning → Treat with **Atropine first, titrate aggressively**. *Reference: Goldfrank's Toxicologic Emergencies, 11th ed.; Eddleston et al., Lancet 2008; Harrison's Principles of Internal Medicine, 21st ed.* 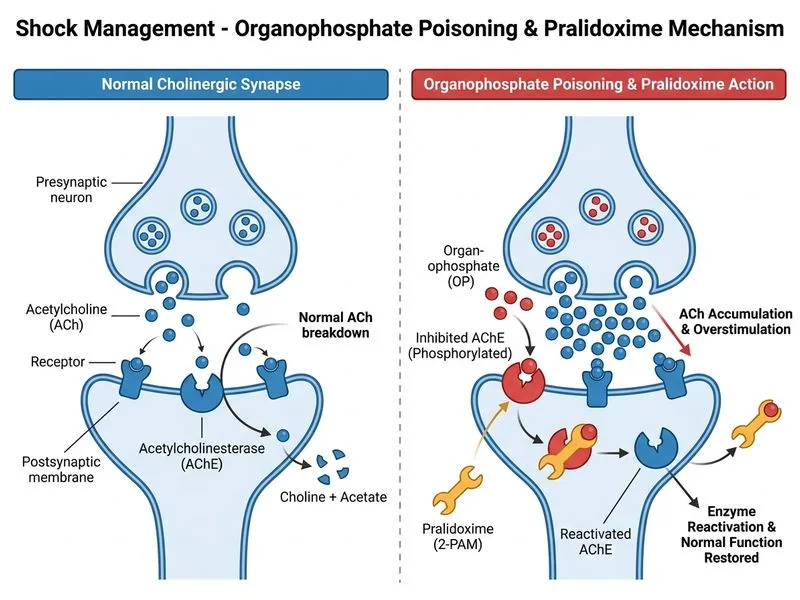
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.