## Clinical Diagnosis: Acute Pulmonary Embolism with RV Shock This patient presents with **massive pulmonary embolism (PE)** causing **right ventricular shock**: ### Key Diagnostic Features **High-Yield:** Classic triad of acute PE: 1. **Hypoxemia** (SpO₂ 88%) with clear lung fields 2. **Hemodynamic instability** (SBP 76 mmHg, HR 132, syncope) 3. **RV strain** on imaging (RV dilatation, D-shaped septum, RV dysfunction) **Clinical Pearl:** The elevated JVD + clear lungs + RV dilatation is pathognomonic for **RV failure from acute afterload increase** (PE), not left heart failure. ### Why This Is Massive PE - **Hemodynamic criteria**: SBP <90 mmHg = **shock** → massive PE - **Imaging**: RV dilatation + RV dysfunction = RV strain - **Troponin normal** (0.02): Does NOT exclude PE; troponin is insensitive for acute RV strain - **ECG**: Right axis deviation + V1–V3 T inversions = RV strain pattern ## Why Thrombolysis/Thrombectomy Is Correct **Key Point:** Massive PE with shock is a **Class I indication for thrombolysis or mechanical thrombectomy** [cite:ACC/AHA PE Guidelines 2019]. **Mechanism:** - Acute PE causes acute RV afterload increase → RV dilatation → septal shift → LV compression → cardiogenic shock - **Thrombolysis** dissolves clot, rapidly reduces RV afterload, restores RV output - **Mechanical thrombectomy** is alternative if contraindications to thrombolysis or failed thrombolysis **Dosing (Alteplase for PE):** - 100 mg IV over 2 hours (or 0.6 mg/kg if weight <65 kg) - Followed by unfractionated heparin (UFH) bolus 80 U/kg, then infusion **Why UFH over LMWH?** UFH is reversible (protamine) and has shorter half-life — critical if bleeding occurs post-thrombolysis. ```mermaid flowchart TD A[Acute PE suspected]:::outcome --> B[Confirm with CTPA/V-Q scan]:::action B --> C{Hemodynamically stable?}:::decision C -->|Yes| D[Anticoagulation alone]:::action C -->|No: SBP <90| E[Massive PE with shock]:::urgent E --> F{Contraindication to thrombolysis?}:::decision F -->|No| G[Thrombolysis: Alteplase 100 mg IV]:::action F -->|Yes| H[Mechanical thrombectomy]:::action G --> I[UFH bolus + infusion]:::action H --> I I --> J[Supportive care: O₂, vasopressor if needed]:::action J --> K[ICU monitoring]:::outcome ``` ## Why Other Options Are Wrong ### Fluid Bolus (500 mL NS) **Warning:** This is a **dangerous trap** in RV shock from PE. - **Pathophysiology**: In PE, the RV is already maximally dilated and operating on the flat part of the Starling curve - **Why fluid fails**: Additional preload does NOT increase RV output; instead, it worsens RV dilatation → further septal shift → LV compression → **decreased LV output and worsening shock** - **Correct approach**: RV shock from PE requires **afterload reduction** (thrombolysis), not preload increase - **Exception**: Fluid is only used if concurrent hypovolemia (e.g., bleeding) — this patient has no such history ### Dobutamine Infusion **Clinical Pearl:** Inotropes are **temporizing measures only** in PE shock and should NOT delay definitive therapy (thrombolysis). - **Why it fails**: Dobutamine increases contractility but does NOT reduce the underlying RV afterload (massive clot burden) - **Role**: May be used as **bridge to thrombolysis** if profound hypotension (SBP <70) requires temporary support - **This patient**: SBP 76 mmHg — thrombolysis is urgent; dobutamine alone is insufficient ### Inhaled Nitric Oxide + IV Epoprostenol - **Indication**: Chronic pulmonary hypertension or acute RV failure from **parenchymal lung disease** (ARDS, ILD) - **Why wrong here**: Inhaled NO and epoprostenol are **pulmonary vasodilators** — they reduce RV afterload but do NOT address the **mechanical obstruction** (clot) - **Mechanism failure**: Vasodilation alone cannot overcome a massive PE; thrombolysis is required - **Role in PE**: These agents may be used **adjunctively** post-thrombolysis if residual pulmonary hypertension persists ## Management Algorithm for Massive PE | Step | Timing | Action | |------|--------|--------| | Immediate | 0–5 min | O₂ to target SpO₂ >90%, IV access, continuous monitoring | | Urgent | 5–15 min | **Thrombolysis** (Alteplase 100 mg IV) OR **mechanical thrombectomy** | | Concurrent | 5–15 min | UFH bolus 80 U/kg, then infusion (target aPTT 1.5–2.5× control) | | Supportive | As needed | Vasopressor (noradrenaline) if SBP <70 despite thrombolysis | | Monitoring | Continuous | ICU, serial troponin, RV function reassessment | **Mnemonic: MASSIVE PE = Mortality reduction = Mechanical thrombolysis (or alteplase)** ## Key Differentiator: RV Shock vs. LV Shock | Feature | RV Shock (PE) | LV Shock (MI) | |---------|---------------|---------------| | JVD | ↑↑ (elevated) | Normal or low | | Lung fields | Clear | Crackles/pulmonary edema | | RV on echo | Dilated, dysfunctional | Normal | | Fluid response | Worsens shock | Improves shock | | Treatment | Thrombolysis/thrombectomy | Revascularization | **High-Yield:** **Clear lungs + elevated JVD + shock = think PE, not cardiogenic shock from MI.** 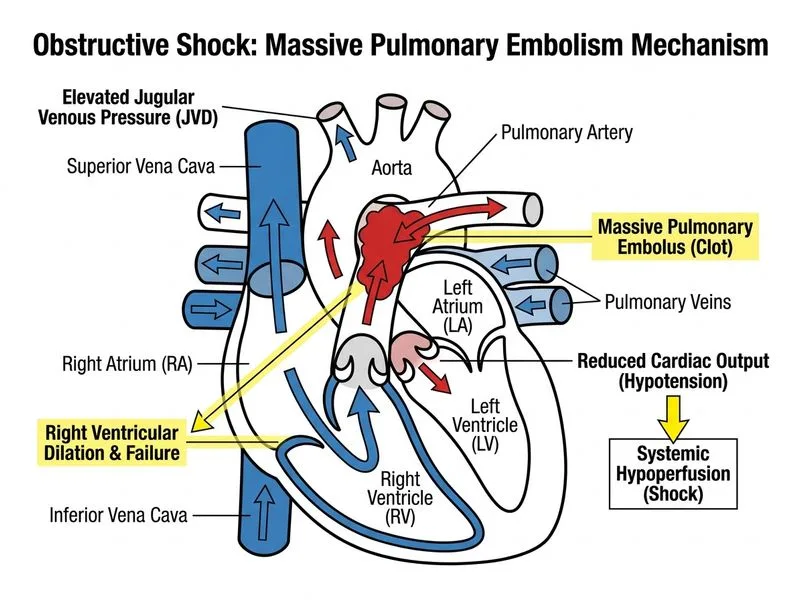
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.