## Clinical Context This patient presents with **septic shock** secondary to community-acquired pneumonia (CAP). The diagnostic criteria are met: infection (fever, pneumonia on imaging), systemic inflammation (elevated WBC, procalcitonin), hypotension refractory to fluid resuscitation, and tissue hypoperfusion (elevated lactate >4 mmol/L, tachycardia). ## Septic Shock Definition & Management Hierarchy **Key Point:** Septic shock is defined as sepsis with persistent hypotension requiring vasopressors to maintain MAP ≥65 mmHg AND elevated lactate (>2 mmol/L) despite adequate fluid resuscitation [cite:Surviving Sepsis Campaign 2021]. ### Fluid Resuscitation Phase (Already Done) The patient has received 2 L crystalloid bolus (approximately 30 mL/kg for a 70 kg patient is the target), yet remains hypotensive with elevated lactate. This indicates **fluid-refractory shock**. ### Vasopressor Initiation Criteria | Criterion | Status in This Patient | | --- | --- | | Sepsis confirmed | ✓ Yes (fever + pneumonia + SIRS) | | Hypotension (SBP <90 or MAP <65) | ✓ Yes (BP 92/56 → MAP ~68, borderline) | | Adequate fluid resuscitation attempted | ✓ Yes (2 L bolus given) | | Persistent hypotension/tissue hypoperfusion | ✓ Yes (lactate 4.2, tachycardia) | **High-Yield:** Norepinephrine is the **first-line vasopressor** in septic shock. It provides both α-adrenergic (vasoconstriction) and β-adrenergic (inotropic) effects, maintaining systemic vascular resistance and cardiac output simultaneously [cite:Harrison 21e Ch 295]. ## Why Norepinephrine Over Alternatives? **Mnemonic: NOREPI-FIRST** — **N**orepinephrine is **O**ptimal, **R**educes **E**piphrine need, **P**reserves **I**notropism, **F**irst-line **I**n **R**efractory **S**epsis, **T**argeting **MAP** ≥65. - **Norepinephrine:** α > β effect; increases SVR and cardiac output; mortality benefit in septic shock - ~~Epinephrine~~ (second-line if norepinephrine inadequate; higher arrhythmia risk) - ~~Dopamine~~ (arrhythmogenic, not recommended as first-line in sepsis) - ~~Phenylephrine~~ (pure α-agonist; reduces cardiac output; reserved for specific scenarios) ## Concurrent Measures 1. **Antibiotics:** Broad-spectrum coverage (e.g., ceftriaxone + azithromycin or fluoroquinolone for CAP) should be started within 1 hour of recognition of sepsis. 2. **Source control:** Imaging (CXR done) and clinical assessment for drainage needs. 3. **Lactate monitoring:** Serial lactate is a prognostic marker; clearance indicates improving tissue perfusion. 4. **Reassess fluid status:** Avoid over-resuscitation (risk of ARDS, pulmonary edema). ## Clinical Pearl In this patient, the lactate of 4.2 mmol/L despite fluid resuscitation is the key trigger for vasopressor initiation. Lactate >4 mmol/L in sepsis correlates with increased mortality and indicates anaerobic metabolism from inadequate tissue perfusion—a problem that crystalloid alone cannot solve. Vasopressors restore perfusion pressure. 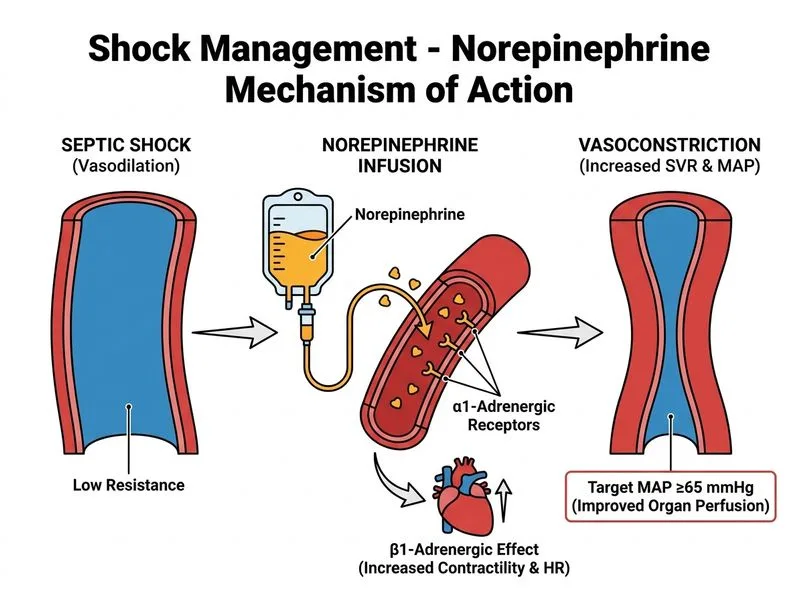
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.